BK101
Knowledge Base
Vaccinations - Infections - Viruses - Colds - Flu
Vaccines Explained - Colds - Covid - Viruses - Flu - Pandemic - Diseases - Antibiotics - Infection
You have the right to refuse a vaccine or say no to a vaccine when you have valid reasons that are based on facts. But if you are seeking a fake exemption or if you're an Anti-Vaxxer who does not have valid reasons, then your ignorance may be a threat to other people and not just a threat to yourself. You need to explain the exact vaccine that you're taking about? You have to know who is the individual receiving the vaccine and why the individual needs the vaccine and what the vaccine is for? You have to know what are the risks for receiving the vaccine as well as the risks you are taking if you do not receive the vaccine, which is best explained using facts, numbers, proof and confirmed evidence. You don't want to look like nut job or a raving maniac who needs to be in a mental health facility. But for some reason, morons can have a voice, just like some of the people on Fox News, who are extremely dangerous terrorists that threaten the well being and mental health of innocent people all over the world. This behavior is totally irresponsible and unwarranted.
Human Rights - Exemptions - Right to Try - Number Needed to Treat - FDA
We know that most people are not against vaccines, because most vaccines are beneficial. But people do have concerns. So people need a clear understanding of the reasons why they need a particular vaccine and know how much they need and when? People also need to know all the ingredients that are in the vaccine? People have the right to know the facts and understand their choices and the effectiveness of certain vaccines.
Consent - Permission - Educated Decision
Consent is having permission to do something or have access to personal information. To give an affirmative reply or response that gives your approval.
Implied Consent is consent which is not expressly granted by a person, but rather implicitly granted by a person's actions and the facts and circumstances of a particular situation. In some cases, a person's silence or inaction is the same as saying yes.
Informed Consent is having a clear understanding of the facts, implications, risks, and the consequences of an action. When you're fully informed, you can give legal and logical permission to someone before they conduct a healthcare intervention on you. Informed consent is the process in which a health care provider educates a patient about the risks, benefits, and alternatives of a given procedure or intervention. The patient must be competent to make a voluntary decision about whether to undergo the procedure or intervention.
Two Party Consent Law states under Penal Code § 632, which means you must get consent of all parties before using any recording device to capture a confidential communication, including a cell phone.
Personal Rights - Liberty - Sovereignty - Free Will - Mentally Able - Informed - Decision - Mature - My Body My Choice - No means No - Unconstitutional - Transparency - Fine Print - Disclaimer - Opt Out - Effectiveness - Entrapment - False Evidence - Conscientious Objector - Passive - Accessory to a Crime - Involuntary Servitude - Conformity Dangers - Engineering Consent
Full Disclosure is to fully disclose evidence of proven factual information gathered and presented to an individual or group. And the acknowledgement of possible conflicts of interest in one's work.
Pretending to understand something can be extremely dangerous.
Involuntary Treatment refers to medical treatment undertaken without the consent of the person being treated. Involuntary treatment is permitted by law in some countries when overseen by the judiciary through court orders; other countries defer directly to the medical opinions of doctors. In medical ethics, involuntary treatment is conceptualized as a form of parens patriae whereby the state takes on the responsibilities of incompetent adults on the basis of the duty to protect and the duty of beneficence (the duty of the state to repair the random harms of nature).
Ginny Pigs - Big Pharma - Drug War
Silence Procedure states that "he who is silent is taken to agree", "silence implies/means consent") is a way of formally adopting texts, often, but not exclusively in international political context.
Asking Questions - Consumer Warnings - Hospital Infections - Number Needed to Treat
Consent of the Governed refers to the idea that a government's legitimacy and moral right to use state power is only justified and lawful when consented to by the people or society over which that political power is exercised. This theory of consent is historically contrasted to the divine right of kings and had often been invoked against the legitimacy of colonialism. Article 21 of the United Nation's 1948 Universal Declaration of Human Rights states that "The will of the people shall be the basis of the authority of government".
Consent Form is a form signed by a patient prior to a medical procedure to confirm that he or she agrees to the procedure and is aware of any risks that might be involved. The primary purpose of the consent form is to provide evidence that the patient gave consent to the procedure in question.
Authorization is a document giving an official instructions, permission or approval.
Permission is the act of giving a formal or written authorization that gives approval for someone to do something.
Dissent is non-agreement or opposition to a prevailing idea. Strawman.
Compliance in psychology refers to a response—specifically, a submission—made in reaction to a request. Defined as the effect that the words, actions, or mere presence of other people (real or imagined) have on our thoughts, feelings, attitudes, or behavior; social influence is the driving force behind compliance. It is important that psychologists and ordinary people alike recognize that social influence extends beyond our behavior—to our thoughts, feelings and beliefs—and that it takes on many forms. Persuasion and the gaining of compliance are particularly significant types of social influence since they utilize the respective effect's power to attain the submission of others. Studying compliance is significant because it is a type of social influence that affects our everyday behavior—especially social interactions. Compliance itself is a complicated concept that must be studied in depth so that its uses, implications and both its theoretical and experimental approaches may be better understood. Military Draft - Doctrine.
If everyone signs non-disclosure agreements, then how will the public be informed of negligence and abuse? Companies are using non-disclosure agreements to get away with committing crimes and to silence victims of crimes, allowing the criminals to keep committing more crimes.
You have the Right to Remain Silent, but sometimes you have to speak and be heard. And if you want to be understood, you have to learn some things first in order to know how to explain the injustice that you are trying to inform people about. You don't want to sound like a raving lunatic or sound like those small talkers in the media who explain very little, because that will end up just spreading ignorance like a disease.
To say that most people except things in society is a lie. Most people are not informed enough about their decisions or their choices. Most people don't even except their own ignorance because they have no idea about the things they are ignorant about. This is why informed consent is extremely important, but not more important than improving education. Being passive or being a blind follower is a result of a dumbed down education.
Consent to Operate is a certificate that is needed by the manufacturers when the industry is established and is ready to operate, as per the stipulated norms under the Water Act and the Air Act, which is mandated by the Central Pollution Control Board guidelines that no proposed industry is allowed within the approved residential area stipulated by Municipal Corporation. No orange or red category industries must be established within the municipal corporation limits barring the industrial areas/zone. The Air and Water Act also stipulates the punishment for producers if any industry falling into green/orange or red is functioning without obtaining consent from State Pollution Control Board. The punishment prescribed under the act is imprisonment for a term which may extend to 3 months or a fine which may extend to ten thousand rupees or both. The manufacturer or the owner of the industry is held legally responsible for the punishment. Documents required to obtain Consent to Operate are: Health Trade License, Factory/Trade License, Authorisation Letter, Pan Card and the Aadhar Card, Municipality or Industry License, Proof of Registration of unit, Site Plan, Water Bill, GST certificate, Environmental Statement (form-V), CA Letter on the total price of the plan, FSSAI Certificate (in case of a food-related business), Electricity Bill, Proof of ownership.
Consent to Establish requires registering through the Online Consent Management and Monitoring System of the concerned State Pollution Control Boards. The application to be uploaded should have all the mandatory info along with the documents required to be enclosed with the application. This is followed by a mandatory inspection of the unit by the official personnel of the State Pollution Control Board/Pollution Control Committee. After the assessment of the manufacturing unit and authorization of the respective committee, the decision for authorization is taken. Further, under the process of describing Consent To Operate v/s Consent To Establish, if the producers or manufacturers cannot establish the industry within the obligatory time, the manufacturer is instructed to register for the leeway of the certificate one month after the expiration of the certificate. The certificate will be delivered after the authorized officer has finished his inspection.
Opting Out by Default
Op Out should be by default, and you should only Opt In when you want to give someone permission, someone that you trust. And you should only opt in when you fully understand the risks and the benefits. The default option is the option the chooser will obtain if he or she does nothing.
Passive - Consent - You Vote Everyday - Not to Choose is to Choose - Procrastination - I Don't Feel like Doing it
Opt-Out Systems in organ donation will occur automatically unless a specific request is made before death for organs not to be taken. So anyone who has not refused consent to donate is a donor. If you don't refuse consent, then you give consent. If you don't say anything, then someone will assume that you said yes. A presumed consent system, it is assumed that individuals do intend to donate their organs.
Default Effect is the option the chooser will obtain if he or she does nothing. Broader interpretations of default options include options that are normative or suggested. Experiments and observational studies show that making an option a default increases the likelihood that it is chosen; this is called the default effect. Different causes for this effect have been discussed. Setting or changing defaults therefore has been proposed as an effective way of influencing behavior—for example, with respect to deciding whether to become an organ donor, giving consent to receive e-mail marketing, or choosing the level of one's retirement contributions.
By Default is an option that is selected automatically unless an alternative is specified. You choose, or you lose your ability to choose, and someone else chooses for you. Default is lossing because you did not show up. A loss resulting from failure to do something. Default in computing is when a person assumes a particular value when none other is specified.
Public Health Insurance Option is a proposed alternative health insurance plan offered by the government that would compete with other private health insurance companies within the United States.
Negative Option Billing is a business practice in which customers are given goods or services that were not previously ordered, and must either continue to pay for the service or specifically decline it in advance of billing. According to the Federal Trade Commission, unsolicited goods are considered a gift, and the recipient is not required to pay for or return them. This is different than situations where a customer signs up for a service or club without reading fine print and agrees to purchase goods through the mail. negative option billing is the model on which mail order services, such as Columbia House, and other book clubs are structured.
Exemptions - Reasons
Religious Exemption is when some parents or people either use fake religious adherence or invent fake religions in order to get an exemption that is not based on facts or science. Although exemptions vary from state to state, all school immunization laws grant exemptions to children for medical reasons. Almost all states grant religious exemptions for people who have religious beliefs against immunizations. There are almost no religions that object to vaccinations. We have a strong tradition of protecting the freedom of religion in our country, as we should. The First Amendment specifically guarantees that the government cannot prohibit “the free exercise” of religion. In plain English, that means every individual has the right to hold their own religious beliefs and to engage in actions or practices in support of those religious beliefs without government intrusion. The Supreme Court has acknowledged it would be absurd to allow people to opt out of many generally applicable laws by simply claiming their religious beliefs compelled contrary action, especially when that would actually harm the rule of law, public safety and general welfare. Contradictions.
Religious Charlatans - Above the Law - Immunity - Privileged - Invalid Arguments - Draft Exemptions - Law is Debatable - Truth is Debatable - Separation of Church and State
Religious Fundamentalism, delusions, and conspiracy beliefs related to the COVID-19 Pandemic.
Exception is the act of excepting something or excluding something because it does not fall under the current rule or the intended meaning of a law. An instance that does not conform to a rule or generalization. A special case to which a rule does not apply. A person or thing that is excluded from a general statement or does not follow a rule.
It is not a valid defense to a crime to cite a religious belief or religiously imposed duty. Reynolds v. United States, 98 U.S. 145 (1878). But I have a right to defend myself if I do have valid reasons. We know the government can sometimes impose regulations, even if those regulations burden actions taken in furtherance of religious beliefs. But when? The Supreme Court concluded in 1940, “Conduct remains subject to regulation for the protection of society.”
Employment Div. v. Smith, 494 U.S. 872 (1990). A law is constitutional under the Free Exercise Clause if it is facially neutral and generally applied. Respondents Smith and Black were fired by a private drug rehabilitation organization because they ingested peyote, a hallucinogenic drug. Their applications for unemployment compensation were denied by the State of Oregon under a state law disqualifying employees discharged for work-related "misconduct." Right to Try.
Religious Freedom Restoration Act of 1993 (1993). Congress adopted the Religious Freedom Restoration Act of 1993 to override the Supreme Court decision in Employment Division, Department of Human Resources of Oregon v. Smith (1990) and provide greater protection under the First Amendment free exercise clause.
There Needs to be Exemptions because individuals can have special needs and unique requirements and vulnerabilities. People have a right to legally defend themselves, even against the government. But a person must have the right to explain their case and have a right to a fair trial. The drug war and prohibition is just two examples of corrupt government overreach. Vulnerabilities.
Medical Exemptions: All 50 states allow exemptions for children who have a valid medical reason, and almost all states allow nonmedical exemptions for parents with either religious or philosophical objections. Antibodies.
Medical Exemption is an exception to compulsory school immunization laws, based upon a medical condition. According to the Centers for Disease Control and Prevention (CDC), all 50 states allow school children to be exempted from vaccination requirements for medical reasons.
California Gov. Gavin Newsom signed bills on Monday September 10th 2019 to crack down on doctors who write fraudulent medical exemptions for school children's vaccinations. The bill, SB 276, aims to crack down on bogus medical exemptions.
Legitimate is something based on known statements, events or conditions. In accordance with recognized or accepted standards or principles. Something that is authorized or sanctioned by experts, or in accordance with law or conforming to the law or to rules. Justified.
Excuse is a reason which you give in order to explain why something has been done or has not been done, or in order to avoid doing something.
When the government forces people to take vaccines, and also threatens people who don't comply, and at the same time, the government offers no alternatives, no options, no health advice, or offers tests that would help verify immunity or vulnerability, and instead of just testing people for a negative or positive covid result, all I can think about is Jonestown. People are being setup to take the real poison in the future. We know that history repeats itself, mostly because schools never teach people the truth about history, or do people learn the facts about their world that would help protect them from the ignorance of corrupted individuals. When people show how gullible and naive they are, there will always be criminals ready to exploit them. Booster shot? The only thing that they're boosting is peoples concern. And now they're going after children. If the covid-18 vaccine is 91% effective at preventing symptomatic infection in young children, does this mean that children will be infected and not know it, thus spreading the virus even more? If the covid-19 vaccine for children would help prevent hospitalizations and death from COVID-19, that would only be for children who are the most vulnerable? Which means that majority of children should not be vaccinated. This makes it seem like the zombie apocalypse is upon us. The corporate controlled government and the corporate controlled media are now using the words efficacy and effectiveness to manipulate the truth and to blur the facts. Science has been abandoned and replaced with propaganda, which is nothing new. These corporate puppets are more concerned with protecting profits than they are with protecting people. When they say 90% effective, you should ask, effective against what? Effective against getting the virus, or effective against spreading the virus? Effective against being hospitalized because of the virus or effective against dying from the virus? And exactly who is being protected the most from this vaccine? Is it the majority of the millions of people who never get sick or show symptoms, or is it just the most vulnerable people who are a small percentage of the population? And just how did you determine this efficacy rate? Were the participants of the study hand picked? And what were the requirements of these handpicked individuals?
Effectiveness - Efficacy
Efficacy is the ability to produce a desired or intended result. Efficacy is the capacity or the power to produce a desired effect. Vaccine efficacy is the relative reduction in the risk or risk benefit ratio. Efficacy is a measurement made during a clinical trial. The people who join clinical trials are not a perfect reflection of the population at large, and the results can be easily skewed to make misleading claims.
Effectiveness is the quality of being able to bring about an effect. Effectiveness is how well the vaccine works out in the real world. Efficiency.
Effective is producing or capable of producing an intended result or having a striking effect. Able to accomplish a purpose.
Biological Plausibility is one component of a method of reasoning that can establish a cause-and-effect relationship between a biological factor and a particular disease or adverse event. It is also an important part of the process of evaluating whether a proposed therapy, drug, vaccine or surgical procedure, has a real benefit to a patient. This concept has application to many controversial public affairs debates, such as that over the causes of adverse vaccination outcomes. Biological plausibility is the proposal of a causal association—a relationship between a putative cause and an outcome—that is consistent with existing biological and medical knowledge.
Why are flu vaccines only about 60 Percent Effective? If that's the case, then education is more effective than vaccines. The vaccine does not protect you from spreading the virus, it only gives you a 60% chance of not getting sick from a certain virus. The flu vaccine is an educated guess.
Seasonal flu vaccinations don't 'stick' long-term in bone marrow. Contrast to childhood vaccinations. Seasonal flu vaccination does increase the number of antibody-producing cells specific for flu in the bone marrow. However, most of the newly generated cells are lost within one year, researchers found.
Comparative Effectiveness Research - Repeatability - Pros and Cons - Cancer Treatments
Unlike vaccines for measles or polio that work more than 90 percent of the time, the new Malaria Vaccine has an efficacy rate between 26 and 36 percent.
The Cutter Incident: How America's First Polio Vaccine Led to a Growing Vaccine Crisis. In April 1955 more than 200,000 children in five Western and mid-Western USA states received a polio vaccine in which the process of inactivating the live virus proved to be defective. Within days there were reports of paralysis and within a month the first mass vaccination program against polio had to be abandoned. Subsequent investigations revealed that the vaccine, manufactured by the California-based family firm of Cutter Laboratories, had caused 40,000 cases of polio, leaving 200 children with varying degrees of paralysis and killing 10.
Cutter Laboratories was a family-owned pharmaceutical company located in Berkeley, California, founded by Edward Ahern Cutter in 1897. Cutter's early products included anthrax vaccine, hog cholera (swine fever) virus, and anti-hog cholera serum—and eventually a hog cholera vaccine. The Bayer pharmaceutical company bought Cutter Laboratories in 1974. Biofilm.
SV40 is an abbreviation for simian vacuolating virus 40 or simian virus 40, a polyomavirus that is found in both monkeys and humans. Like other polyomaviruses, SV40 is a DNA virus that sometimes causes tumors in animals, but most often persists as a latent infection. SV40 has been widely studied as a model eukaryotic virus, leading to many early discoveries in eukaryotic DNA replication and transcription.
Number Needed to Treat - Number Needed to Educate
Number Needed to Treat is the average number of patients who need to be treated to prevent one additional bad outcome. e.g. the number of patients that need to be treated for one to benefit compared with a control in a clinical trial. NNT is the effectiveness of a health-care intervention, typically a treatment with medication. If people are harmed more than they are helped by a drug, then you need to understand why. If the benefits outweigh the risks, or if the risks outweigh the benefits, then you need to understand why. Viruses can be devious, especially language viruses.
Number Needed to Harm is an average of one patient who would not otherwise have been harmed. Risk Benefit Ratio.
Number Needed to Vaccinate states that the number of people needed to be vaccinated is sometimes small. So vaccinating more people does not make people safer, especially when the vaccination may have the potential to do more harm then good if given to more people than needed. Protecting the most vulnerable people is a priority, but there is still risks involved.
Effect Size is a quantitative measure of the strength of a phenomenon. Examples of effect sizes are the correlation between two variables, the regression coefficient in a regression, the mean difference, or even the risk with which something happens, such as how many people survive after a heart attack for every one person that does not survive. For each type of effect size, a larger absolute value always indicates a stronger effect. Effect sizes complement statistical hypothesis testing, and play an important role in power analyses, sample size planning, and in meta-analyses. They are the first item (magnitude) in the MAGIC criteria for evaluating the strength of a statistical claim.
Herd Immunity occurs when a large percentage of a population has become immune to an infection, thereby providing a measure of protection for individuals who are not immune. But just being immune does not mean you or someone else can't be a carrier of an infectious disease.
Poor quality food, poor quality water, poor quality air, and a poor quality education all contribute to disease vulnerabilities. Viruses can be Devious - Brain Hacking.
Number Needed to Educate. Humans need Herd Immunity from Ignorance. So what is the percentage of a population that would help people to be immune from the actions of ignorant people or immune from propaganda? It only takes a few ignorant people to cause damage and increase the vulnerabilities of the whole herd. Ignorance does not discriminate. Most people are extremely vulnerable to the horrible effects that ignorance brings. The best inoculation is education, and a commitment to life long learning that will help people to be protected from the ignorance-virus that has infected millions of people. There are a lot of parasites in the world. And ignorance is a communicable disease. Having enough valuable knowledge and information can help people to be immune to almost every disease in the world. Knowledge is the cure because it helps prevent a lot of mistakes that people can make. You need protection from viruses of the mind. The mind needs protection from the corrupting influences of power, from the corrupting influences of money, and from the corrupting influences of fame.
Vaccine helps to build up anti-bodies so that people can defend themselves against virus's. We need a vaccine to help people guard themselves against ignorance and corruption. We will call it a Real High Quality Education Vaccine, or an inoculation against ignorance. This way when children grow up, they will have enough knowledge and skills and anti-bodies to defend themselves, and others, from corruption, abuse, waste and other crimes that kill millions every year. It's not just the lack of a vaccine that will kill you, it's the lack of knowledge about how to protect yourself from a particular disease that will kill you. A vaccine can help replace education where there is very little education, which happens to be the entire planet. You will save more people by educating them, then you will by injecting them, especially if the injection is mostly propaganda. Education is the only proven vaccination for ignorance, which kills more people then all diseases combined.
New research reveals psychological 'booster shots' can strengthen resistance to misinformation over time. A new study has found that targeted psychological interventions can significantly enhance long-term resistance to misinformation. Dubbed 'psychological booster shots,' these interventions improve memory retention and help individuals recognize and resist misleading information more effectively over time. The research team tested three types of misinformation-prevention methods: Text-based interventions, where participants read pre-emptive messages explaining common misinformation tactics. Video-based interventions, short educational clips that expose the emotional manipulation techniques used in misleading content. Gamified interventions, an interactive game that teaches people to spot misinformation tactics by having them create their own (fictional) fake news stories in a safe, controlled environment.
Silent Pandemic of Ignorance has reared it's ugly head. The Silent Pandemic of Obesity refers to the widespread and growing problem of obesity around the world, often considered a hidden crisis because it can develop gradually without noticeable symptoms, but still poses significant health risks due to its link to chronic diseases like diabetes, heart disease, and certain cancers; essentially, the term highlights the seriousness of obesity despite not always being readily apparent as a major health concern. The Silent Epidemic of lifestyle-related diseases that rob many individuals of their health and life itself. A Silent Disease is a medical condition that does not exhibit noticeable symptoms in its early stages, earning it the moniker of “silent killer.” Early detection and prevention are key, so it's important to be aware of these diseases. A disease spreading without symptoms for a prolonged period before it is detected can kill millions, like with antimicrobial resistance, when bacteria, viruses, fungi, and parasites stop responding to medication.
BK101 is the silver bullet, the magic bullet, the magic wand, the antidote. Silver Bullet is a simple and seemingly magical solution to a complicated problem. Bullet made of Silver is used in fiction as a supposedly magical method for killing werewolves. Magic Bullet is something that cures or remedies without causing harmful side effects. Waving a Magic Wand is to provide the perfect solution to a given problem or difficulty, as if by magic. Antidote is a substance that can counteract a form of poisoning.
Isolation (Number Needed to Isolate) - Social Distancing - Pandemic
Asymptomatic Carrier is a person or other organism that has contracted an infectious disease, but who displays no symptoms. Although unaffected by the disease themselves, carriers can transmit it to others.
Basic Reproduction Number the expected number of cases directly generated by one case in a population where all individuals are susceptible to infection. The definition describes the state where no other individuals are infected or immunized (naturally or through vaccination). The most important uses of R0 are determining if an emerging infectious disease can spread in a population and determining what proportion of the population should be immunized through vaccination to eradicate a disease. The basic reproduction number is affected by several factors including the duration of infectivity of affected patients, the infectiousness of the organism, and the number of susceptible people in the population that the affected patients are in contact with.
Infection Rate is the probability or risk of an infection in a population. It is used to measure the frequency of occurrence of new instances of infection within a population during a specific time period. Wash Hands.
Case Fatality Rate is the proportion of deaths from a certain disease compared to the total number of people diagnosed with the disease for a certain period of time. A CFR is conventionally expressed as a percentage and represents a measure of disease severity. CFRs are most often used for diseases with discrete, limited time courses, such as outbreaks of acute infections. A CFR can only be considered final when all the cases have been resolved (either died or recovered). The preliminary CFR, for example, during the course of an outbreak with a high daily increase and long resolution time would be substantially lower than the final CFR.
Risk - Potential Side Effects
Vaccines are not Risk Free. But if you don't know the risks, then how can you decide? How do you minimize risk without increasing risk for yourself or for others.
Risk Benefit Ratio - Side Effects - Interactions
Viral Contaminated Vaccines. Vaccines produced using infected cell cultures could lead to seroconversion. Vaccine Contaminants.
Premature Launch of Dengue Fever Vaccine Dengvaxia has Deadly Repercussions. Out of 1 million kids in the Philippines, the vaccine would cause about 1,000 to be hospitalized over five years, but on the other hand, the vaccine would prevent about 12,000 hospitalizations for a new dengue infection in children who have had a prior dengue infection during this same time period. That's not an acceptable risk. A risk needs to be exceedingly small to be tolerated. For example, with the measles vaccine, the risk of encephalitis is about 1 in 1 million, or 1,000 times less than the risk from a measles infection, the vaccine is safe only for children who have had a prior dengue infection. In some instances children were given the vaccine by untrained health workers and allegedly without a proper physical beforehand. Some children allegedly had preexisting medical conditions that made the immunization dangerous. But these children were still inoculated, officials were also indicted for not properly helping children who had serious reactions to the shot. the confidence in vaccines among Philippine parents has plummeted from 82% in 2015 to only 21% in 2018.
Pharmacovigilance is defined as the science and activities relating to the detection, assessment, understanding and prevention of adverse effects or any other drug-related problem.
The CDC says the benefits from vaccines far outweighs the risks. But those benefits only happen under the right conditions and only when they are relevant. So with that kind of thinking you can say that almost anything in the world can have benefits. But what people really want to know is why there are risks with taking vaccines? If the risks come from the negligence of a corporation, then the CDC is an accessory to a crime of negligence. When people are seeking help, you're not supposed to provide them with poisons or contaminates, and then on top of that, have the nerve to say that the vaccine is better than nothing, which is an outright lie. People are going to be extremely upset when they find out the truth, as they should be, because this truth is really freaking disturbing to say the least. It looks like the great awakening will not be as pleasurable as it should be.
Public Confidence is Low, trust has been lost and faith in government is almost nonexistent. But sadly, many people don't even know that they are being lied to, so as far as those people are concerned, as long as they keep on believing the lies, they will believe that the public trust is secure, even when it's not. People are not well informed, and they don't even know it.
We have to force pharmaceutical companies to do more testing to see which people are more vulnerable to certain vaccines, and we also have to force pharmaceutical companies to make safer vaccines.
The FDA is not always our Friend. They are easily corrupted with money and power, just like a lot of people are.
Vaccine Adverse Event Reporting System ( VAERS as of September 26, 2021) - More than 726,000 Covid vaccine-related adverse events reported to VAERS as CDC and FDA overturn advisory committee recommendations on Pfizer’s third vaccine. VAERS data released by the CDC included a total of 726,965 adverse event reports from all age groups following Covid vaccines, including 15,386 deaths and 99,410 serious complications between December 14, 2020, and September 17, 2021. There seems to be three situations: The appearance of a cancer rapidly after the injection (two weeks to a few months) and very progressive, in a person who was previously free of known carcinological pathologies. The resumption of cancer in a patient who has been in complete remission for several months or years. The rapid, even explosive, evolution of a cancer that is not yet controlled. Vaccine-induced temporary immunosuppression is also a factor that may contribute to the post-vaccination spike in coronavirus infections seen in many countries. Post-vaccination reactivation of latent viral infections, including shingles virus, EBV (Epstein-Barr) and hepatitis virus, has also been observed.
Why do Vaccine Makers have their own Court System?
Vaccine indemnification program in the US paid out thousands of claims for Billions of dollars.
Vaccine Court refers to the Office of Special Masters of the U.S. Court of Federal Claims, which administers a no-fault system for litigating vaccine injury claims. These claims against vaccine manufacturers cannot normally be filed in state or Federal Civil Courts, but instead must be heard in the Court of Claims, sitting without a jury.
National Vaccine Injury Compensation Program (VICP)
National Childhood Vaccine Injury Act (wiki)
Vaccine Compensation - Vaccine Injury - Compensation Reports.
Right to Information - Research Papers Under Reported - Risk Benefit Ratio.
How many vaccines should I get, and when? Should I get one vaccine at a time so that we can see which vaccines are the safest? Are Vaccinations are more effective when administered in the morning because of fluctuations in immune responses throughout the day?
Vaccination Schedule (wiki)
Which Type of Vaccine is Safer? Oral or Injection? For the polio vaccine, the injection is safer then the oral vaccination.
Inhalable form of messenger RNA. Patients with lung disease could find relief by breathing in messenger RNA molecules.
Should I get a DNA Screening to determine if any defects in my genes can be triggered by a vaccination?
Does a Vaccine Kill Good Bacteria? Bacteria that naturally colonize the gut may help mount a strong immune response to a seasonal flu vaccine. Findings also suggest that antibiotic treatment, which decreases the number and diversity of resident gut bacteria, may reduce the immune response to the vaccine. Understanding how gut bacteria affect vaccine responses may help scientists develop new strategies to enhance vaccine-induced immunity.
Films About Vaccines
Of course, most of these films have been censored. Just like many documentaries that have been removed that are educational. So you will have to search for the film on the internet.
How Vaccines Harm Child Brain Development - Dr Russell Blaylock MD (youtube) Adding insult to injury.
Shots in the Dark (vimeo)
In Lies We Trust (youtube)
Lethal Injection: The Story Of Vaccination (youtube)
The Greater Good is a 2012 feature documentary that looks behind the fear, hype and politics that have polarized the vaccine debate in America today.
How We'll Fight the Next Deadly Virus (video and text) TEDWomen 2015 | May 2015.
Dr. Peter McCullough gave an extensive rundown on everything Covid-19 vaccines, from safety and efficacy to the fraudulent "approval" of the Pfizer vaccine.
Vaccine Liberation Army - Drug Errors - Vaccine Truth.
Early Development and Toxins - Autoimmune Disease.
Ask for Thiomersal Mercury free Vaccines. Research.
Human Experimentation - Human Test Subjects.
Pharmaceutical Dangers - The word Natural can be Misleading.
Health Documentaries - Consumer Safety
Human Diploid Cell.
National Vaccine Information Center - Dr. Tenpenny.
Correlation does not necessarily prove causation, but you can't use that as a basis for your argument, especially when you can't prove correlation to be true or false. And you can't just focus on one ingredient and say that you done your research. Cherry Picking Data just makes look like you're hiding something.
Vaccination - Inoculation - Immunization
Vaccine is an agent that resembles a disease-causing micro-organism and is often made from weakened or killed forms of the microbe, its toxins or one of its surface proteins. The agent stimulates the body's immune system to recognize the agent as a threat, destroy it, and keep a record of it, so that the immune system can more easily recognize and destroy any of these micro-organisms that it later encounters. A vaccine works by training the immune system to recognize and combat pathogens, either viruses or bacteria. To do this, certain molecules from the pathogen must be introduced into the body to trigger an immune response. These molecules are called antigens, and they are present on all viruses and bacteria. By injecting these antigens into the body, the immune system can safely learn to recognize them as hostile invaders, produce antibodies, and remember them for the future. If the bacteria or virus reappears, the immune system will recognize the antigens immediately and attack aggressively well before the pathogen can spread and cause sickness. Vaccine Types.
Inoculation refers to artificial induction of immunity against various infectious diseases.
Immunization is the process by which an individual's immune system becomes fortified against an agent, which is known as the immunogen, by exposing an animal to an immunogen in a controlled way, so that its body can learn to protect itself. This is called active immunization.
Immunogenic relates to or denoting to substances that are able to produce an immune response.
Immunogenicity is the ability of a particular substance, such as an antigen or epitope, to provoke an immune response in the body of a human and other animal. In other words, immunogenicity is the ability to induce a humoral and/or cell-mediated immune responses.
Rapid Deployment Vaccine Collaborative is the rapid development, testing, and public sharing of vaccine recipes that are simple enough to be produced and administered by individual citizen scientists.
Artificial Induction of Immunity is the artificial induction of immunity to specific diseases by making people immune to disease by means other than waiting for them to catch the disease. The purpose is to reduce the risk of death and suffering.
Immunity in medicine is the balanced state of multicellular organisms having adequate biological defenses to fight infection, disease, or other unwanted biological invasion, while having adequate tolerance to avoid allergy, and autoimmune diseases.
Herd Immunity - Inoculation for Ignorance
Natural Immunity does not mean 100 percent immunity. You could have antibodies but still be vulnerable. Strong immunity can come from a healthy life style and also from the lack of vulnerabilities in your immune system. Vaccines may keep you safe, but not as safe as a healthy lifestyle. I stopped getting flu vaccines and I never got the flu. But there are people who did get the flu vaccine and never got the flu. So what was it, the vaccine or a healthy lifestyle?
Can you still Transmit or Spread Covid-19 after being Vaccinated? The vaccine will protect you from getting ill and then ending up hospitalized. But it's possible that you could still carry the virus and still be contagious to others. So those who get the vaccine should still wear masks and should continue practicing physical distancing. It’s also not yet known whether the Pfizer and Moderna vaccines protect people from infection entirely, or just from the symptoms. That means vaccinated people might still be able to get infected and pass the virus on, although it would likely be at a much lower rate.
Breakthrough Infection is a case of illness in which a vaccinated individual becomes sick from the same illness that the vaccine is meant to prevent. Simply, they occur when vaccines fail to provide immunity against the pathogen they are designed to target. Causes of breakthrough infections include improper administration or storage of vaccines, mutations in viruses and antibody blocking. For these reasons, vaccines are rarely 100% effective. The common flu vaccine is estimated to provide immunity to the flu in 58% of recipients. The measles vaccine fails to provide immunity to 2% of children that receive the vaccine. However, if herd immunity exists, it typically prevents individuals who are ineffectively vaccinated from contracting the disease. Accordingly, herd immunity reduces the number of breakthrough infections in a population. The varicella vaccine is 85% effective at preventing varicella infection. However, 75% of individuals that are diagnosed with breakthrough varicella exhibit milder symptoms than individuals that are not vaccinated. Variants - Strains - Mutations.
Antibody-Dependent Enhancement is a phenomenon in which the presence of specific antibodies can be beneficial to the virus and the binding of a virus to suboptimal antibodies enhances its entry into host cells, followed by its replication. Antiviral antibodies promote viral infection of target immune cells by exploiting the phagocytic FcγR or complement pathway. After interaction with the virus the antibody binds Fc receptors (FcR) expressed on certain immune cells or some of the complement proteins. FcγR binds antibody via its fragment crystallizable region (Fc). Usually the process of phagocytosis is accompanied by the virus degradation, however, if the virus is not neutralized (either due to low affinity binding or targeting to a non-neutralizing epitope), antibody binding might result in a virus escape and therefore, enhanced infection. Thus, phagocytosis can cause viral replication, with the subsequent death of immune cells. The virus “deceives” the process of phagocytosis of immune cells and uses the host's antibodies as a Trojan horse. ADE may occur due to the non-neutralizing characteristic of the antibody, which bind viral epitopes other than those involved in a host cell attachment and entry. ADE may also happen due to the presence of sub-neutralizing concentrations of antibodies (binding to viral epitopes below the threshold for neutralization). In addition ADE can be induced when the strength of antibody-antigen interaction is below the certain threshold. This phenomenon might lead to both increased virus infectivity and virulence. The viruses that can cause ADE frequently share some common features such as antigenic diversity, abilities to replicate and establish persistence in immune cells. ADE can occur during the development of a primary or secondary viral infection, as well as after vaccination with a subsequent virus challenge. It has been observed mainly with positive-strand RNA viruses. Among them are Flaviviruses such as Dengue virus, Yellow fever virus, Zika virus, Coronaviruses, including alpha- and betacoronaviruses, Orthomyxoviruses such as influenza, Retroviruses such as HIV, and Orthopneumoviruses such as RSV. The mechanism that involves phagocytosis of immune complexes via FcγRII / CD32 receptor is better understood compared to the complement receptor pathway. Cells that express this receptor are represented by monocytes, macrophages, some categories of dendritic cells and B-cells. ADE is mainly mediated by IgG antibodies, however, IgM along with complement, and IgA antibodies have also been shown to be trigger ADE. ADE may cause enhanced respiratory disease and acute lung injury after respiratory virus infection (ERD) with symptoms of monocytic infiltration and an excess of eosinophils in respiratory tract. ADE along with type 2 T helper cell-dependent mechanisms may contribute to a development of the vaccine associated disease enhancement (VADE), which is not limited to respiratory disease. Some vaccine candidates that targeted coronaviruses, RSV virus and Dengue virus elicited VADE, and were terminated from further development or became approved for use only for patients who have had those viruses before. ADE is sometimes less precisely called immune enhancement or disease enhancement.
COVID-19 Vaccine Information - COVID-19 Vaccine Information - COVID-19 Vaccine Providers
Will a COVID-19 vaccine alter my DNA? No. The mRNA from a COVID-19 vaccine never enters the nucleus of the cell, which is where our DNA is kept. COVID-19 mRNA vaccines do not change or interact with your DNA in any way. Messenger RNA vaccines—also called mRNA vaccines—are the first COVID-19 vaccines authorized for use in the United States. mRNA vaccines teach our cells how to make a protein that triggers an immune response. The mRNA from a COVID-19 vaccine never enters the nucleus of the cell, which is where our DNA is kept. This means the mRNA cannot affect or interact with our DNA in any way. Instead, COVID-19 mRNA vaccines work with the body’s natural defenses to safely develop immunity to disease. At the end of the process, our bodies have learned how to protect against future infection. That immune response and making antibodies is what protects us from getting infected if the real virus enters our bodies. Cell Death.
Are COVID-19 tests compiling people’s DNA? Only if someone wanted to. The coronavirus has RNA. If you get infected with the coronavirus, the coronavirus injects its RNA into your cells and forces them to make copies of the virus. The new copies burst out of the cell spread the virus to other cells in your body to make more copies. With the covid-19 test, the human DNA in the saliva is not analyzed and the sample is not kept longer than necessary for testing for the coronavirus.
Antigen is a molecule capable of inducing an immune response on the part of the host organism, though sometimes antigens can be part of the host itself. In other words, an antigen is any substance that causes an immune system to produce antibodies against it. Each antibody is specifically produced by the immune system to match an antigen after cells in the immune system come into contact with it; this allows a precise identification of the antigen and the initiation of a tailored response. The antibody is said to "match" the antigen in the sense that it can bind to it thanks to adaptations performed to a region of the antibody; because of this, many different antibodies can be produced, with specificity to bind many different antigens while sharing the same basic structure. In most cases, an antibody can only bind one specific antigen; in some instances, however, antibodies may bind more than one antigen.
Vaccinations Info - Vaccines.gov - Number Needed to Treat
Inoculation is not new, it's been around for hundreds of years. What's new is how we are administering our medicine today.
What other alternatives do we have that would boost our immune system?
Immune T Cells May Offer Lasting Protection Against COVID-19 - Antigen Recognition by T Cells.
Disease Outbreak Map and Monitoring.
Booster Dose is an extra administration of a vaccine after an earlier or prime dose. After initial immunization, a booster injection or booster dose is a re-exposure to the immunizing antigen. It is intended to increase immunity against that antigen back to protective levels, after memory against that antigen has declined through time. For example, tetanus shot boosters are often recommended every 10 years, before which memory cells specific against tetanus have lost their function or undergone apoptosis. The need for a booster dose following a primary vaccination is evaluated in several ways. One way is to measure the level of antibodies specific against a disease, a few years after the primary dose is given. Anamnestic response, the rapid production of antibodies after a stimulus of an antigen, is a typical way to measure the need for a booster dose of a certain vaccine. If the anamnestic response is high after receiving a primary vaccine many years ago, there is most likely little to no need for a booster dose. People can also measure the active B and T cell activity against that antigen after a certain amount of time that the primary vaccine was administered, or determine the prevalence of the disease in vaccinated populations. If a patient receives a booster dose but already has a high level of antibody, then a reaction called an Arthus reaction could develop, a localized form of Type III hypersensitivity induced by high levels of IgG antibodies causing inflammation. The inflammation is often self-resolved over the course of a few days, but could be avoided altogether by increasing the length of time between the primary vaccine and the booster dose. It is not yet fully clear why some vaccines such as hepatitis A and B are effective for life, and some such as tetanus need boosters. The prevailing theory is that if the immune system responds to a primary vaccine rapidly, the body does not have time to sufficiently develop immunological memory against the disease, and memory cells will not persist in high numbers for the lifetime of the human. After a primary response of the immune system against a vaccination, memory T helper cells and B cells persist at a fairly constant level in germinal centers, undergoing cell division at a slow to nonexistent rate. While these cells are long-lived, they do not typically undergo mitosis, and eventually the rate of loss of these cells will be greater than the rate of gain. In these cases, a booster dose is required to "boost" the memory B and T cell count back up again.
No Evidence Yet That Recovered COVID-19 Patients Are Immune, WHO Says. Immunity passports in the context of COVID-19. The development of immunity to a pathogen through natural infection is a multi-step process that typically takes place over 1-2 weeks. The body responds to a viral infection immediately with a non-specific innate response in which macrophages, neutrophils, and dendritic cells slow the progress of virus and may even prevent it from causing symptoms. This non-specific response is followed by an adaptive response where the body makes antibodies that specifically bind to the virus. These antibodies are proteins called immunoglobulins. The body also makes T-cells that recognize and eliminate other cells infected with the virus. This is called cellular immunity. This combined adaptive response may clear the virus from the body, and if the response is strong enough, may prevent progression to severe illness or re-infection by the same virus. This process is often measured by the presence of antibodies in blood. Laboratory tests that detect antibodies to SARS-CoV-2 in people, including rapid immunodiagnostic tests, need further validation to determine their accuracy and reliability. Inaccurate immunodiagnostic tests may falsely categorize people in two ways. The first is that they may falsely label people who have been infected as negative, and the second is that people who have not been infected are falsely labeled as positive. Both errors have serious consequences and will affect control efforts. These tests also need to accurately distinguish between past infections from SARS-CoV-2 and those caused by the known set of six human coronaviruses. Four of these viruses cause the common cold and circulate widely. The remaining two are the viruses that cause Middle East Respiratory Syndrome and Severe Acute Respiratory Syndrome. People infected by any one of these viruses may produce antibodies that cross-react with antibodies produced in response to infection with SARS-CoV-2. People who assume that they are immune to a second infection because they have received a positive test result may ignore public health advice. A person may have very low levels of neutralizing antibodies in their blood, so knowing how long a person may be immune is not clear.
How many children get Autism who have never received a vaccine in their entire life? So what if my child did not get autism from vaccines, but what about a lower IQ, or other side effects?
Non-Communicable Disease is a medical condition or disease that is not caused by infectious agents (non-infectious or non-transmissible). Causes of Death - Poverty.
Vaccine-Preventable Diseases (wiki)
Vaccine Preventable Diseases Monitoring System.
Health Map.
Russell Blaylock MD.
Vaccines Hurt Babies (youtube channel)
Cytokine - Colds and Flu - Immune System
Microglia are a type of glial cell located throughout the brain and spinal cord. Microglia account for 10–15% of all cells found within the brain. As the resident macrophage cells, they act as the first and main form of active immune defense in the central nervous system (CNS)
Mitochondrial Antiviral-Signaling Protein (wiki).
Viruses Carry Antiviral Cargo
cGAMP (wiki).
Immunize - FDA Biologics Blood Vaccines.
When WHO says routine life-saving immunizations could avert 1.5 million deaths each year from preventable diseases, what they're not saying is that the 1.5 million deaths each year from preventable diseases is mostly a result of poor people who have no access to a good education, or clean water, or healthy food, or healthy homes. When you lie and mislead people, that means you are trying to hide something, and that's when people stop trusting you. So what will stop the murders of millions of people every year? Maybe a shot of the truth. Path.
The number of cases of Polio worldwide in 2018 as of Dec. 25 was 29, compared to 22 in 2017. There were an estimated 350,000 cases around the world in 1988.
Vaccine-Derived Poliovirus is a strain related to the weakened live poliovirus contained in oral polio vaccine. If allowed to circulate in under- or unimmunized populations for long enough, or replicate in an immunodeficient individual, the weakened virus can revert to a form that causes illness and paralysis.
A mysterious polio-like disease, called Acute Flaccid Myelitis that can paralyze patients, mostly children, appeared in the U.S. in 2014 with 120 confirmed cases from August to December. There were 22 confirmed cases in 2015, 149 confirmed cases in 2016, 35 confirmed cases is 2017 and 182 cases as of Dec. 21, 2018.
Acute is having or experiencing a rapid onset and short but severe course. Extremely sharp or intense.
Vaccine Equity: All governments to ensure that COVID-19 vaccines are distributed free and equally at the point of care and without risk of financial hardship and without unfair illogical discrimination, starting with health workers and those people at greatest risk of COVID-19, to prioritize affected communities and the voices of essential workers in decision-making and ensure gender equality is central to all actions. Unequal distribution of vaccines still remains the biggest threat to ending the acute stage of this pandemic and driving a global recovery. We must continue to push for vaccines to be both equitably distributed and equitably produced throughout 2021 and beyond. Vaccine distribution remains nonexistent in many of the poorest countries, and experts anticipate that 80% of the population in low-resource settings will not receive a vaccine this year. Although investment in discovery is critical, the long-term neglect of public health and global delivery strategies has left us poorly equipped to end this pandemic. The world is on the brink of a catastrophic moral failure – and the price of this failure will be paid with lives and livelihoods in the world’s poorest countries. #VaccinEquity, which aims to overcome the pandemic and the inequalities that lie at the root of so many global health challenges, as well as drive a global recovery. Global Citizen said its campaign had raised $302 million and secured over 26 million COVID-19 vaccine doses. The money will go toward vaccine delivery, testing and personal protective equipment, as part of the COVAX initiative. The effort, led by the World Health Organization, Gavi and other partners, aims to evenly distribute vaccines and supplies around the world.
Vaccine Types
Inactivated Vaccines use the killed version of the germ that causes a disease. Inactivated vaccines usually don't provide immunity (protection) that's as strong as live vaccines. So you may need several doses over time (booster shots) in order to get ongoing immunity against diseases. Inactivated Vaccine is a vaccine consisting of virus particles, bacteria, or other pathogens that have been grown in culture and then killed to destroy disease producing capacity. In contrast, live vaccines use pathogens that are still alive (but are almost always attenuated, that is, weakened). Pathogens for inactivated vaccines are grown under controlled conditions and are killed as a means to reduce infectivity and thus prevent infection from the vaccine. The virus is killed using a method such as heat or formaldehyde. Inactivated vaccines are further classified depending on the method used to inactivate the virus. Whole virus vaccines use the entire virus particle, fully destroyed using heat, chemicals, or radiation. Split virus vaccines are produced by using a detergent to disrupt the virus. Subunit vaccines are produced by purifying out the antigens that best stimulate the immune system to mount a response to the virus, while removing other components necessary for the virus to replicate or survive or that can cause adverse reactions. Because inactivated viruses tend to produce a weaker response by the immune system than live viruses, immunologic adjuvants and multiple "booster" injections may be required to provide an effective immune response against the pathogen. Attenuated vaccines are often preferable for generally healthy people because a single dose is often safe and very effective. However, some people cannot take attenuated vaccines because the pathogen poses too much risk for them (for example, elderly people or people with immunodeficiency). For those patients, an inactivated vaccine can provide protection.
Attenuated Vaccines or Live Vaccines use a weakened or attenuated form of the germ that causes a disease. Because these vaccines are so similar to the natural infection that they help prevent, they create a strong and long-lasting immune response. Attenuated Vaccine is a vaccine created by reducing the virulence of a pathogen, but still keeping it viable (or "live"). Attenuation takes an infectious agent and alters it so that it becomes harmless or less virulent. These vaccines contrast to those produced by "killing" the virus (inactivated vaccine). Attenuated vaccines stimulate a strong and effective immune response that is long-lasting. In comparison to inactivated vaccines, attenuated vaccines produce a stronger and more durable immune response with a quick immunity onset. Attenuated vaccines function by encouraging the body to create antibodies and memory immune cells in response to the specific pathogen which the vaccine protects against. Common examples of live attenuated vaccines are measles, mumps, rubella, yellow fever, and some influenza vaccines. Attenuated Vaccine is a vaccine created by reducing the virulence of a pathogen, but still keeping it viable (or "live"). Attenuation takes an infectious agent and alters it so that it becomes harmless or less virulent. These vaccines contrast to those produced by "killing" the virus (inactivated vaccine). Live Vaccines (wiki) - Living Drug - How Live Vaccines enhance the body's immune response. New findings point the way to more efficient vaccines. Live Attenuated Influenza Vaccine is a type of influenza vaccine in the form of a nasal spray that used to be recommended to prevent influenza. In June 2016 the CDC stopped recommending the use of LAIV as its effectiveness has appeared to have decreased between 2013 and 2016. - Live Attenuated Influenza Vaccine FluMist (wiki)
Messenger RNA vaccines or mRNA vaccines make proteins in order to trigger an immune response. They do not contain a live virus, no risk of causing disease in the person getting vaccinated. less effective. RNA Vaccine is a type of vaccine that uses a copy of a natural chemical called messenger RNA (mRNA) to produce an immune response. The vaccine transfects molecules of synthetic RNA into immunity cells. Once inside the immune cells, the vaccine's RNA functions as mRNA, causing the cells to build the foreign protein that would normally be produced by a pathogen (such as a virus) or by a cancer cell. These protein molecules stimulate an adaptive immune response which teaches the body how to identify and destroy the corresponding pathogen or cancer cells. The delivery of mRNA is achieved by a co-formulation of the molecule into lipid nanoparticles which protect the RNA strands and helps their absorption into the cells. Genetic Vaccine or DNA and RNA-based vaccines. DNA vaccines were introduced less than a decade ago but have already been applied to a wide range of infectious and malignant diseases. Katalin Karikó.
Subunit Vaccine is a vaccine that presents one or more antigens to the immune system without introducing pathogen particles, whole or otherwise. The antigens involved can be any molecule, and do not need to be a protein subunit; the word "subunit" simply means the antigen is a fragment of the pathogen. Just like inactivated vaccines, the vaccine is completely "dead", and is therefore less risky. Subunit, recombinant, polysaccharide, and conjugate vaccines use specific pieces of the germ—like its protein, sugar, or capsid (a casing around the germ). Because these vaccines use only specific pieces of the germ, they give a very strong immune response that’s targeted to key parts of the germ.
Viral Vector Vaccines use a modified version of a different virus as a vector to deliver protection. Viral Vector are tools commonly used by molecular biologists to deliver genetic material into cells. This process can be performed inside a living organism (in vivo) or in cell culture (in vitro). Viruses have evolved specialized molecular mechanisms to efficiently transport their genomes inside the cells they infect. Delivery of genes or other genetic material by a vector is termed transduction and the infected cells are described as transduced. Molecular biologists first harnessed this machinery in the 1970s. Paul Berg used a modified SV40 virus containing DNA from the bacteriophage λ to infect monkey kidney cells maintained in culture. In addition to their use in molecular biology research, viral vectors are used for gene therapy and the development of vaccines.
Toxoid Vaccines are made from a toxin or poison that has been made harmless but that elicits an immune response against the toxin. Toxoid use a toxin or harmful product made by the germ that causes a disease. They create immunity to the parts of the germ that cause a disease instead of the germ itself. That means the immune response is targeted to the toxin instead of the whole germ. Toxoid is an inactivated toxin (usually an exotoxin) whose toxicity has been suppressed either by chemical (formalin) or heat treatment, while other properties, typically immunogenicity, are maintained. Toxins are secreted by bacteria, whereas toxoids are altered form of toxins; toxoids are not secreted by bacteria. Thus, when used during vaccination, an immune response is mounted and immunological memory is formed against the molecular markers of the toxoid without resulting in toxin-induced illness. Such a preparation is also known as an anatoxin. There are toxoids for prevention of diphtheria, tetanus and botulism. Toxoids are used as vaccines because they induce an immune response to the original toxin or increase the response to another antigen since the toxoid markers and toxin markers are preserved. For example, the tetanus toxoid is derived from the tetanospasmin produced by Clostridium tetani. The latter causes tetanus and is vaccinated against by the DTaP vaccine. While patients may sometimes complain of side effects after a vaccine, these are associated with the process of mounting an immune response and clearing the toxoid, not the direct effects of the toxoid. The toxoid does not have virulence as the toxin did before inactivation. Toxoids are also useful in the production of human antitoxins. Multiple doses of tetanus toxoid are used by many plasma centers in the United States for the development of highly immune persons for the production of human anti-tetanus immune globulin (tetanus immune globulin (TIG), HyperTet (c)), which has replaced horse serum-type tetanus antitoxin in most of the developed world. Toxoids are also used in the production of conjugate vaccines. The highly antigenic toxoids help draw attention to weaker antigens such as polysaccharides found in the bacterial capsule.
Microneedle Patch. Your skin is a pretty good place to deliver a vaccine. It's full of immune cells. The outermost part of the skin called the stratum corneum consists of a layer of cells thinner than a sheet of paper. Tiny needles are now frequently made out of water-soluble materials, so once they get into your skin, they dissolve, releasing whatever you've packed inside of them. Thr patch could deliver multiple vaccine doses spaced days or weeks apart with a single application. The trick is to imbed the vaccine in needles that dissolve at different rates. The patient wouldn't need to remember the schedule of the vaccination. Vaccine Patch.
Vaccine printer could help vaccines reach more people. The printer generates vaccine-filled microneedle patches that can be stored long-term at room temperature and applied to the skin.
Transdermal Patch is a medicated adhesive patch that is placed on the skin to deliver a specific dose of medication through the skin and into the bloodstream. Often, this promotes healing to an injured area of the body. An advantage of a transdermal drug delivery route over other types of medication delivery such as oral, topical, intravenous, intramuscular, etc. is that the patch provides a controlled release of the medication into the patient, usually through either a porous membrane covering a reservoir of medication or through body heat melting thin layers of medication embedded in the adhesive. The main disadvantage to transdermal delivery systems stems from the fact that the skin is a very effective barrier; as a result, only medications whose molecules are small enough to penetrate the skin can be delivered by this method. A wide variety of pharmaceuticals are now available in transdermal patch form. The first commercially available prescription patch was approved by the U.S. Food and Drug Administration in December 1979. These patches administered scopolamine for motion sickness.
Needle free injection technology - Laser powered liquid jets could inject drugs into skin without needles.
Dry Powder Nasal Vaccines as an alternative to needle-based delivery. Dry powder vaccines offer the advantages of chemical and physical stability in comparison to liquid formulations. An intranasal vaccine can elicit both a local and systemic immune response. Mucoadhesive compounds can extend the residence time for powder formulations on the nasal mucosa, potentially increasing the immune response. Manufacture and characterization of a formulation containing particles of a dry powder vaccine are discussed.
New nasal spray treats Delta variant infection in mice, indicating broad spectrum results. The specially designed compound, named N-0385, blocks a particular human enzyme's activity, used by the virus to infect a host cell.
Center for Drug Design, Development and Delivery.
HYDRA Device converts electricity passing through a piezoelectric chip into mechanical vibration, or sound waves, which in turn break liquid into a spray, so that vaccines can be inhaled through a nebulizer device.
Vaccines made from Plants. Plant-Based Vaccines or Plant-Derived Vaccines. Quebec-based Medicago is transforming the use of plant-based technologies to rapidly develop and produce novel vaccines and therapeutic proteins. Plants are among the world’s most prolific protein producers; in contrast to protein production via cell cultures or eggs, which is relatively complicated and time-consuming, plants express proteins of varying complexity and glycosylation patterns with high efficiency. So Medicago, a clinical-stage biopharmaceutical company located in Quebec, Canada, is harnessing a plant-based transient expression process to produce pharmaceutical-grade proteins in a matter of weeks. Compared to alternative production systems, our proprietary plant-based manufacturing platform has many advantages, including faster lead time, scalability and versatility. Medicago’s production process starts with the synthesis of genetic sequence coding for a particular protein. This sequence is then introduced into Agrobacterium tumefaciens , a bacterial vector that can transfer genetic material to plants only. The plant in question, Nicotiana benthamiana , is a close relative of tobacco indigenous to Australia, has a fast growth rate, is a non-food crop, and is easy to work with. It is dipped into a bath of the modified Agrobacterium , which, with the assistance of a vacuum, is soaked up by the plant. The Agrobacterium transfers the genetic material into the leaf tissue, which then produces and accumulates the recombinant product for 6–8 days. At this point, the leaves are harvested and the proteins are extracted and purified under pharma-grade conditions. COVID vaccine grown in plants, No ultracold freezers required. The vaccine look-alike is something called a "virus-like particle" produced in plant cells that were given genetic instructions to make the coronavirus spike protein. Vaccines work by showing the immune system something that looks like a virus, but isn't. Doing that allows the immune system to prepare itself in case the real virus should show up. Plant-based vaccines for animals and humans: recent advances in technology and clinical trials. Plant-based vaccines: novel and low-cost possible route for Mediterranean innovative vaccination strategies
Immune system-stimulating nanoparticle could lead to more powerful vaccines. Researchers designed a new nanoparticle adjuvant that may be more potent than others now in use. Studies in mice showed it significantly improved antibody production following vaccination against HIV, diphtheria and influenza. Although the idea of using adjuvants to boost vaccine effectiveness has been around for decades, there are only a handful of FDA-approved vaccine adjuvants. One is aluminum hydroxide, an aluminum salt that induces inflammation, and another is an oil and water emulsion that is used in flu vaccines. A few years ago, the FDA approved an adjuvant based on saponin, a compound derived from the bark of the Chilean soapbark tree. Saponin formulated in liposomes is now used as an adjuvant in the shingles vaccine, and saponins are also being used in a cage-like nanoparticle called an immunostimulatory complex (ISCOM) in a Covid-19 vaccine that is currently in clinical trials. Researchers have shown that saponins promote inflammatory immune responses and stimulate antibody production, but how they do that is unclear. In the new study, the MIT and La Jolla team wanted to figure out how the adjuvant exerts its effects, and to see if they could make it more potent. They designed a new type of adjuvant that is similar to the ISCOM adjuvant but also incorporates a molecule called MPLA, which is a toll-like receptor agonist. When these molecules bind to toll-like receptors on immune cells, they promote inflammation. The researchers call their new adjuvant SMNP (saponin/MPLA nanoparticles).
The medicine of the future could be artificial life forms. Imagine a life form that doesn't resemble any of the organisms found on the tree of life. One that has its own unique control system, and that a doctor would want to send into your body. Hybrid peptide-DNA nanostructures is the parent of a special artificial hybrid molecule that could lead to the creation of artificial life forms. Such artificial life forms can act as vaccines against viral infection and can be used as nanorobots or nano-machines loaded with medication or diagnostic elements and sent into a patient's body. Self-Assembly of Hybrid Peptide-DNA Nanostructures using Homotrimeric Coiled-Coil/Nucleic Acid Building Blocks. Peptides and DNA are two of the most commonly used self-assembling biological molecules for the construction of nanomaterials.
Vaccines for Covid-19 by Manufacturer
Pfizer - BioNTech COVID-19 Vaccine. Requires 2 shots, 21 days apart FDA has authorized the emergency use of the Pfizer-BioNTech COVID-19 Vaccine in individuals 16 years of age and older. The Pfizer BioNTech COVID-19 vaccine is a messenger RNA or mRNA vaccine that has both synthetic, or chemically produced, and enzymatically produced components from naturally occurring substances such as proteins. The vaccine does not contain any live virus. Its inactive ingredients include potassium chloride, monobasic potassium, phosphate, sodium chloride, dibasic sodium phosphate dihydrate, and sucrose, as well as small amounts of other ingredients. The Pfizer-BioNTech COVID-19 Vaccine includes the following ingredients: mRNA, lipids ((4-hydroxybutyl)azanediyl)bis(hexane-6,1-diyl)bis(2-hexyldecanoate), 2 [(polyethylene glycol)-2000]-N,N-ditetradecylacetamide, 1,2-Distearoyl-sn-glycero-3-phosphocholine, and cholesterol), potassium chloride, monobasic potassium phosphate, sodium chloride, dibasic sodium phosphate dihydrate, and sucrose. The approval status of the Pfizer‑BioNTech COVID‑19 Vaccine varies worldwide. In countries where the vaccine has not been approved by the relevant regulatory authority, it is an investigational drug, and its safety and efficacy have not been established.
Moderna COVID-19 Vaccine. Name: mRNA-1273. 2 shots, one month (28 days) apart. Contains the following ingredients: messenger ribonucleic acid (mRNA), lipids ( SM-102, polyethylene glyc ol [ P EG] 2000 dimyristoyl glycerol [DMG], cholesterol, and 1,2-distearoyl-sn-glycero-3-phosphocholine [DSP C]), tromethamine, tromethamine hydrochloride, acetic acid, sodium acetate, and sucrose. Clinical trials for the Moderna vaccine included people from the following racial and ethnic categories: 79.4% White, 20% Hispanic/Latino, 9.7% African American, 4.7% Asian, <3% other races/ethnicities. Age and sex breakdown: 52.6% male, 47.4% female, 25.3% 65 years and older. Most people who participated in the trials (82%) were considered to have an occupational risk of exposure, with 25.4% of them being healthcare workers. Among people who participated in the clinical trials, 22.3% had at least one high-risk condition, which included lung disease, heart disease, obesity, diabetes, liver disease, or HIV infection. Four percent (4%) of participants had two or more high-risk conditions.
Johnson & Johnson’s Janssen COVID-19 Vaccine. Name: JNJ-78436735. Type of vaccine: Viral vector. 1 shot. Includes the following ingredients: recombinant, replication-incompetentadenovirus type 26expressing the SARS-CoV-2 spike protein, citric acid monohydrate, trisodium citrate dihydrate, ethanol, 2-hydroxypropyl-β-cyclodextrin (HBCD), polysorbate-80, sodium chloride. V-safe is a new voluntary smartphone-based tool that uses text messaging and web surveys to check in with people who have been vaccinated to identify potential side effects after COVID-19 vaccination. V-safeasks questions that help CDC monitor the safety of COVID-19 vaccines. V-safealso provides live telephone follow-up by CDC if participants report a significant health impact following COVID-19 vaccination. Side effects were more common in people 18–59 years old compared to people 60 years and older. Clinical trials for the J&J/Janssen vaccine included people from the following racial and ethnic categories: 58.7% White, 45.3% Hispanic or Latino, 19.4% Black or African American, 9.5% American Indian or Alaska Native, 5.6% Multiple races, 3.3% Asian, 0.2% Native Hawaiian or other Pacific Islander. Sex breakdown: 54.9% Male, 45.0% Female, <0.1% Undifferentiated or unknown sex. Age breakdown: 66.5% 18–59 years, 33.5% 60 years and older, 19.6% 65 years and older, 3.5% 75 years and older. Estimates of Vaccine Efficacy from Phase 3 Clinical Trials (image).
AstraZeneca - Oxford-AstraZeneca ChAdOx1 nCoV-19 (AZD1222) vaccine is given as a two-dose course, which is given as an injection into the upper arm. The second dose is given 4-12 weeks after the first dose. AZD1222 US Phase III trial met primary efficacy endpoint in preventing COVID-19 at interim analysis. 79% vaccine efficacy at preventing symptomatic COVID-19. 100% efficacy against severe or critical disease and hospitalization. Comparable efficacy result across ethnicity and age, with 80% efficacy in participants aged 65 years and over. For full information on ingredients, ask for the Patient Information Leaflet for the vaccine you are offered. Favourable reactogenicity and overall safety profile. The active ingredient of the Oxford-AstraZeneca ChAdOx1 nCoV-19 vaccine is made from a modified adenovirus which causes the common cold in chimpanzees. This virus has been modified so that it cannot cause an infection. It is used to deliver the genetic code for the coronavirus spike protein. The vaccine also contains inactive ingredients such as polysorbate 80, an emulsifier, and a very small amount of alcohol (0.002mg per dose). The vaccine also contains traces of magnesium (3 to 20 parts per million). Sucrose (sugar). Acidity regulators such as Histidine, and sodium and potassium salts.
 Nucleic acid and viral vectored vaccines
explained. Newer vaccines such as mRNA vaccines and viral vectored
vaccines, including the Oxford ChAdOx1 nCoV-19 vaccine differ from many
traditional vaccines in the way they activate the immune system. Most
traditional vaccines inject the antigen (part of the disease that
stimulates an immune response) directly into the body. Firstly, we will
look at how cells normally manufacture proteins. Our DNA (DeoxyRibonucleic
Acid) is safely packaged inside the nucleus of a cell and cannot leave.
Within this DNA are gene sequences, and each gene encodes the blueprints
for making one of the proteins the body needs. To make a protein the first
step is to transcribe DNA into mRNA (messenger Ribonucleic Acid) using a
special enzyme (or “tool”) called RNA polymerase. This step is a one-way
process as cells are unable to transcribe RNA back into DNA. Unlike
DNA, mRNA is free to leave the nucleus as it has a pass that allows it to
exit. However, this pass is one way and once it leaves, the mRNA cannot
return. Once it has left the nucleus the mRNA links up with the special
cellular machinery in the cytoplasm. This machinery uses the information
coded in the mRNA to make new proteins. As with the process of going from
DNA to mRNA this process is also one-way, and it’s not possible to go
backwards from protein to mRNA. These proteins may be used inside the cell
or transported out of the cell for use elsewhere in the body. The COVID-19
mRNA vaccines take advantage of this internal process to make copies of
the spike protein, which usually appears on the surface of the
coronavirus. There are two types of vaccine which use this process: mRNA
vaccines. In this type of vaccine, mRNA is delivered to the cell inside a
lipid membrane. Once the mRNA is inside the cell, the same machinery that
is used to make our own proteins can make the spike protein. This mRNA has
no way of getting into the nucleus where our DNA is. Even if it could,
mRNA cannot fuse with DNA and as with our own mRNA, has no way of getting
translated back to DNA. As such, there is no way for human DNA to be
altered by an mRNA vaccine. This mRNA lasts a few days before the cell
removes it, but in that time we have produced a lot of spike protein to
stimulate the immune response. Viral vectored vaccines. Viral vectored
vaccines work in a different way. The genetic information inside a viral
vectored vaccine like ChAdOx1 is DNA rather than RNA. This DNA is a short
linear piece of double stranded DNA which contains the viral genes along
with the gene for the spike protein. The viral vector first infects the
cell and then delivers this DNA to the cell nucleus. The cell can then
transcribes the viral genes (DNA) into mRNA using the same RNA polymerase
it uses for our own genes. After transcription, the mRNA gets tagged so it
can leave the nucleus and be made into spike protein by the cell
machinery. In the Oxford vaccine, the viral gene that is required to
replicate viral DNA has been removed. As viruses use a different process
to human cells to replicate their DNA, the cell itself cannot replicate
viral DNA either. This means the viral vector cannot replicate (make more
viruses) or cause disease. Both the original viral DNA and the spike
protein mRNA only last a few days before the cell removes them. Such
design features alongside a cell’s natural DNA protection measures,
prevents any possibility of viral DNA integrating with human DNA.
AZD1222 is produced in genetically modified human embryonic kidney
(HEK) 293 cellsand by recombinant DNA technology. List of excipients: L-Histidine,
L-Histidine hydrochloride monohydrate, magnesium chloride hexahydrate,
polysorbate 80, ethanol, sucrose, sodium chloride, disodium edetate
dihydrate, and water for injections.
Nucleic acid and viral vectored vaccines
explained. Newer vaccines such as mRNA vaccines and viral vectored
vaccines, including the Oxford ChAdOx1 nCoV-19 vaccine differ from many
traditional vaccines in the way they activate the immune system. Most
traditional vaccines inject the antigen (part of the disease that
stimulates an immune response) directly into the body. Firstly, we will
look at how cells normally manufacture proteins. Our DNA (DeoxyRibonucleic
Acid) is safely packaged inside the nucleus of a cell and cannot leave.
Within this DNA are gene sequences, and each gene encodes the blueprints
for making one of the proteins the body needs. To make a protein the first
step is to transcribe DNA into mRNA (messenger Ribonucleic Acid) using a
special enzyme (or “tool”) called RNA polymerase. This step is a one-way
process as cells are unable to transcribe RNA back into DNA. Unlike
DNA, mRNA is free to leave the nucleus as it has a pass that allows it to
exit. However, this pass is one way and once it leaves, the mRNA cannot
return. Once it has left the nucleus the mRNA links up with the special
cellular machinery in the cytoplasm. This machinery uses the information
coded in the mRNA to make new proteins. As with the process of going from
DNA to mRNA this process is also one-way, and it’s not possible to go
backwards from protein to mRNA. These proteins may be used inside the cell
or transported out of the cell for use elsewhere in the body. The COVID-19
mRNA vaccines take advantage of this internal process to make copies of
the spike protein, which usually appears on the surface of the
coronavirus. There are two types of vaccine which use this process: mRNA
vaccines. In this type of vaccine, mRNA is delivered to the cell inside a
lipid membrane. Once the mRNA is inside the cell, the same machinery that
is used to make our own proteins can make the spike protein. This mRNA has
no way of getting into the nucleus where our DNA is. Even if it could,
mRNA cannot fuse with DNA and as with our own mRNA, has no way of getting
translated back to DNA. As such, there is no way for human DNA to be
altered by an mRNA vaccine. This mRNA lasts a few days before the cell
removes it, but in that time we have produced a lot of spike protein to
stimulate the immune response. Viral vectored vaccines. Viral vectored
vaccines work in a different way. The genetic information inside a viral
vectored vaccine like ChAdOx1 is DNA rather than RNA. This DNA is a short
linear piece of double stranded DNA which contains the viral genes along
with the gene for the spike protein. The viral vector first infects the
cell and then delivers this DNA to the cell nucleus. The cell can then
transcribes the viral genes (DNA) into mRNA using the same RNA polymerase
it uses for our own genes. After transcription, the mRNA gets tagged so it
can leave the nucleus and be made into spike protein by the cell
machinery. In the Oxford vaccine, the viral gene that is required to
replicate viral DNA has been removed. As viruses use a different process
to human cells to replicate their DNA, the cell itself cannot replicate
viral DNA either. This means the viral vector cannot replicate (make more
viruses) or cause disease. Both the original viral DNA and the spike
protein mRNA only last a few days before the cell removes them. Such
design features alongside a cell’s natural DNA protection measures,
prevents any possibility of viral DNA integrating with human DNA.
AZD1222 is produced in genetically modified human embryonic kidney
(HEK) 293 cellsand by recombinant DNA technology. List of excipients: L-Histidine,
L-Histidine hydrochloride monohydrate, magnesium chloride hexahydrate,
polysorbate 80, ethanol, sucrose, sodium chloride, disodium edetate
dihydrate, and water for injections.Injections
 Injection in medicine is the act of putting a liquid, especially a
drug, into a person's body using a needle (usually a
hypodermic needle) and a
syringe.
Injection is a technique for delivering drugs by
parenteral administration, that is, administration via a route other
than through the digestive tract.
Parenteral injection includes subcutaneous, intramuscular,
intravenous,
intraperitoneal, intracardiac, intraarticular and intracavernous
injection. Injection is generally administered as a
bolus, but can possibly be used for continuous drug administration as
well. Even when administered as a bolus, the medication may be
long-acting, and can then be called
depot injection. Administration by an indwelling catheter is generally
preferred instead of injection in case of more long-term or recurrent drug
administration. Injections are among the most common health care
procedures, with at least 16 billion administered
in developing and transitional countries each year. 95% of
injections are administered in curative care, 3% are for immunization, and
the rest for other purposes, such as
blood transfusions. In
some instances the term injection is used synonymously with inoculation
even by different workers in the same hospital. This should not cause
confusion; the focus is on what is being injected/inoculated, not the
terminology of the procedure. Since the process inherently involves a
small puncture wound to the body (with varying
degrees of pain depending
on injection type and location, medication type, needle gauge and the
skill of the individual administering the injection), fear of needles is a
common phobia.
Injection in medicine is the act of putting a liquid, especially a
drug, into a person's body using a needle (usually a
hypodermic needle) and a
syringe.
Injection is a technique for delivering drugs by
parenteral administration, that is, administration via a route other
than through the digestive tract.
Parenteral injection includes subcutaneous, intramuscular,
intravenous,
intraperitoneal, intracardiac, intraarticular and intracavernous
injection. Injection is generally administered as a
bolus, but can possibly be used for continuous drug administration as
well. Even when administered as a bolus, the medication may be
long-acting, and can then be called
depot injection. Administration by an indwelling catheter is generally
preferred instead of injection in case of more long-term or recurrent drug
administration. Injections are among the most common health care
procedures, with at least 16 billion administered
in developing and transitional countries each year. 95% of
injections are administered in curative care, 3% are for immunization, and
the rest for other purposes, such as
blood transfusions. In
some instances the term injection is used synonymously with inoculation
even by different workers in the same hospital. This should not cause
confusion; the focus is on what is being injected/inoculated, not the
terminology of the procedure. Since the process inherently involves a
small puncture wound to the body (with varying
degrees of pain depending
on injection type and location, medication type, needle gauge and the
skill of the individual administering the injection), fear of needles is a
common phobia.Disease
Disease is a particular abnormal condition, a disorder of a structure or function, that affects part or all of an organism. The study of disease is called pathology which includes the causal study of etiology, which is the study of causation, or origination. Disease is often construed as a medical condition associated with specific symptoms and signs. It may be caused by external factors such as pathogens, or it may be caused by internal dysfunctions particularly of the immune system such as an immunodeficiency, or a hypersensitivity including allergies and autoimmunity.
Non-Communicable Disease is a disease that is not transmissible directly from one person to another. NCDs include Parkinson's disease, autoimmune diseases, strokes, most heart diseases, most cancers, diabetes, chronic kidney disease, osteoarthritis, osteoporosis, Alzheimer's disease, cataracts, and others. NCDs may be chronic or acute. Most are non-infectious, although there are some non-communicable infectious diseases, such as parasitic diseases in which the parasite's life cycle does not include direct host-to-host transmission. NCDs are the leading cause of death globally. In 2012, they caused 68% of all deaths (38 million) up from 60% in 2000. About half were under age 70 and half were women. Risk factors such as a person's background, lifestyle and environment increase the likelihood of certain NCDs. Every year, at least 5 million people die because of tobacco use and about 2.8 million die from being overweight. High cholesterol accounts for roughly 2.6 million deaths and 7.5 million die because of high blood pressure. Healing.
The deadliest disease is propaganda, which is extremely infectious, especially for ignorant and gullible people.
Progressive Disease is a disease or physical ailment whose course in most cases is the worsening, growth, or spread of the disease. This may happen until death, serious debility, or organ failure occurs. Some progressive diseases can be halted and reversed by treatment. Many can be slowed by medical therapy. Some cannot be altered by current treatments.
Illness is a disease or period of sickness affecting the body or mind. Impairment of normal physiological function affecting part or all of an organism.
Body Burden - Body affects the Mind - Food Poison - Cognitive Impairment - Cancer
Sick is a feeling of nausea or a feeling that you get when you're about to vomit. Sickness is affected by an impairment of normal physical or mental function.
Nausea is a feeling of illness or discomfort in the digestive system, usually characterized by a strong urge to vomit.
Vomiting is the involuntary, forceful expulsion of the contents of one's stomach through the mouth and sometimes the nose.
Terminal Illness is an incurable disease that cannot be adequately treated and is reasonably expected to result in the death of the patient. This term is more commonly used for progressive diseases such as cancer or advanced heart disease than for trauma. Terminal illness or end-stage disease is an incurable disease that cannot be adequately treated and is reasonably expected to result in the death of the patient. This term is more commonly used for progressive diseases such as cancer or advanced heart disease than for trauma.
Chronic Condition is a human health condition or disease that is persistent or otherwise long-lasting in its effects or a disease that comes with time. The term chronic is often applied when the course of the disease lasts for more than three months. Common chronic diseases include arthritis, asthma, cancer, COPD, diabetes and some viral diseases such as hepatitis C and HIV/AIDS. An illness which is lifelong because it ends in death is a terminal illness. Chronic Disease.
Chronic Medicine is a human health condition or disease that is persistent or otherwise long-lasting in its effects or a disease that comes with time.
Rare Disease is any disease that affects a small percentage of the population. In some parts of the world, an orphan disease is a rare disease whose rarity means there is a lack of a market large enough to gain support and resources for discovering treatments for it, except by the government granting economically advantageous conditions to creating and selling such treatments. Orphan drugs are ones so created or sold. Most rare diseases are genetic and thus are present throughout the person's entire life, even if symptoms do not immediately appear. Many rare diseases appear early in life, and about 30% of children with rare diseases will die before reaching their fifth birthday. With only three diagnosed patients in 27 years, ribose-5-phosphate isomerase deficiency is considered the rarest known genetic disease. No single cut-off number has been agreed upon for which a disease is considered rare. A disease may be considered rare in one part of the world, or in a particular group of people, but still be common in another. The US organisation Global Genes has estimated that more than 300 million people worldwide are living with one of the approximately 7,000 diseases they define as "rare" in the United States.
Idiopathic Disease is any disease with an unknown cause or mechanism of apparent spontaneous origin. Rare Disease.
Pathogen is anything that can produce disease. Infectious agent such as a virus, bacterium, prion, a fungus, or even another micro-organism. Model sheds new light on pathogen cooperation.
Pathogenic is a bacterium, virus, or other microorganism causing disease.
Pathogenesis of a disease is the biological mechanism or mechanisms that leads to the diseased state.
Asymptomatic is a patient who is a carrier for a disease or infection but experiences no symptoms.
Communicable - Contagious - Transmissible - Host
Institute for Health Metrics and Evaluation is an independent population Health Research center at UW Medicine provides rigorous and comparable measurement of the world's most important health problems and evaluates the strategies used to address them. IHME makes this information freely available so that policymakers have the evidence they need to make informed decisions about how to allocate resources to best improve population health.
Infectious Diseases Emergency Preparedness Plan.
Hepatitis A, B, C, D and E viruses kill 1.34 million people a year. HIV/AIDS claims 1 million lives a year. Estimates vary for malaria (from 429,000 deaths by WHO's calculations to 719,000 deaths according to the new report). TB statistics range from 1.2 million in the study to 1.8 million from WHO).
Global Burden of Disease Study is a comprehensive regional and global research program of disease burden that assesses mortality and disability from major diseases, injuries, and risk factors. GBD is a collaboration of over 1,800 researchers from 127 countries. The Lancet general medical journal.
Mosquito-Borne Disease are diseases caused by bacterial, viruses or parasites transmitted by mosquitoes. They can transmit disease without being affected themselves. Diseases transmitted by mosquitoes include: malaria, dengue, West Nile virus, chikungunya, yellow fever, filariasis, Japanese encephalitis, Saint Louis encephalitis, Western equine encephalitis, Eastern equine encephalitis, Venezuelan equine encephalitis, La Crosse encephalitis and Zika fever. Nearly 700 million people get a mosquito borne illness each year resulting in greater than one million deaths.
A secret weapon against Zika and other mosquito-borne diseases: Nina Fedoroff (video and interactive text). A little British company called Oxitec genetically modified that mosquito so that when it mates with a wild female, its eggs don't develop to adulthood. Zika Virus (wiki)
Why Malaria Parasites Genus Plasmodium are faster than human immune cells. Elementary cytoskeleton protein is different in parasites and represents a starting point for a possible new therapy against malaria infections.
Newly described Human Antibody prevents Malaria in mice.
Researchers map malaria parasites proliferating in human blood cells. Malaria parasites transform healthy red blood cells into rigid versions of themselves that clump together, hindering the transportation of oxygen. The infectious disease affects more than 200 million people across the world and causes nearly half a million deaths every year, according to the World Health Organization's 2018 report on malaria. Until now, however, researchers did not have a strong understanding of how the parasite so effectively infiltrated a system's red blood cells.
Mosquito Net offers protection against mosquitos, flies, and other insects, and thus against the diseases they may carry. Examples include malaria, dengue fever, yellow fever, zika virus and various forms of encephalitis, including the West Nile virus. To be effective the mesh of a mosquito net must be fine enough to exclude such insects without reducing visibility or air flow to unacceptable levels. It is possible to increase the effectiveness of a mosquito net greatly by treating it with an appropriate insecticide or mosquito repellant. Beds.
Molecular Pathology is an emerging discipline within pathology which is focused in the study and diagnosis of disease through the examination of molecules within organs, tissues or bodily fluids. Molecular pathology shares some aspects of practice with both anatomic pathology and clinical pathology, molecular biology, biochemistry, proteomics and genetics, and is sometimes considered a "crossover" discipline. It is multi-disciplinary in nature and focuses mainly on the sub-microscopic aspects of disease. A key consideration is that more accurate diagnosis is possible when the diagnosis is based on both the morphologic changes in tissues (traditional anatomic pathology) and on molecular testing.
Eradication of Infectious Diseases is the reduction of an infectious disease's prevalence in the global host population to zero.
Measles
Over the past 60 years, the number of new diseases cropping up in a decade has almost quadrupled. The number of outbreaks each year has more than tripled since 1980.
Toxins - Pesticides
 Epidemiology is the study and analysis
of the patterns,
causes and effects of health and disease conditions in
defined populations. It is the cornerstone of public health, and shapes
policy decisions and evidence-based practice by identifying risk factors
for disease and targets for preventive healthcare. Epidemiologists help
with study design, collection, and statistical analysis of data, amend
interpretation and dissemination of results (including peer review and
occasional systematic review). Epidemiology has helped develop methodology
used in clinical research, public health studies, and, to a lesser extent,
basic research in the biological
sciences.
Epidemiology is the study and analysis
of the patterns,
causes and effects of health and disease conditions in
defined populations. It is the cornerstone of public health, and shapes
policy decisions and evidence-based practice by identifying risk factors
for disease and targets for preventive healthcare. Epidemiologists help
with study design, collection, and statistical analysis of data, amend
interpretation and dissemination of results (including peer review and
occasional systematic review). Epidemiology has helped develop methodology
used in clinical research, public health studies, and, to a lesser extent,
basic research in the biological
sciences.Pathophysiology is a convergence of pathology with physiology. Pathology is the medical discipline that describes conditions typically observed during a disease state, whereas physiology is the biological discipline that describes processes or mechanisms operating within an organism. Pathology describes the abnormal or undesired condition, whereas pathophysiology seeks to explain the physiological processes or mechanisms whereby such condition develops and progresses. Pathophysiology can also mean the functional changes associated with or resulting from disease or injury. Another definition is the functional changes that accompany a particular disease.
Fast Spreading Diseases - Pandemic - Epidemic
Pandemic is an epidemic of infectious disease that has spread through human populations across a large region. An epidemic that is geographically widespread and prevalent over a whole country, multiple continents, or even worldwide. An infectious disease occurring throughout a region or even throughout the world and existing everywhere over a wide geographical area. Flu pandemics generally exclude recurrences of seasonal flu. Throughout history, there have been a number of pandemics, such as smallpox and tuberculosis. One of the most devastating pandemics was the Black Death, killing over 75 million people in 1350. The most recent pandemics include the HIV pandemic as well as the 1918 and 2009 H1N1 pandemics.
Emergency Preparedness for Disease Outbreaks (containment)
Epidemic is a widespread outbreak of an infectious disease where many people are infected at the same time or attacking or affecting many individuals in a community or a population simultaneously. Epidemic is the rapid spread of infectious disease to a large number of people in a given population within a short period of time, usually two weeks or less. A widespread endemic disease that is stable in terms of how many people are getting sick from it is not a pandemic. List of Epidemics (wiki).
Outbreak is a sudden spontaneous occurrence.
Endemic is a disease or condition that is regularly found among particular people or in a certain area. Systemic.
Epidemics: The Invisible Threat (video, 10.13.14, 52 min.)
Disease X represents a hypothetical, unknown pathogen that could cause a future epidemic. Disease X is a placeholder name that was adopted by the World Health Organization in February 2018 on their shortlist of blueprint priority diseases.
Coronavirus - Measles
The Andromeda Strain is a 1971 American science fiction thriller film about a team of scientists who investigate a deadly organism of extraterrestrial origin. After a U.S. government satellite crashes near the small rural town of Piedmont, New Mexico, on February 5, nearly all the residents are dead. A military recovery team from Vandenberg Air Force Base attempts to recover the satellite but dies while trying to do so. Suspecting that the satellite has brought back an alien organism, the military activates an elite team of scientists.
Improving Researchers' Abilities to Forecast Epidemics - Doomsday
Advances in AI can help prepare the world for the next pandemic, global group of scientists find. Scientists across Africa, America, Asia, Australia, and Europe outline for the first time how Artificial Intelligence can transform the landscape of infectious disease research and improve pandemic preparedness. Opportunities for AI and pandemic preparedness identified in the research include: Promising advances in improving current models of disease spread, aiming to make modelling more robust, accurate and realistic. Progress in pinpointing areas of high-transmission potential, helping ensure limited healthcare resources can be allocated in the most efficient possible way. Potential to improve genetic data in disease surveillance, ultimately accelerating vaccine development and the identification of new variants. Potential to help determine the properties of new pathogens, predict their traits and identify whether cross species jumps are likely. Predicting which new variants of already-circulating pathogens -- such as SARS-CoV-2 and influenza viruses -- might arise, and which treatments and vaccines are best in reducing their impact.
Possible AI-aided integration of population-level data with data from individual-level sources -- including wearable technologies such as heart rate and step counts -- to better detect and monitor outbreaks. AI can create a new interface between the highly technical science and healthcare professionals with limited training, improving capacity in settings that need these tools the most.
Newest doctors shun infectious diseases specialty. Thousands of doctors ready to continue their training celebrated Match Day for specialty fellowships on Nov. 30, but one group lamented its results, infectious diseases physicians. Despite its central role in the COVID pandemic, the infectious diseases specialty saw 44% of its training programs go unfilled. The most obvious reason is that the pay is low compared with other specialties. And on top of that, the field has long been understaffed, leading to long hours – a problem supercharged by the strain of the pandemic.
2002 - 2003 - Severe Acute Respiratory Syndrome-Related Coronavirus is a species of coronavirus that infects humans, bats and certain other mammals. It is an enveloped positive-sense single-stranded RNA virus that enters its host cell by binding to the ACE2 receptor. It is a member of the genus Betacoronavirus and subgenus Sarbecoronavirus. SARS (wiki).
2009 - Swine Influenza is an infection caused by any one of several types of swine influenza viruses. Swine influenza virus (SIV) or swine-origin influenza virus (S-OIV) is any strain of the influenza family of viruses that is endemic in pigs. As of 2009, the known SIV strains include influenza C and the subtypes of influenza A known as H1N1, H1N2, H2N1, H3N1, H3N2, and H2N3. Swine influenza virus is common throughout pig populations worldwide. Transmission of the virus from pigs to humans is not common and does not always lead to human flu, often resulting only in the production of antibodies in the blood. If transmission does cause human flu, it is called zoonotic swine flu. People with regular exposure to pigs are at increased risk of swine flu infection. It is estimated that in the 2009 flu pandemic 11–21% of the then global population (of about 6.8 billion), or around 700 million to 1.4 billion people, contracted the illness—more in absolute terms than the Spanish flu pandemic. However, with about 150,000–575,000 fatalities, it had a much lower case fatality rate. In August 2010, the World Health Organization declared the swine flu pandemic officially over. Subsequent cases of swine flu were reported in India in 2015, with over 31,156 positive test cases and 1,841 deaths up to March 2015.
2012–2013 - Middle East Respiratory Syndrome is a viral respiratory infection caused by the MERS-Coronavirus (MERS-CoV), is also known as camel flu. Symptoms may range from mild to severe. They include fever, cough, diarrhea and shortness of breath. Disease is typically more severe in those with other health problems. Mortality is about one-third of diagnosed cases. MERS-CoV is a betacoronavirus derived from bats. Camels have been shown to have antibodies to MERS-CoV but the exact source of infection in camels has not been identified. Camels are believed to be involved in its spread to humans but it is unclear how. Spread between humans typically requires close contact with an infected person. Its spread is uncommon outside of hospitals. Thus, its risk to the global population is currently deemed to be fairly low. As of 2020 there is no specific vaccine or treatment for the disease; a number of antiviral medications were being studied. The World Health Organization recommends that those who come in contact with camels wash their hands frequently and do not touch sick camels and that camel-based food products be appropriately cooked. Treatments that help with the symptoms may be given to those infected.
Ebola virus disease is a viral haemorrhagic fever of humans and other primates caused by ebolaviruses. Signs and symptoms typically start between two days and three weeks after contracting the virus with a fever, sore throat, muscular pain, and headaches. Vomiting, diarrhoea and rash usually follow, along with decreased function of the liver and kidneys. At this time, some people begin to bleed both internally and externally. The disease has a high risk of death, killing 25% to 90% of those infected, with an average of about 50%. This is often due to low blood pressure from fluid loss, and typically follows six to 16 days after symptoms appear. The virus spreads through direct contact with body fluids, such as blood from infected humans or other animals. Spread may also occur from contact with items recently contaminated with bodily fluids. Spread of the disease through the air between primates, including humans, has not been documented in either laboratory or natural conditions. Semen or breast milk of a person after recovery from EVD may carry the virus for several weeks to months. Fruit bats are believed to be the normal carrier in nature, able to spread the virus without being affected by it. Other diseases such as malaria, cholera, typhoid fever, meningitis and other viral haemorrhagic fevers may resemble EVD. Blood samples are tested for viral RNA, viral antibodies or for the virus itself to confirm the diagnosis. Control of outbreaks requires coordinated medical services and community engagement. This includes rapid detection, contact tracing of those who have been exposed, quick access to laboratory services, care for those infected, and proper disposal of the dead through cremation or burial. EVD outbreaks occur intermittently in tropical regions of sub-Saharan Africa. Between 1976 and 2013, the World Health Organization reports 24 outbreaks involving 2,387 cases with 1,590 deaths. The largest outbreak to date was the epidemic in West Africa, which occurred from December 2013 to January 2016, with 28,646 cases and 11,323 deaths. It was declared no longer an emergency on 29 March 2016. Other outbreaks in Africa began in the Democratic Republic of the Congo in May 2017, and 2018. In July 2019, the World Health Organization declared the Congo Ebola outbreak a world health emergency.
Angiotensin-Converting Enzyme 2 is an enzyme attached to the outer surface (cell membranes) of cells in the lungs, arteries, heart, kidney, and intestines. ACE2 lowers blood pressure by catalysing the cleavage of angiotensin II (a vasoconstrictor peptide) into angiotensin 1–7 (a vasodilator). ACE2 also serves as the entry point into cells for some coronaviruses. ACE2 counters the activity of the related angiotensin-converting enzyme (ACE) by reducing the amount of angiotensin-II and increasing Ang(1-7) making it a promising drug target for treating cardiovascular diseases. ACE2 is a single-pass type I membrane protein, with its enzymatically active domain exposed on the surface of cells in lungs and other tissues. The extracellular domain of ACE2 is cleaved from the transmembrane domain by another enzyme known as sheddase, and the resulting soluble protein is released into the blood stream and ultimately excreted into urine.
Black Death was the deadliest pandemic in recorded history. It killed an estimated 75–200 million people in Europe and the Mediterranean between 1346 and 1353. Plague is caused by the bacteria Yersinia pestis, a zoonotic bacteria usually found in small mammals and their fleas. People infected with Y. pestis often develop symptoms after an incubation period of one to seven days. There are two main clinical forms of plague infection: bubonic and pneumonic. Bubonic plague is the most common form and is characterized by painful swollen lymph nodes or 'buboes'. Plague is transmitted between animals and humans by the bite of infected fleas, direct contact with infected tissues, and inhalation of infected respiratory droplets. Plague can be a very severe disease in people, with a case-fatality ratio of 30% to 60% for the bubonic type, and is always fatal for the pneumonic kind when left untreated. Antibiotic treatment is effective against plague bacteria, so early diagnosis and early treatment can save lives. From 2010 to 2015 there were 3248 cases reported worldwide, including 584 deaths. Currently, the three most endemic countries are the Democratic Republic of the Congo, Madagascar, and Peru. New research published this month in the journal Nature, provides biological evidence that places the ancestral origins of Black Death in Central Asia, in what is now modern-day Kyrgyzstan.
How Black Death survivors gave their descendants an edge during pandemics. Using DNA extracted from teeth of people who died during and after the Black Death pandemic, researchers were able to identify genetic differences between those who survived and who died from the virus. When the bubonic plague arrived in London in 1348, the disease devastated the city. So many people died, so quickly, that the city's cemeteries filled up. In the end, this bubonic plague, known as the Black Death, likely killed 30 to 50% of people in parts of Europe and the United Kingdom. That's a mortality rate that's at least 200 times higher than the one estimated for COVID. Bubonic plague is one of three types of plague caused by the plague bacterium (Yersinia pestis).
New viruses that could cause epidemics on the horizon. Suddenly they appear and -- like the SARS-CoV-2 coronavirus -- can trigger major epidemics: Viruses that nobody had on their radar. They are not really new, but they have changed genetically. In particular, the exchange of genetic material between different virus species can lead to the sudden emergence of threatening pathogens with significantly altered characteristics. Using a new computer-assisted analysis method, we discovered 40 previously unknown nidoviruses in various vertebrates from fish to rodents, including 13 coronaviruses," reports DKFZ group leader Stefan Seitz. With the help of high-performance computers, the research team, which also includes Chris Lauber's working group from the Helmholtz Center for Infection Research in Hanover, has sifted through almost 300,000 data sets. According to virologist Seitz, the fact that we can now analyze such huge amounts of data in one go opens up completely new perspectives. Virus research is still in its relative infancy. Only a fraction of all viruses occurring in nature are known, especially those that cause diseases in humans, domestic animals and crops. The new method therefore promises a quantum leap in knowledge with regard to the natural virus reservoir.
System to auto-detect new variants will inform better response to future infectious disease outbreaks. Researchers have come up with a new way to identify more infectious variants of viruses or bacteria that start spreading in humans -- including those causing flu, COVID, whooping cough and tuberculosis. The new approach uses samples from infected humans to allow real-time monitoring of pathogens circulating in human populations, and enable vaccine-evading bugs to be quickly and automatically identified. This could inform the development of vaccines that are more effective in preventing disease. The approach can also quickly detect emerging variants with resistance to antibiotics. This could inform the choice of treatment for people who become infected -- and try to limit the spread of the disease. It uses genetic sequencing data to provide information on the genetic changes underlying the emergence of new variants. This is important to help understand why different variants spread differently in human populations. By creating 'family trees', the new approach identifies new variants automatically based on how much a pathogen has changed genetically, and how easily it spreads in the human population -- removing the need to convene experts to do this. It can be used for a broad range of viruses and bacteria and only a small number of samples, taken from infected people, are needed to reveal the variants circulating in a population. This makes it particularly valuable for resource-poor settings.
Contagion - Easy to Spread
Contagious is easily diffused or spread as from one person to another. A disease capable of being transmitted by infection.
Contagious Disease is easily spread from one person to another. A subset category of transmissible diseases, which are transmitted to other persons, either by physical contact with the person suffering the disease, or by casual contact with their secretions or objects touched by them or airborne route among other routes. Contagiousness varies between diseases. Non-contagious infections, by contrast, usually require a special mode of transmission between persons or hosts. These include need for intermediate vector species (mosquitoes that carry malaria) or by non-casual transfer of bodily fluid (such as transfusions, needle sharing or sexual contact). The boundary between contagious and non-contagious infectious diseases is not perfectly drawn, as illustrated classically by tuberculosis, which is clearly transmissible from person to person, but was not classically considered a contagious disease. In the present day, most sexually transmitted infections are considered contagious, but only some of them are subject to medical isolation. A disease may be known to be contagious but its causative factors remain undetermined. A contagion may be more infectious if the incubation period is long. Death Rate.
Transmissible is capable of being transmitted by infection. Isolation - Social Distancing.
Spread is to disperse widely and become distributed or widespread. Become widely known and passed on.
Diffused is to move outward or cause something to become widely known. Diffusing of light rays is when light is subjected to scattering by reflection from a rough surface or transmission through a translucent material.
Transmission is the passing of a pathogen causing communicable disease from an infected host individual or group to a particular individual or group, regardless of whether the other individual was previously infected. The term strictly refers to the transmission of microorganisms directly from one individual to another by one or more of the following means: Airborne – coughing, sneezing, breathing. Airborne infection – really small dry and wet particles that stay in the air for long periods of time allowing airborne contamination even after the departure of the host. Particle size < 5 μm. Droplet infection – small and usually wet particles that stay in the air for a short period of time. Contamination usually occurs in the presence of the host. Particle size > 5 μm. Direct physical contact – touching an infected individual, including sexual contact. Indirect physical contact – usually by touching a contaminated surface, including soil (fomite). Fecal-oral transmission – usually from unwashed hands, contaminated food or water sources due to lack of sanitation and hygiene, an important transmission route in pediatrics, veterinary medicine and developing countries. Transmission can also be indirect, via another organism, either a vector (e.g. a mosquito or fly) or an intermediate host (e.g. tapeworm in pigs can be transmitted to humans who ingest improperly cooked pork). Indirect transmission could involve zoonoses or, more typically, larger pathogens like macroparasites with more complex life cycles. Transmissions can be autochthonous (i.e. between two individuals in the same place) or may involve travel of the microorganism or the affected hosts.
Airborne Disease is any disease that is caused by pathogens that can be transmitted through the air over time and distance by small particles. Such diseases include many of considerable importance both in human and veterinary medicine. The relevant pathogens may be viruses, bacteria, or fungi, and they may be spread through breathing, talking, coughing, sneezing, raising of dust, spraying of liquids, toilet flushing or any activities which generate aerosol particles or droplets. Human airborne diseases do not include conditions caused by air pollution such as Volatile Organic Compounds (VOCs), gases and any airborne particles. Airborne transmission is distinct from transmission by respiratory droplets, which are large enough (usually greater than 5 µm) to fall to the ground rapidly after being produced. Airborne virus has long been considered to be a virus that spreads in exhaled particles that are tiny enough to linger in the air and move with air currents, letting them be breathed in by passersby who then get sick. Measles is a good example of this kind of virus — an exhaled measles pathogen can hang suspended in a room for a couple hours after an infected person leaves. Currently available research supports the possibility that SARS-CoV-2 could be spread via bioaerosols generated directly by patients' exhalation. fine particles emitted when someone breathes that can be suspended in the air rather than larger droplets produced through coughs and sneezes. Droplets are larger respiratory particles that are 5 to 10 micrometers in size. Those are considered "big," even though a 5 micrometer particle would still be invisible to the naked eye. Traditionally, those droplets are thought to not travel more than about three feet or so after exhalation. That would mean the virus can only spread to people who get close to an infected person or who touch surfaces or objects that might have become contaminated by these droplets. This is why public health messages urge people to wash their hands and stand at least 6 feet away from other people. Number Needed to Treat.
Bioaerosol are a subcategory of particles released from terrestrial and marine ecosystems into the atmosphere. They consist of both living and non-living components, such as fungi, pollen, bacteria and viruses. Common sources of bioaerosols include soil, water, and sewage. Bioaerosols are typically introduced into the air via wind turbulence over a surface. Once in the atmosphere, they can be transported locally or globally: common wind patterns/strengths are responsible for local dispersal, while tropical storms and dust plumes can move bioaerosols between continents. Over ocean surfaces, bioaerosols are generated via sea spray and bubbles. Bioaerosols can transmit microbial pathogens, endotoxins, and allergens to which humans are sensitive. A well-known case was the meningococcal meningitis outbreak in sub-Saharan Africa, which was linked to dust storms during dry seasons. Other outbreaks linked to dust events including Mycoplasma pneumonia and tuberculosis. Another instance was an increase in human respiratory problems in the Caribbean that may have been caused by traces of heavy metals, microorganism bioaerosols, and pesticides transported via dust clouds passing over the Atlantic Ocean.
Zoonosis is an infectious disease caused by bacteria, viruses, or parasites that spread from non-human animals to humans. A Bat could have a virus and then give it to an intermediate host like a pangolin or a snake, and then the pangolin or a snake could pass it on to a human. Then a human could even transmit back to animals.
Deforestation - Factory Farms - Over Development
Cross-Species Transmission is the transmission of an infectious pathogen, such as a virus, between hosts belonging to different species. Once introduced into an individual of a new host species, the pathogen may cause disease for the new host and/or acquire the ability to infect other individuals of the same species, allowing it to spread through the new host population. The phenomenon is most commonly studied in virology, but cross-species transmission may also occur with bacterial pathogens or other types of microorganisms. CST is also called interspecies transmission, host jump, or spillover.
Spillover Infection occurs when a reservoir population with a high pathogen prevalence comes into contact with a novel host population. The pathogen is transmitted from the reservoir population and may or may not be transmitted within the host population. Spillover is a common event; in fact, more than two-thirds of human viruses are zoonotic. Most spillover events result in self-limited cases with no further human to human transmission, as occurs, for example, with rabies, anthrax, histoplasmosis or hidatidosis. Other zoonotic pathogens are able to be transmitted by humans to produce secondary cases and even to establish limited chains of transmission. Some examples are the Ebola and Marburg filoviruses, the MERS and SARS coronaviruses or some avian flu viruses. Finally, some few spillover events can result in the final adaptation of the microbe to the humans, who became a new stable reservoir, as occurred with the HIV virus resulting in the AIDS epidemic. In fact, most of the pathogens which are presently exclusive of humans were probably transmitted by other animals sometime in the past. If the history of mutual adaptation is long enough, permanent host-microbe associations can be established resulting in co-evolution, and even on permanent integration of the microbe genome in the human genome, as it is the case of endogenous viruses. The closer the two species are in phylogenetic terms, the easier it is for microbes to overcome the biological barrier to produce successful spillovers. For this reason, other mammals are the main source of zoonotic agents for humans. Zoonotic spillover has increased in the last 50 years, mainly due to the environmental impact of agriculture, that promotes deforestation, changing wildlife habitat, and the impacts of increased land use. Spillover infection is also known as pathogen spillover and spillover event.
Waterborne Diseases are conditions caused by pathogenic micro-organisms that are transmitted in water. These diseases can be spread while bathing, washing, drinking water, or by eating food exposed to contaminated water. While diarrhea and vomiting are the most commonly reported symptoms of waterborne illness, other symptoms can include skin, ear, respiratory, or eye problems
Vector in epidemiology is any agent which carries and transmits an infectious pathogen into another living organism; most agents regarded as vectors are organisms, such as intermediate parasites or microbes, but it could be an inanimate medium of infection such as dust particles.
Communicable Disease is a disease that is transmitted through direct contact with an infected individual or indirectly through a vector. Non-Communicable Disease is a disease that is not transmissible directly from one person to another.
 Infection Rate is the probability or risk of an infection in a
population. It is used to measure the frequency of occurrence of new
instances of infection within a population during a specific time period.
Epidemic Disease Occurrence.
Infection Rate is the probability or risk of an infection in a
population. It is used to measure the frequency of occurrence of new
instances of infection within a population during a specific time period.
Epidemic Disease Occurrence.Transmission Risks and Rates Transmission of an infection requires three conditions: An infectious individual. A susceptible individual. An effective contact between them. An effective contact is defined as any kind of contact between two individuals such that, if one individual is infectious and the other susceptible, then the first individual infects the second. Whether or not a particular kind of contact will be effective depends on the infectious agent and its route of transmission. Mutations.
Susceptible Individual is a member of a population who is at risk of becoming infected by a disease. Susceptibles have been exposed to neither the wild strain of the disease nor a vaccination against it, and thus have not developed immunity.
Basic Reproduction Number the expected number of cases directly generated by one case in a population where all individuals are susceptible to infection. The definition describes the state where no other individuals are infected or immunized naturally or through vaccination. Some definitions, such as that of the Australian Department of Health, add absence of "any deliberate intervention in disease transmission". The basic reproduction number is not to be confused with the effective reproduction number R, which is the number of cases generated in the current state of a population, which does not have to be the uninfected state. By definition, R0 cannot be modified through vaccination campaigns. Also, it is important to note that R0 is a dimensionless number and not a rate, which would have units of time-1, or units of time like doubling time. R0 is not a biological constant for a pathogen as it is also affected by other factors such as environmental conditions and the behavior of the infected population. Furthermore R0 values are usually estimated from mathematical models, and the estimated values are dependent on the model used and values of other parameters. Thus values given in the literature only make sense in the given context and it is recommended not to use obsolete values or compare values based on different models. R0 does not by itself give an estimate of how fast an infection spreads in the population. The most important uses of R0 are determining if an emerging infectious disease can spread in a population and determining what proportion of the population should be immunized through vaccination to eradicate a disease. In commonly used infection models, when R0 > 1 the infection will be able to start spreading in a population, but not if R0 < 1. Generally, the larger the value of R0, the harder it is to control the epidemic. For simple models, the proportion of the population that needs to be effectively immunized (meaning not susceptible to infection) to prevent sustained spread of the infection has to be larger than 1 - 1/R0. Conversely, the proportion of the population that remains susceptible to infection in the endemic equilibrium is 1/R0. The basic reproduction number is affected by several factors including the duration of infectivity of affected patients, the infectiousness of the organism, and the number of susceptible people in the population that the affected patients are in contact with. (Basic reproduction rate is sometimes called basic reproductive ratio, or incorrectly basic reproductive rate, and denoted R0, pronounced R nought or R zero). R-O = 1.5 reproduction rate.
People have an average of 16 contacts per day. There are many short-duration contacts (four contacts per day per person are less than 30 min) representing casual interactions. Social Contacts and Mixing Patterns Relevant to the Spread of Infectious Diseases. If you spend a few minutes with an infected person, you have around a 10% chance of being infected, and an even higher chance for infection if you are not aware or trained on how to protect yourself.
Index Case or Patient Zero is the first documented patient in a disease epidemic within a population, or the first documented patient included in an epidemiological study. It can also refer to the first case of a condition or syndrome (not necessarily contagious) to be described in the medical literature, whether or not the patient is thought to be the first person affected. An index case can achieve the status of a "classic" case study in the literature, as did Phineas Gage, the first known person to exhibit a definitive personality change as a result of a brain injury.
Depletion-of-Susceptibles bias in influenza vaccine waning studies: how to ensure robust results. Evidence of the depletion of susceptibles effect in non-experimental pharmacoepidemiologic research.
A model for the spread and control of pandemic influenza in an isolated geographical region. Ee postulated 12 control scenarios that combined social distancing, targeted antiviral treatment and antiviral prophylaxis (TATP) and home quarantine. For each, we calculated the value of Rc and the proportion of the population infected in an epidemic under the application of selected control scenarios. Structured Kermack–McKendrick integral equation model to describe the spread of a novel influenza-like virus in an isolated population.
Environmental Persistence of Influenza Viruses Is Dependent upon Virus Type and Host Origin. Highly transmissible influenza viruses (IV) must remain stable and infectious under a wide range of environmental conditions following release from the respiratory tract into the air. Understanding how expelled IV persist in the environment is critical to limiting the spread of these viruses.
A note on the derivation of epidemic final sizes. Final size relations are known for many epidemic models. The derivations are often tedious and difficult, involving indirect methods to solve a system of integro-differential equations.
Viral Shedding refers to the expulsion and release of virus progeny following successful reproduction during a host-cell infection. Once replication has been completed and the host cell is exhausted of all resources in making viral progeny, the viruses may begin to leave the cell by several methods. The term is used to refer to shedding from a single cell, shedding from one part of the body into another part of the body, and shedding from bodies into the environment where the viruses may infect other bodies.
Superspreading Event is an event in which an infectious disease is spread much more than usual, while an unusually contagious organism infected with a disease is known as a superspreader. In the context of a human-borne illness, a superspreader is an individual who is more likely to infect others, compared with a typical infected person. Such superspreaders are of particular concern in epidemiology. Some cases of superspreading conform to the 80/20 rule, where approximately 20% of infected individuals are responsible for 80% of transmissions, although superspreading can still be said to occur when superspreaders account for a higher or lower percentage of transmissions. In epidemics with such superspreader events, the majority of individuals infect relatively few secondary contacts. SSEVs are shaped by multiple factors including a decline in herd immunity, nosocomial infections, virulence, viral load, misdiagnosis, airflow dynamics, immune suppression, and co-infection with another pathogen.
Reducing COVID-19 spread. Researchers have found that physical distancing is universally effective at reducing the spread of COVID-19, while social bubbles and masks are more situation-dependent. The researchers developed a model to test the effectiveness of measures such as physical distancing, masks or social bubbles when used in various settings. The researchers incorporated data from reports of outbreaks at a range of events, such as parties, meals, nightclubs, public transit and restaurants. The researchers say that an individual's chances of becoming infected with COVID-19 depend heavily on the transmission rate and the duration -- the amount of time spent in a particular setting. Events were categorized as saturating (high transmission probability) or linear (low transmission probability). Examples of high transmission settings include bars, nightclubs and overcrowded workplaces while low transmission settings include public transit with masks, distancing in restaurants and outdoor activities. The model suggests that physical distancing was effective at reducing COVID-19 transmission in all settings but the effectiveness of social bubbles depends on whether chances of transmission are high or low. In settings where there is mixing and the probability of transmission is high, such as crowded indoor workplaces, bars and nightclubs and high schools, having strict social bubbles can help reduce the spread of COVID-19. The researchers found that social bubbles are less effective in low transmission settings or activities where there is mixing, such as engaging in outdoor activities, working in spaced offices or travelling on public transportation wearing masks. They note that masks and other physical barriers may be less effective in saturating, high transmission settings (parties, choirs, restaurant kitchens, crowded offices, nightclubs and bars) because even if masks halve the transmission rates that may not have much impact on the transmission probability (and so on the number of infections).
Host - Harbor - Carrier
Host in biology is an organism that harbors a parasitic, a mutualistic, or a commensalist guest (symbiont), the guest typically being provided with nourishment and shelter. Examples include animals playing host to parasitic worms (e.g. nematodes), cells harbouring pathogenic (disease-causing) viruses, a bean plant hosting mutualistic (helpful) nitrogen-fixing bacteria. More specifically in botany, a host plant supplies food resources to micropredators, which have an evolutionarily stable relationship with their hosts similar to ectoparasitism. The host range is the collection of hosts that an organism can use as a partner. Definitive or Primary Host - an organism in which the parasite reaches maturity and reproduces sexually, if possible. This is the final host. Secondary or Intermediate Host - an organism that harbors the sexually immature parasite and is required by the parasite to undergo development and complete its life cycle. It often acts as a vector of the parasite to reach its definitive host. For example, Dirofilaria immitis, the heartworm of dogs, uses the mosquito as its intermediate host until it matures into the infective L3 larval stage. Paratenic Host - an organism that harbors the sexually immature parasite but is not necessary for the parasite's development cycle to progress. Paratenic hosts serve as "dumps" for non-mature stages of a parasite in which they can accumulate in high numbers. The trematode Alaria americana may serve as an example: the so-called mesocercarial stages of this parasite reside in tadpoles, which are rarely eaten by the definitive canine host. The tadpoles are more frequently preyed on by snakes, in which the mesocercariae may not undergo further development. However, the parasites may accumulate in the snake paratenic host and infect the definitive host once the snake is consumed by a canid. The nematode Skrjabingylus nasicola is another example, with slugs as the intermediate hosts, shrews and rodents as the paratenic hosts, and mustelids as the definitive hosts. Dead-end, Incidental, or Accidental Host - an organism that generally does not allow transmission to the definitive host, thereby preventing the parasite from completing its development. For example, humans and horses are dead-end hosts for West Nile virus, whose life cycle is normally between culicine mosquitoes and birds. People and horses can become infected, but the level of virus in their blood does not become high enough to pass on the infection to mosquitoes that bite them. Reservoir Host - an organism that harbors a pathogen but suffers no ill effects. However, it serves as a source of infection to other species that are susceptible, with important implications for disease control. A single reservoir host may be reinfected several times. Dormant.
Fomite is any inanimate object that, when contaminated with or exposed to infectious agents (such as pathogenic bacteria, viruses or fungi), can transfer disease to a new host. In the 21st century, the role of fomites in disease transfer is higher than ever in human history because of the indoor lifestyle.
A Genetic Rearrangement of Red Blood Cell Glycophorin Receptors that confers a 40 percent reduced risk from severe Malaria.
Scientists discover off-switch for ‘Molecular Machine’ active in many diseases. Researchers have uncovered how an inflammation process automatically switches off in healthy cells.
The Brain Detects Disease in others even before it breaks out. Our sense of vision and smell alone are enough to make us aware that someone has a disease even before it breaks out. Herd Immunity.
Wash Your Hands - Soap - Disinfect - Clean
Keeping Hands Clean is one of the most important steps that you can take to avoid getting sick and spreading germs to others. Though ordinary soap diluted in water is sufficient to rupture and kill many types of bacteria and viruses, soap and water does not always kill germs, but good hand washing works by removing germs from your hands, which is why 20 seconds of good Hand Washing is sometimes necessary. Water is a solvent, but it needs a little extra help sometimes.
Protect Yourself from Viruses. If sick, limit contact with others as much as possible to keep from infecting them. Avoid close contact with sick people. Wash your hands often with soap and water.
Avoid touching your eyes, nose and mouth because germs spread this way.
When you cough or sneeze, it's a good idea to cover your nose and mouth with a tissue and then throw out your used tissue. If you don’t have a tissue, then cough or sneeze into your upper sleeve or elbow, not into your hands.
Hand Washing - Good Hygiene - Bathing (skin)
Think Twice - Food Safety - Air Purification
Infections - Antiviral Drug - Pathogens - Biofilms - Colds - Resistance
Disinfect is to clean something, especially with a chemical, in order to destroy bacteria, microorganisms or pathogens.
Clean or cleaning is to remove unwanted substances like dirt and filth from a surface and make it free from impurities or infection. Cleanliness is being clean and free from germs, dirt, trash, or waste, and the habit of achieving and maintaining that state. Stain Removing Tips (image).
Soap is made from fats and oils that react with lye (sodium hydroxide). Solid fats like coconut oil, palm oil, tallow (rendered beef fat), or lard (rendered pork fat), are used to form bars of soap that stay hard and resist dissolving in the water left in the soap dish. Solid soap, because of its reusable nature, may hold bacteria acquired from previous uses. The CDC still states "liquid soap with hands-free controls for dispensing is preferable. Soap is made of pin-shaped molecules, each of which has a hydrophilic head, it readily bonds with water and a hydrophobic tail, which shuns water and prefers to link up with oils and fats. These molecules, when suspended in water, alternately float about as solitary units, interact with other molecules in the solution and assemble themselves into little bubbles called micelles, with heads pointing outward and tails tucked inside. When you wash your hands with soap and water, you surround any microorganisms on your skin with soap molecules. The hydrophobic tails of the free-floating soap molecules attempt to evade water; in the process, they wedge themselves into the lipid envelopes of certain microbes and viruses, prying them apart.
Carbolic Soap is a mildly antiseptic soap containing carbolic acid and/or cresylic acid, both of which are phenols derived from either coal tar or petroleum sources. Lifebuoy Soap.
Vegan Soap are made from fats or oils of vegetable origin rather than from saponified tallow or other animal fats. In addition to fats, the other main ingredient is either wood ash, potassium hydroxide or sodium hydroxide.
Castile Soap is an olive-oil-based hard soap made in a style similar to that originating in the Castile region of Spain.
Antibacterial Soap is a soap which contains chemical ingredients that purportedly assist in killing bacteria. The majority of antibacterial soaps contain triclosan, though other chemical additives are also common.
Glycerin Soap is a soap that contains glycerin, a component of fat or oil.
Ivory Soap bar contains sodium tallowate, sodium cocoate or sodium palm kernelate, water, sodium chloride, sodium silicate, magnesium sulfate, and fragrance. The soap bar has a determined pH value: 9.5 and new varieties of Ivory soap contain altered ingredients, such as in "Simply Ivory" (or "simplement ivory"): sodium tallowate and/or sodium palmate, water, sodium cocoate or sodium palm kernelate, glycerin, sodium chloride, fragrance, one or more of the following: coconut acid, palm kernel acid, tallow acid or palmitic acid, and tetrasodium EDTA. The additional ingredients primarily are to reduce the harshness of the soap, since additional glycerin and fatty acids are typically used for that. Tetrasodium EDTA is primarily to reduce soap scum formation. Bars of Ivory now come without the words "soap" or "float" on the packaging, and they are made with the latter formula. The optimal range for pH-balanced skincare products is between 4 and 6.
New, biological, and safer soaps. Surfactants are synthesized from petroleum and are the main active ingredient in most soaps, detergents, and shampoos. Biosurfactants, produced by bacteria, are safer and can replace synthetic surfactants. Rhamnolipid molecules are some of the safest surfactants known and are particularly attractive, thanks to their biodegradability, minimal toxicity, and amenability to be produced from industrial waste. But there's a problem. They are made using Pseudomonas aeruginosa, a pathogenic bacterium harmful to humans.
Hand Sanitizer is a liquid generally used to decrease infectious agents on the hands. Formulations of the alcohol-based type are preferable to hand washing with soap and water in most situations in the healthcare setting.
Antiseptic are antimicrobial substances that are applied to living tissue/skin to reduce the possibility of infection, sepsis, or putrefaction. Antiseptics are generally distinguished from antibiotics by the latter's ability to safely destroy bacteria within the body, and from disinfectants, which destroy microorganisms found on non-living objects. Some antiseptics are true germicides, capable of destroying microbes (bacteriocidal), while others are bacteriostatic and only prevent or inhibit their growth. Antibacterials include antiseptics that have the proven ability to act against bacteria. Microbicides which destroy virus particles are called viricides or antivirals. Antifungals, also known as an antimycotics, are pharmaceutical fungicides used to treat and prevent mycosis (fungal infection).
Disinfectant are antimicrobial agents that are applied to the surface of non-living objects to destroy microorganisms that are living on the objects. Disinfection does not necessarily kill all microorganisms, especially resistant bacterial spores; it is less effective than sterilization, which is an extreme physical and/or chemical process that kills all types of life. Disinfectants are different from other antimicrobial agents such as antibiotics, which destroy microorganisms within the body, and antiseptics, which destroy microorganisms on living tissue. Disinfectants are also different from biocides — the latter are intended to destroy all forms of life, not just microorganisms. Disinfectants work by destroying the cell wall of microbes or interfering with their metabolism. Sanitizers are substances that simultaneously clean and disinfect. Disinfectants are frequently used in hospitals, dental surgeries, kitchens, and bathrooms to kill infectious organisms. Bacterial endospores are most resistant to disinfectants, but some viruses and bacteria also possess some tolerance. Disinfectants are used to rapidly kill bacteria. They kill off the bacteria by causing the proteins to become damaged and outer layers of the bacteria cell to rupture. The DNA material subsequently leaks out. In wastewater treatment, a disinfection step with chlorine, ultra-violet (UV) radiation or ozonation can be included as tertiary treatment to remove pathogens from wastewater, for example if it is to be reused to irrigate golf courses. An alternative term used in the sanitation sector for disinfection of waste streams, sewage sludge or fecal sludge is sanitisation or Sanitization. - Water Filters.
Hypochlorous Acid is a weak acid that forms when chlorine dissolves in water, and itself partially dissociates, forming hypochlorite, ClO-. HClO and ClO- are oxidizers, and the primary disinfection agents of chlorine solutions. HClO cannot be isolated from these solutions due to rapid equilibration with its precursor. Sodium hypochlorite (NaClO) and calcium hypochlorite (Ca(ClO)2), are bleaches, deodorants, and disinfectants.
Contamination is the presence of an unwanted constituent, harmful substance or impurity in a material, physical body, natural environment, workplace, etc.
Cross-Contamination - Allergies - Food Safety - Superbugs - Infection Prevention in Aging
Multidrug-Resistant Organisms in Hospitals: What Is on Patient Hands and in their Rooms? Healthcare workers' hands are still the primary mode of microbe transmission to patients. But hospital room surfaces like the nurse call button can also have germs.
Pneumonia-Causing Bacteria can be spread by Nose Picking and Rubbing.
Sterilization in microbiology refers to any process that eliminates, removes, kills, or deactivates all forms of life and other biological agents (such as fungi, bacteria, viruses, spore forms, prions, unicellular eukaryotic organisms such as Plasmodium, etc.) present in a specified region, such as a surface, a volume of fluid, medication, or in a compound such as biological culture media. Sterilization can be achieved through various means, including: heat, chemicals, irradiation, high pressure, and filtration. Sterilization is distinct from disinfection, sanitization, and pasteurization, in that sterilization kills, deactivates, or eliminates all forms of life and other biological agents which are present.
The Potentially Deadly Bacterium that's on everyone's Skin. A close relative of MRSA, Staphylococcus epidermidis, is a major cause of life-threatening infections after surgery, but it is often overlooked by clinicians and scientists because it is so abundant. They have identified a set of 61 genes that allow this normally harmless skin bacterium to cause life-threatening illness.
Staphylococcus Epidermidis is a Gram-positive bacterium, and one of over 40 species belonging to the genus Staphylococcus. It is part of the normal human flora, typically the skin flora, and less commonly the mucosal flora. It is a facultative anaerobic bacteria. Although S. epidermidis is not usually pathogenic, patients with compromised immune systems are at risk of developing infection. These infections are generally hospital-acquired. S. epidermidis is a particular concern for people with catheters or other surgical implants because it is known to form biofilms that grow on these devices. Being part of the normal skin flora, S. epidermidis is a frequent contaminant of specimens sent to the diagnostic laboratory.
Plasma device designed for consumers can quickly disinfect surfaces. Plasma-based disinfectant and sanitizer proves 99% effective at killing bacteria and now is being tested on deactivating virus. The COVID-19 pandemic has cast a harsh light on the urgent need for quick and easy techniques to sanitize and disinfect everyday high-touch objects such as doorknobs, pens, pencils, and personal protective gear worn to keep infections from spreading. Now scientists at the U.S. Department of Energy's (DOE) Princeton Plasma Physics Laboratory and the New Jersey Institute of Technology (NJIT) have demonstrated the first flexible, hand-held, device based on low-temperature plasma -- a gas that consists of atoms, molecules, and free-floating electrons and ions -- that consumers can quickly and easily use to disinfect surfaces without special training. The room-temperature plasma interacts with air to produce what are called reactive oxygen and nitrogen species -- molecules and atoms of the two elements -- along with a mixture of electrons, currents, and electrical fields. The electrons and fields team up to enable the reactive species to penetrate and destroy bacteria cell walls and kill the cells. Room-temperature plasmas, which compare with the fusion plasmas PPPL studies that are many times hotter than the core of the sun, are produced by sending short pulses of high-speed electrons through gases like air, creating the plasma and leaving no time for it to heat up. Such plasmas are also far cooler than the thousand-degree plasmas that the laboratory studies to synthesize nanoparticles and conduct other research. A special feature of the device is its ability to improve the action of hydrogen peroxide, a common antiseptic cleanser. "We demonstrate faster disinfection than plasma or hydrogen peroxide alone in stable low power operation," the authors write. "Hence, plasma activation of a low concentration hydrogen peroxide solution, using a hand-held flexible DBD device results in a dramatic improvement in disinfection."
Space Station gets a bacteria-killing upgrade using an antimicrobial metal surface that explodes bacteria on contact. Coating called AGXX, which consists of thin layers of the metals silver and ruthenium treated with vitamin C. AGXX works via a redox reaction between the silver and ruthenium, producing free radicals that damage bacterial cell membranes. Over time, some bacteria grew, but by 19 months there were 80% fewer strains on the AGXX than the steel control. Spacecraft are ripe environments for bacterial resistance, partly because there isn’t the normal competition between the human-associated bacteria and bugs from environment. Certain strains develop thicker cell walls and others multiply faster in microgravity.
Far-UVC Light: A new tool to control the spread of airborne-mediated microbial diseases. Germicidal ultraviolet light, typically at 254 nm, if used directly, can be a health hazard to skin and eyes. But far-UVC light (207–222 nm) efficiently kills pathogens potentially without harm to exposed human tissues. A 9-Watt Near-UV Light Disinfecting A19 E26 LED Light Bulb, 800 Lumens, 3000 Kelvin, Non-Dimmable.
Researchers use ultrasound waves to move objects hands-free. Contactless manipulation method could be used in industries such as robotics and manufacturing. While it's been demonstrated before that light and sound waves can manipulate objects, the objects have always been smaller than the wavelength of sound or light, or on the order of millimeters to nanometers, respectively. The University of Minnesota team has developed a method that can move larger objects using the principles of metamaterial physics. Metamaterials are materials that are artificially engineered to interact with waves, like light and sound. By placing a metamaterial pattern on the surface of an object, the researchers were able to use sound to steer it in a certain direction without physically touching it.
Take off your Shoes when entering a Home. A study done by the University of Arizona found an average of 421,000 different bacteria on shoes. Coliforms, a bacterial indicator of the level of sanitation of foods and water (and universally present in feces), were detected on the bottoms of 96% of shoes.
Masks - Air Filtration
 Surgical Mask may keep you from spreading germs, but it will not
effectively protect you
from breathing in tiny viruses that can easily get through the mask and
around the mask where it's lose and not sealed against the face. A
N95
Respirator Mask is more effective as long as it's fitted properly and not
worn for several hours because it also restricts oxygen flow. Don't wear a
face mask if you are not sick. Face masks are for sick people and health
care providers. Leave the face masks in stores for the doctors and the
nurses and the sick people, unless you can
make your own mask. The N95 is the USA standard. The KN95 is the
China standard. The KF94 is the Korean standard. FFP2 is the EU standard.
The most commonly known respirator rating is the
NIOSH system, which rates
masks as N95, N99, and N100. These masks are rated by the
American National Institute
for Occupational Safety and health, which is part of the CDC. The
number on a
NIOSH rated masks signifies the
filtration
effectiveness of the
filter. For
example, an
N95 mask is required to stop AT LEAST 95% of particles of 0.3
microns in size. An R95 mask will also filter out at least 95% of
0.3-micron particles. The only difference comes in with N100 and P100
rated masks. Complete filtration is at this point impossible, and a 100
rated mask is effective at stopping 99.97% of 0.3-micron particles. Hong
Kong inventor unveils reusable masks he
says employ UV rays, ‘photocatalytic coating’ to disinfect in storage,
Stark Chan, who rose to fame as a teen tech prodigy, says the coating on
the masks’ exterior releases a substance that can kill bacteria and
viruses. The tech entrepreneur said while the new masks have no formal
certification, a local university has found them more effective than
surgical masks. Company launches ultraviolet disinfectant that makes a
single-use mask reusable.
A Novel Anti-Influenza Copper Oxide Containing Respiratory Face Mask.
N95 filtering face piece
respirator
decontamination that would allow it to be reused multiple times
instead of throwing away after one use.
Surgical Mask may keep you from spreading germs, but it will not
effectively protect you
from breathing in tiny viruses that can easily get through the mask and
around the mask where it's lose and not sealed against the face. A
N95
Respirator Mask is more effective as long as it's fitted properly and not
worn for several hours because it also restricts oxygen flow. Don't wear a
face mask if you are not sick. Face masks are for sick people and health
care providers. Leave the face masks in stores for the doctors and the
nurses and the sick people, unless you can
make your own mask. The N95 is the USA standard. The KN95 is the
China standard. The KF94 is the Korean standard. FFP2 is the EU standard.
The most commonly known respirator rating is the
NIOSH system, which rates
masks as N95, N99, and N100. These masks are rated by the
American National Institute
for Occupational Safety and health, which is part of the CDC. The
number on a
NIOSH rated masks signifies the
filtration
effectiveness of the
filter. For
example, an
N95 mask is required to stop AT LEAST 95% of particles of 0.3
microns in size. An R95 mask will also filter out at least 95% of
0.3-micron particles. The only difference comes in with N100 and P100
rated masks. Complete filtration is at this point impossible, and a 100
rated mask is effective at stopping 99.97% of 0.3-micron particles. Hong
Kong inventor unveils reusable masks he
says employ UV rays, ‘photocatalytic coating’ to disinfect in storage,
Stark Chan, who rose to fame as a teen tech prodigy, says the coating on
the masks’ exterior releases a substance that can kill bacteria and
viruses. The tech entrepreneur said while the new masks have no formal
certification, a local university has found them more effective than
surgical masks. Company launches ultraviolet disinfectant that makes a
single-use mask reusable.
A Novel Anti-Influenza Copper Oxide Containing Respiratory Face Mask.
N95 filtering face piece
respirator
decontamination that would allow it to be reused multiple times
instead of throwing away after one use.
Why Wearing a Mask Works (image) - Infrared video shows the risks of airborne coronavirus spread (youtube).
You have a 67% chance of being infected when you're not wearing a mask. You have a 16% chance of being infected when you are wearing a mask. In Hong Cong, 96% of the people wear masks. The infection rate was 0.04%.
Surgical Mask is intended to be worn by health professionals during surgery and during nursing to catch the bacteria shed in liquid droplets and aerosols from the wearer's mouth and nose. They are not designed to protect the wearer from inhaling airborne bacteria or virus particles and are less effective than respirators, such as N95 or NIOSH masks, which provide better protection due to their material, shape and tight seal. Flu.
Protective Masks are pieces of kit or equipment worn on the head and face to afford protection to the wearer, and today usually have these functions: Providing a supply of air or filtering the outside air (respirators and dust masks). Protecting the face against flying objects or dangerous environments, while allowing vision.
Elastomeric masks provide a more durable, less costly option for health care workers. Use of elastomeric masks reduces the number of N95 masks needed by nearly 95 percent in one month. UV-C light is effective for killing COVID-19 on N95s, study demonstrates.
NIOSH Air Filtration Rating refers to the publications of National Institute for Occupational Safety and Health of US government pertaining to respirators and masks worn to filter contaminated air, regardless of cause. The first part of the filter's classification uses the letters N, R, or P to indicate the filter's ability to function when exposed to petroleum. "N" = not resistant to petroleum. "R" = somewhat resistant to petroleum. "P" = strongly resistant to petroleum. The second part lists the percentage of particles that the mask is certified to block (such as 95 or 97 percent). The most common is N95, which is recommended by the US Centers for Disease Control and Prevention for most cases of air contamination. These filters are designed to seal tightly around mouth and nose and are made of material certified to block 95% of particles 0.3 μm or larger in diameter, roughly the size of a single virus and include PM2.5.
Safety Engineering - Occupational Hazards - Hazmat Suit - Medical Face Shield
Homemade Face Masks may be a Combination of Two Fabrics. One layer of a tightly woven cotton sheet combined with two layers of polyester-spandex chiffon, which is a sheer fabric often used in evening gowns, can filter out the most aerosol particles (80-99%, depending on particle size), with performance close to that of an N95 mask material. Substituting the chiffon with natural silk or flannel, or simply using a cotton quilt with cotton-polyester batting, produced similar results. The researchers point out that tightly woven fabrics, such as cotton, can act as a mechanical barrier to particles, whereas fabrics that hold a static charge, like certain types of chiffon and natural silk, serve as an electrostatic barrier. However, a 1% gap reduced the filtering efficiency of all masks by half or more, emphasizing the importance of a properly fitted mask.
Why is it So Hard Not to Touch your Face? Touching your face is a perfect example of a habit. You often experience small itches on your face, because of the many sensory receptors in the skin of your face and mucous membranes. The motions you need to make to move your arms and hands to touch your face in a particular place are roughly the same each time you do it, and you have been practicing these motions your whole life. As a result, responding to an itch or small pain with a touch is easy to do without thinking about it. To stop yourself from engaging in this action, there are two effortful processes you have to go through. First, you have to be mindful of an action you have performed your whole life mindlessly. That is hard. Second, to stop yourself from doing something that your motivational system has engaged, you have to activate a second circuit in the motivational system that stops actions that have been engaged. This inhibition system is effortful to engage and can be disrupted by stress or distraction. you need to reprogram your habit system to perform a different action and teach your motivational system something new and more beneficial. Of course there will be times when you will eventually touch your face without thinking about it. But over time, you will become more and more aware it and start exercising control. Don't rub your eyes. Don't bite your fingernails. Don't wipe your nose on the back of your hand.
Two Specific Nose Cell Types have been identified as likely Initial Infection Points for COVID-19 coronavirus. We found that the receptor protein -- ACE2 -- and the TMPRSS2 protease that can activate SARS-CoV-2 entry are expressed in cells in different organs, including the cells on the inner lining of the nose. We then revealed that mucus-producing goblet cells and ciliated cells in the nose had the highest levels of both these COVID-19 virus proteins, of all cells in the airways. This makes these cells the most likely initial infection route for the virus. The two key entry proteins ACE2 and TMPRSS2 were also found in cells in the cornea of the eye and in the lining of the intestine. This suggests another possible route of infection via the eye and tear ducts, and also revealed a potential for fecal-oral transmission.
Say it, Don't Spray it! How much we spit when talking? During human expiratory activities such as talking, laughing, coughing and sneezing, many droplets of saliva and other secretions are expelled from the respiratory tract (the mouth and nose). Larger droplets may rapidly settle out of the air and thus contribute to disease transmission to individuals in close proximity; smaller droplets may remain suspended for a long time and contribute to disease transmission over larger distances. Their sizes predominately determine the times they can remain airborne and thus the possibility of spread of infectious diseases if these respiratory droplets contain infectious pathogens. Moreover, the size distribution of such droplets influences the type of microorganisms that may be carried as well as the strategies for controlling the infections.
I don't judge people who wear a mask or who don't wear a mask. Everyone has personal reasons. I wear a mask mostly out of respect for other people, and not just for myself. Wearing a mask is just one decision of many decisions that I will make today. I wear a mask when the risk is high or when the vulnerability is high. But sometimes I am temporarily incoherent when I make a spontaneous decision. I'm not claiming insanity or claiming to be a victim of a calamity, it's just a random choice of circumstance. I'm not saying that it's right or wrong, because it's not a carefully decided choice, it is what it is. I will debate it if necessary, but we only have so much time, but I'm willing if you are, just as long as it's relative to our situation. Discrimination - Assumptions.
Hospital Infections
There were approximately 721,800 infections in 648,000 patients of 183 hospitals in 10 states in a 2011 survey. In that year alone, around 75,000 of these patients died that year as a result of a health care-associated infection. Hospital infections cost the U.S. 9.8 billion each year. Superbugs are on the rise. Hospitals are gaming a system by failing to report patient-infection rates and, in turn, the facilities can see a bonus or a penalty worth millions of dollars. The bonuses and penalties are part of Medicare's Inpatient Quality Reporting program, which is meant to reward hospitals for low infection rates and give consumers access to the information at the agency's Hospital Compare website.
Contagious Transmissible - What is an Infection - Super Bugs - Antimicrobial Materials - Disease - Microbiota
Hospital-Acquired Infection or nosocomial infection is an infection that is acquired in a hospital or other health care facility. To emphasize both hospital and nonhospital settings, it is sometimes instead called a healthcare–associated infection (HAI or HCAI). Such an infection can be acquired in hospital, nursing home, rehabilitation facility, outpatient clinic, diagnostic laboratory or other clinical settings. Infection is spread to the susceptible patient in the clinical setting by various means. Health care staff also spread infection, in addition to contaminated equipment, bed linens, or air droplets. The infection can originate from the outside environment, another infected patient, staff that may be infected, or in some cases, the source of the infection cannot be determined. In some cases the microorganism originates from the patient's own skin microbiota, becoming opportunistic after surgery or other procedures that compromise the protective skin barrier. Though the patient may have contracted the infection from their own skin, the infection is still considered nosocomial since it develops in the health care setting. In the United States, the Centers for Disease d fungi combined, cause or contribute to 99,000 deaths each year. In Europe, where hospital surveys have been conducted, the category of gram-negative infections are estimated to account for two-thirds of the 25,000 deaths each year. Nosocomial infections can cause severe pneumonia and infections of the urinary tract, bloodstream and other parts of the body. Many types display antimicrobial resistance, which can complicate treatment.
Antimicrobial Resistance is the ability of a microbe to resist the effects of medication previously used to treat them. This broader term also covers antibiotic resistance, which applies to bacteria and antibiotics. Resistance arises through one of three ways: natural resistance in certain types of bacteria; genetic mutation; or by one species acquiring resistance from another. Resistance can appear spontaneously because of random mutations; or more commonly following gradual buildup over time, and because of misuse of antibiotics or antimicrobials. Resistant microbes are increasingly difficult to treat, requiring alternative medications or higher doses—which may be more costly or more toxic. Microbes resistant to multiple antimicrobials are called multidrug resistant (MDR); or sometimes superbugs. Antimicrobial resistance is on the rise with millions of deaths every year. A few infections are now completely untreatable because of resistance. All classes of microbes develop resistance (fungi, antifungal resistance; viruses, antiviral resistance; protozoa, antiprotozoal resistance; bacteria, antibiotic resistance).
Humans are mostly Microbes.
How can governments fight antimicrobial resistance with policy? Described in these 69 studies were 17 different types of policies that governments have deployed and tested to reduce antimicrobial use, including public awareness campaigns, antimicrobial guidelines, vaccination, and tailored regulations for prescribing and reimbursement. Unfortunately, most existing policy options have not been rigorously evaluated, which limits their usefulness in planning future policy interventions. Of the studies, only 4 had a randomized controlled design, the gold standard for medical interventions, while 35 used rigorous quasi-experimental designs and the remaining 30 were uncontrolled and descriptive. The current systematic review was unable to directly investigate the impact of the different interventions on AMR, but reductions in antimicrobial use are likely to lead to lower levels of resistance over time.
Antifungal Resistance Threat. Without immediate action, humanity will potentially face further escalation in resistance in fungal disease, a group of scientists from the around the world has warned. According to the scientists most fungal pathogens identified by the World Health Organization -- accounting for around 3.8 million deaths a year -- are either already resistant or rapidly acquiring resistance to antifungal drugs.
Molecular basis of major Antibiotic Resistance transfer mechanism unraveled. The research team discovered that the workhorse of the transposon insertion machine, the transposase protein, has an unusual shape. This enables it to bind to the DNA in an inactive state, which prevents cleavage and thus destruction of the transposon until it can paste the antibiotic resistance gene in the new host genome. The protein's special shape also forces the transposon DNA to unwind and open up, allowing it to insert its antibiotic resistance cargo at many places in an extremely diverse range of bacteria.
Multi-Drug Resistant Bacteria - Fecal Transplants
Antimicrobial Properties of Copper and its alloys (brasses, bronzes, cupronickel, copper-nickel-zinc, and others) are natural antimicrobial materials.
Infection outbreaks at Hospitals could be reduced by Copper-Coated Uniforms. Uniforms brushed with tiny copper nanoparticles to reduce the spread of bacterial infections and viruses.
Ultra-Thin Plastic film coating kills viruses on nanotextured surfaces by literally pulling viruses apart on contact. A new virus-fighting plastic film could transform everyday surfaces into invisible defenders against disease. Instead of relying on chemicals, this flexible material is covered in microscopic pillars that physically stretch viruses until they burst, rendering them harmless. In lab tests, it destroyed or disabled about 94% of virus particles within an hour, showing impressive effectiveness.
Graphene kills harmful bacteria “superbugs” but spares human cells. Scientists have uncovered how graphene oxide pulls off a remarkable trick: it hunts down and destroys harmful bacteria while leaving human cells completely unharmed. By targeting a molecule found only in bacterial membranes, this ultra-thin carbon-based material acts with laser-like precision—offering a powerful new alternative to traditional antibiotics. Even more exciting, it works against drug-resistant “superbugs,” promotes faster wound healing, and keeps its antibacterial strength even after repeated washing. This discovery points to a new class of antibacterial materials that could be both safe for people and capable of reducing reliance on traditional antibiotics.
Durable, washable textile coating can repel viruses. New research could lead to safely reusable PPE. Researchers have created a textile coating that can not only repel liquids like blood and saliva but can also prevent viruses from adhering to the surface.
Smartphone Screen Technology used to trick Harmful Bacteria. Conducting plastics found in smartphone screens can be used to trick the metabolism of pathogenic bacteria by adding or removing electrons from the plastic surface, bacteria may be tricked into growing more or less.
Antimicrobial is an agent that kills microorganisms or stops their growth. Antimicrobial medicines can be grouped according to the microorganisms they act primarily against. For example, antibiotics are used against bacteria and antifungals are used against fungi. They can also be classified according to their function. Agents that kill microbes are called microbicidal, while those that merely inhibit their growth are called biostatic. The use of antimicrobial medicines to treat infection is known as antimicrobial chemotherapy, while the use of antimicrobial medicines to prevent infection is known as antimicrobial prophylaxis, which refers to the prevention of infection complications using antimicrobial therapy (most commonly antibiotics).
Antibiotics (drugs) - Air Purification - Hand Washing
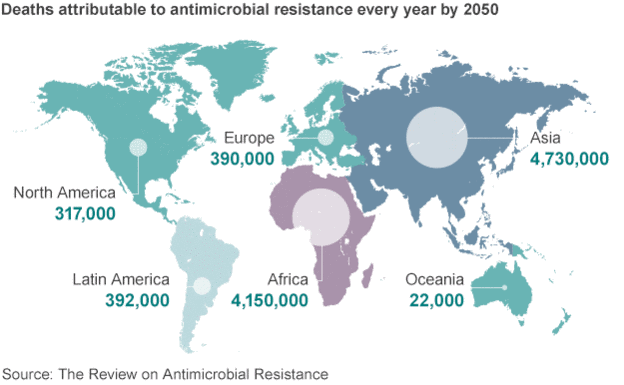 Oligodynamic effect is a biocidal effect of metals, especially heavy
metals, that occurs even in low concentrations.
Oligodynamic effect is a biocidal effect of metals, especially heavy
metals, that occurs even in low concentrations. Biocide is a chemical substance or microorganism intended to destroy, deter, render harmless, or exert a controlling effect on any harmful organism by chemical or biological means.
Disinfectant are antimicrobial agents that are applied to the surface of non-living objects to destroy microorganisms that are living on the objects.
Hospital workers often transfer germs when removing gloves and gowns.
Hand Washing Tips
Doctors should also wipe their stethoscopes between patients
Choosing a Hospital and Surgeon with Low Infections Rates.
Bacterial infections are still killing about 700,000 people each year.
Efflux in microbiology is a mechanism responsible for moving compounds, like neurotransmitters, toxic substances, and antibiotics, out of the cell; this is considered to be a vital part of xenobiotic metabolism. This mechanism is important in medicine as it can contribute to bacterial antibiotic resistance. Efflux systems function via an energy-dependent mechanism (active transport) to pump out unwanted toxic substances through specific efflux pumps. Some efflux systems are drug-specific, whereas others may accommodate multiple drugs with small multidrug resistance (SMR) transporters.
Hospital Errors - Best Practice
Monoclonal antibody prevents malaria infection in African adults. The Phase 2 NIAID-USTTB trial evaluated the safety and efficacy of a one-time, intravenous infusion of a monoclonal antibody called CIS43LS. This antibody was previously shown to neutralize the sporozoites of P. falciparum in the skin and blood before they could infect liver cells. Antibody protected clinical trial participants during six-month malaria season. One dose of an antibody drug safely protected healthy, non-pregnant adults from malaria infection during an intense six-month malaria season in Mali, Africa, a National Institutes of Health clinical trial has found. The antibody was up to 88.2% effective at preventing infection over a 24-week period, demonstrating for the first time that a monoclonal antibody can prevent malaria infection in an endemic region. An estimated 241 million cases of malaria occurred worldwide in 2020, according to the World Health Organization (WHO), resulting in an estimated 627,000 deaths, mostly in children in sub-Saharan Africa. Malaria is caused by Plasmodium parasites, which are transmitted to people through the bite of an infected mosquito. The mosquito injects the parasites in a form called sporozoites into the skin and bloodstream. These travel to the liver, where they mature and multiply. Then the mature parasite spreads throughout the body via the bloodstream to cause illness. P. falciparum is the Plasmodium species most likely to result in severe malaria infections, which, if not promptly treated, may lead to death.
Viruses - Plague's and Epidemics
By masquerading as red blood cells, the Nanosponges attract harmful toxins and remove them from the bloodstream.
Olympus $40,000 gastrointestinal scopes endoscopic retrograde cholangiopancreatography. The scope’s design could allow blood and tissue to become trapped, spreading bacteria from one patient to another. Physicians perform nearly 700,000 of those procedures annually in the U.S., and 2 million worldwide.
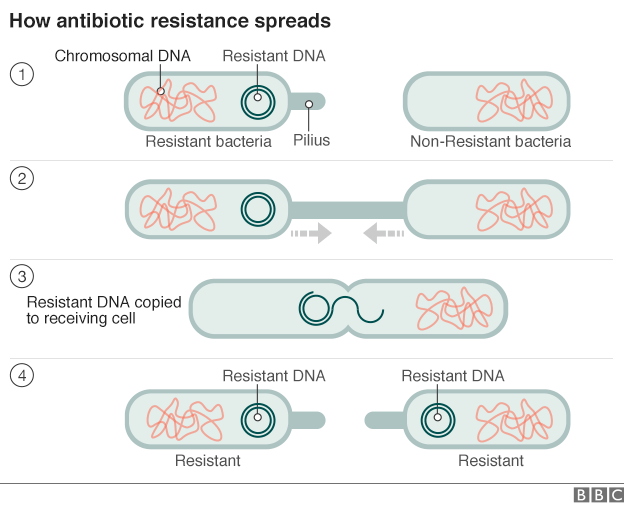 Most of these 18
bacteria, which cause about 2.3 million yearly infections in
the US, have developed
measurable resistances to many drugs within the existing
classes.
Most of these 18
bacteria, which cause about 2.3 million yearly infections in
the US, have developed
measurable resistances to many drugs within the existing
classes.
Heater-cooler devices used in cardiac surgery aerosolized the Mycobacterium chimaera into the air leading to direct contamination of the surgical wound.
Comprehensive serological profiling of human populations using a synthetic human virome
According to the Centers for Disease Control and Prevention, on any given day about 1 in 25 hospital patients has at least one healthcare-associated infection. Tens of thousands of people die each year as a result.
Research, including a 2015 investigation from Consumer Reports, found that many of these cases can be traced back to inappropriate antibiotic use, the very drugs that are supposed to fight infections. Patients on Antibiotics are more susceptible to C. diff, for example, because antibiotics kill off intestinal bacteria make sure all visitors and medical staff wash their hands before approaching you.
Bringing a canister of bleach wipes wiping down surfaces around the hospital bed can reduce the risk of some C. diff infections by as much as 85 percent.
Bathing with chlorhexidine soap, which can remove harmful bacteria you may be carrying on your skin, days before scheduled surgery.
New Disease Surveillance Tool helps Detect any Human-Infecting Virus. A new computational method called 'CATCH' designs molecular 'baits' for any virus known to infect humans and all their known strains, including those that are present in low abundance in clinical samples, such as Zika. The approach can help small sequencing centers around the globe conduct disease surveillance, which is crucial for controlling outbreaks.
Antibiotics - Antimicrobial - Resistance - Super Bugs
Antibiotic are a type of antimicrobial drug used in the treatment and prevention of bacterial infections. They may either kill or inhibit the growth of bacteria. A limited number of antibiotics also possess antiprotozoal activity. Antibiotics are not effective against viruses such as the common cold or influenza, and their inappropriate use allows the emergence of resistant organisms. Drugs which inhibit viruses are termed antiviral drugs or antivirals rather than antibiotics.
List of Antibiotics (wiki) - Ointments for Small Cuts - Honey - Phage
New class of antibiotics active against a wide range of bacteria. Dual-acting immuno-antibiotics block an essential pathway in bacteria and activate the adaptive immune response. Scientists have discovered a new class of compounds that uniquely combine direct antibiotic killing of pan drug-resistant bacterial pathogens with a simultaneous rapid immune response for combating antimicrobial resistance (AMR).
Newly engineered versions of bacterial enzyme reveal how antibiotics could be more potent. Researchers applied a new technology to generate the full inventory of mutations in the bacterial species Escherichia coli where the antibiotic rifampicin attaches to and disables an essential bacterial enzyme known as RNA polymerase (RNAP). Modern medicine depends on antibiotics to treat infections by disabling targets inside bacterial cells. Once inside these cells, antibiotics bind to certain sites on specific enzyme targets to stop bacterial growth. Randomly occurring changes (mutations) in the genes for these targets occur naturally, in some cases making the target harder for the antibiotic to attach to, and that bacterial version resistant to treatment.
Scientists find hidden antibiotic 100x stronger against deadly superbugs. A potent new antibiotic called pre-methylenomycin C lactone. The compound had been "hiding in plain sight" as an intermediate chemical in the natural process that produces the known antibiotic methylenomycin A.
New "super antibiotic" stops deadly gut infection without destroying the microbiome. A newly developed antibiotic called EVG7 could offer a powerful new way to stop Clostridioides difficile, a dangerous gut bacterium that often returns after treatment. In mouse studies, researchers found that even a very small dose of EVG7 was highly effective at clearing the infection and preventing it from coming back. Unlike many current antibiotics, which wipe out large portions of the gut microbiome, EVG7 appears to spare beneficial bacteria that naturally help keep C. difficile in check.
Antibiotic Resistance Genes are often located on plasmids or transposons and can be transferred from cell to cell by conjugation, transformation, or transduction. This gene exchange allows the resistance to rapidly spread throughout a population of bacteria and among different species of bacteria. ARGs are mobile genetic elements that can pass between microorganisms via horizontal gene transfer, even from dead to living cell. DNA Damage.
Scientists discover bacteria can “explode” to spread antibiotic resistance. Bacteria are hijacking their own “immune system” to burst open and share DNA—fueling the spread of antibiotic resistance. Scientists have uncovered a surprising twist in how bacteria share genes—including those that spread antibiotic resistance. Tiny virus-like particles called gene transfer agents or GTAs, once ancient viral invaders, have been repurposed by bacteria into delivery systems that shuttle DNA between neighboring cells. The study reveals a key control hub of three genes, dubbed LypABC, that triggers bacterial cells to burst open and release these DNA-packed couriers.
5,000 year old ice cave bacterium resists modern antibiotics. It’s not just a potential threat — it can also suppress dangerous “superbugs” and produces powerful enzymes that could inspire new medicines and industrial tools. The Psychrobacter SC65A.3 bacterial strain isolated from Scarisoara Ice Cave, despite its ancient origin, shows resistance to multiple modern antibiotics and carries over 100 resistance-related genes. But it can also inhibit the growth of several major antibiotic-resistant 'superbugs' and showed important enzymatic activities with important biotechnological potential.
Antimicrobial Resistance happens when germs like bacteria and fungi develop the ability to defeat the drugs designed to kill them. Antimicrobial resistance does not mean our body is resistant to antibiotics or antifungals.
Microplastics could be fueling antibiotic resistance. Researchers were shocked to see that bacteria's antimicrobial resistance is strengthened when exposed to plastic particles and point to a potential outsized impact on refugees. The plastics provide a surface that the bacteria attach to and colonize. It's estimated that there are 4.95 million deaths associated with antimicrobial-resistant infections each year.
Sugar molecule called pseudaminic acid could defeat deadly superbugs. By designing antibodies that recognize this unique sugar, researchers were able to guide the immune system to attack and eliminate deadly infections that normally shrug off antibiotics. Although it resembles sugars found on human cells, this molecule is made only by bacteria. Many dangerous pathogens use it as a key part of their outer surface, helping them survive and evade immune defenses. The team engineered antibodies that lock onto a sugar found only on bacterial cells, an approach that could support a new generation of immunotherapies for multidrug resistant infections acquired in hospitals. This study shows what's possible when we combine chemical synthesis with biochemistry, immunology, microbiology and infection biology. By precisely building these bacterial sugars in the lab with synthetic chemistry, we were able to understand their shape at the molecular level and develop antibodies that bind them with high specificity. That opens the door to new ways of treating some devastating drug-resistant bacterial infections. Because the human body does not produce this sugar, it offers a highly specific target for developing immunotherapies that avoid harming healthy cells.
Common painkillers like Advil and Tylenol supercharge antibiotic resistance. Painkillers we often trust — ibuprofen and acetaminophen — may be quietly accelerating one of the world’s greatest health crises, antibiotic resistance. Researchers discovered that these drugs not only fuel bacterial resistance on their own but make it far worse when combined with antibiotics. The findings are especially troubling for aged care settings, where residents commonly take multiple medications, creating perfect conditions for resistant bacteria to thrive.
Antimicrobial is an agent that kills microorganisms or stops their growth. Antimicrobial medicines can be grouped according to the microorganisms they act primarily against. Antibiotics are used against bacteria, and antifungals are used against fungi. They can also be classified according to their function. Agents that kill microbes are microbicides, while those that merely inhibit their growth are called bacteriostatic agents. The use of antimicrobial medicines to treat infection is known as antimicrobial chemotherapy, while the use of antimicrobial medicines to prevent infection is known as antimicrobial prophylaxis. Hydrolytic antimicrobial enzymes function by degrading key structural components of the cell walls of bacteria and/or fungi, whereas antimicrobial oxidoreductases exert their effects by the generation in situ of reactive molecules.
Antimicrobial Resistance - Super Bugs - Human Microbes - Antibodies
Antibacterial is an agent that interferes with the growth and reproduction of bacteria. While antibiotics and antibacterials both attack bacteria, these terms have evolved over the years to mean two different things.
New model for antibacterial mechanism. Biologists have discovered an aberrant protein that's deadly to bacteria. This erroneously built protein mimics the action of aminoglycosides, a class of antibiotics. The newly discovered protein could serve as a model to help scientists unravel details of those drugs' lethal effects on bacteria -- and potentially point the way to future antibiotics.
Disinfectant - Hand Washing
Synthesised Antibiotic is Capable of Treating Superbugs. Drug version is based on teixobactin, which is a natural antibiotic discovered by US scientists in soil samples in 2015, could help in the battle against antibiotic resistant pathogens such as MRSA and VRE. Methicillin-Resistant Staphylococcus Aureus - Vancomycin-Resistant Enterococci.
Vancomycin is an antibiotic used to treat a number of bacterial infections. Vancomycin is made by the soil bacterium Amycolatopsis orientalis. Fights bacteria in three different ways.
Viruses - Infections
Synthetic compound shows promise against multidrug resistance. Researchers have synthesized a new compound called infuzide that shows activity against resistant strains of pathogens. Antimicrobial resistance directly causes more than 1 million deaths every year and contributes to more than 35 million more, according to the World Health Organization.
Pregnant women produce super antibodies to protect newborns, now scientists know how. During pregnancy, a subtle molecular change allows immunoglobulin G -- the body's most common type of antibody -- to take on an expanded protective role. Now scientists say this natural process can be replicated to improve vaccines and other antibody-based treatments.
Scientists discovered years ago that newborn infants depend upon immune components transferred from their mothers to survive the onslaught of pathogens that begin invading their bodies as soon as they are born. Eventually, children develop their own immune systems, built through surviving natural exposures to viruses and bacteria, and augmented by a phalanx of well-established childhood vaccines. But in the meantime, it's one of a mother's most important gifts that keeps their babies safe: antibodies.
8,000 New Antibiotic Combinations are surprisingly effective. Grouping 4 or 5 existing medications could help slow antibiotic-resistant bacteria.
Antimicrobial use in agriculture can breed bacteria resistant to first-line human defenses. A new study has shown that overuse of antimicrobials in livestock production can drive the evolution of bacteria more resistant to the first line of the human immune response. Bacteria that had evolved resistance to colistin, an antimicrobial widely used in farming, also showed resistance to compounds that are key components of human and animal immune systems. The results indicate that farmed pigs and chickens could harbour large reservoirs of cross-resistant bacteria, capable of fuelling future epidemics. Drug-resistant infections are one of the most serious threats to global health, and there is an urgent need to develop new, effective antimicrobials. One promising solution could be antimicrobial peptides or AMPs. These are compounds naturally produced by most living organisms, including animals, and have important roles in innate immunity, our first line of defense against bacterial infections.
Testing antibiotic resistance with a fast, cheap, and easy method. Researchers have developed a novel and highly efficient method for rapid antibiotic susceptibility testing using optical microscopy. The technique, called Optical Nanomotion Detection, is extremely rapid, single-cell sensitive, label-free, and requires only a basic traditional optical microscope, equipped with a camera or a mobile phone. Antibiotic sensitivity testing (AST) uses culture methods that expose bacteria to antibiotics, or genetic methods to determine if bacteria possesses genes that confer resistance. We have developed a technique in our laboratories that allows us to obtain an antibiogram within 2-4 hours -- instead of the current 24 hours for the most common germs and one month for tuberculosis. The new technique is called optical nanomotion detection (ONMD), and involves the monitoring of nanoscale vibrations of single bacterial before and while being exposed to antibiotics. The monitoring is performed with a basic optical microscope, a video camera or a mobile phone.
New vaccine concept tackles harmful bacteria in the intestine. In the fight against bacterial pathogens, researchers are combining vaccination with targeted colonization of the intestine by harmless microorganisms. This approach could potentially mark a turning point in the antibiotics crisis. Although we can decimate pathogenic bacteria with a vaccine, we need harmless microorganisms to fill the resulting niche in the intestinal ecosystem in order to achieve long-term success.
Artificial Cells are Tiny Bacteria Fighters. Artificial cells mimic the essential features of live cells, but are short-lived and cannot divide to reproduce themselves. The cells were designed to respond to a unique chemical signature on E. coli bacteria. They were able to detect, attack and destroy the bacteria in laboratory experiments.
 Bacteriophage is
a virus that infects and replicates within bacteria and archaea.
Bacteriophages are composed of proteins that encapsulate a DNA or RNA
genome, and may have structures that are either simple or elaborate. Their
genomes may encode as few as four genes and as many as hundreds of genes.
Phage is a virus that is parasitic and
reproduces itself in bacteria.
Phages replicate within the
bacterium
following the injection of their genome into its cytoplasm. Bacteriophages
are among the most common and diverse entities in the biosphere.
Bacteriophages are ubiquitous viruses, found wherever bacteria exist. It
is estimated there are more than 10*31 bacteriophages on the planet, more
than every other organism on Earth, including bacteria, combined. One of
the densest natural sources for phages and other viruses is seawater,
where up to 9x108 virions per millilitre have been found in microbial mats
at the surface, and up to 70% of marine bacteria may be infected by
phages. Phages have been used for more than 90 years as an alternative to
antibiotics in the former Soviet Union and Central Europe, as well as in
France. They are seen as a possible therapy against multi-drug-resistant
strains of many bacteria (see phage therapy). Phages of Inoviridae have
been shown to complicate biofilms involved in pneumonia and cystic
fibrosis and to shelter the bacteria from drugs meant to eradicate
disease, thus promoting persistent infection.
Bacteriophage is
a virus that infects and replicates within bacteria and archaea.
Bacteriophages are composed of proteins that encapsulate a DNA or RNA
genome, and may have structures that are either simple or elaborate. Their
genomes may encode as few as four genes and as many as hundreds of genes.
Phage is a virus that is parasitic and
reproduces itself in bacteria.
Phages replicate within the
bacterium
following the injection of their genome into its cytoplasm. Bacteriophages
are among the most common and diverse entities in the biosphere.
Bacteriophages are ubiquitous viruses, found wherever bacteria exist. It
is estimated there are more than 10*31 bacteriophages on the planet, more
than every other organism on Earth, including bacteria, combined. One of
the densest natural sources for phages and other viruses is seawater,
where up to 9x108 virions per millilitre have been found in microbial mats
at the surface, and up to 70% of marine bacteria may be infected by
phages. Phages have been used for more than 90 years as an alternative to
antibiotics in the former Soviet Union and Central Europe, as well as in
France. They are seen as a possible therapy against multi-drug-resistant
strains of many bacteria (see phage therapy). Phages of Inoviridae have
been shown to complicate biofilms involved in pneumonia and cystic
fibrosis and to shelter the bacteria from drugs meant to eradicate
disease, thus promoting persistent infection. Phage Therapy is the therapeutic use of bacteriophages to treat pathogenic bacterial infections. Phage therapy has many potential applications in human medicine as well as dentistry, veterinary science, and agriculture. If the target host of a phage therapy treatment is not an animal, the term "biocontrol" (as in phage-mediated biocontrol of bacteria) is usually employed, rather than "phage therapy". Bacteriophages are much more specific than antibiotics. They are typically harmless not only to the host organism, but also to other beneficial bacteria, such as the gut flora, reducing the chances of opportunistic infections. They have a high therapeutic index, that is, phage therapy would be expected to give rise to few side effects. Because phages replicate in vivo, a smaller effective dose can be used. On the other hand, this specificity is also a disadvantage: a phage will only kill a bacterium if it is a match to the specific strain. Consequently, phage mixtures are often applied to improve the chances of success, or samples can be taken and an appropriate phage identified and grown. Phages tend to be more successful than antibiotics where there is a biofilm covered by a polysaccharide layer, which antibiotics typically cannot penetrate. In the West, no therapies are currently authorized for use on humans, although phages for killing food poisoning bacteria (Listeria) are now in use. Phages are currently being used therapeutically to treat bacterial infections that do not respond to conventional antibiotics, particularly in Russia and Georgia. There is also a phage therapy unit in Wrocław, Poland, established 2005, the only such centre in a European Union country. Antibiotics were pushed more than Phage therapy because of corporate monopolies at peoples expense.
Autophagy is a cellular process that degrades and recycles damaged or unnecessary components like proteins and organelles, acting as a "self-eating" mechanism to maintain cellular health and homeostasis. Cold Shower.
Macrophage are a type of white blood cell, of the immune system, that engulfs and digests cellular debris, foreign substances, microbes, cancer cells, and anything else that does not have the type of proteins specific to healthy body cells on its surface in a process called phagocytosis. These large phagocytes are found in essentially all tissues, where they patrol for potential pathogens by amoeboid movement.
Peering into the secrets of phages to see how they kill bacterial superbugs. We saw how the building blocks of the particle interlock in an intricate choreography. At a molecular level, arms swing out and curl around each other forming a continuous chain that braces the head of the phage. This rigid chainmail provides further protection to the DNA of the phage. Surprisingly, the tail on the other hand remains flexible. It's able to bend and not break as it captures the bacteria and ultimately injects them with the phage DNA. Phages are a class of viruses that infect bacteria, and each phage is specific for the species of bacteria it can kill. Phages can be purified to a point of being FDA-approved for treatment of people with bacterial infections, and documented success has been had in the USA, Europe and, recently, Australia.
A new multipurpose on-off switch for inhibiting bacterial growth. Researchers have discovered an antitoxin mechanism that seems to be able to neutralize hundreds of different toxins and may protect bacteria against virus attacks. The mechanism has been named Panacea, after the Greek goddess of medicine whose name has become synonymous with universal cure. The understanding of bacterial toxin and antitoxin mechanisms will be crucial for the future success of so-called phage therapy for the treatment of antibiotic resistance infections, the researchers say.
New research moves closer to harnessing viruses to fight bacteria and reduce antibiotic use. A new study has cast new light on how to best combine antibiotics and phage therapy. Researchers conducted laboratory experiments on Pseudomonas aeruginosa a bacterium which causes disease in immunocompromised and cystic fibrosis patients. They exposed the bacterium to eight types of antibiotics -- and found differences in the mechanisms by which the bacteria evolve resistance to phages, which affect how harmful they are.
Linezolid is an antibiotic used for the treatment of infections caused by Gram-positive bacteria that are resistant to other antibiotics.
Daptomycin is a lipopeptide antibiotic used in the treatment of systemic and life-threatening infections caused by Gram-positive organisms.
Immune System
Antimicrobial Resistance is the ability of a microbe to resist the effects of medication previously used to treat them.
Timing is key for bacteria surviving antibiotics. Researchers found that cells that repaired DNA damaged by antibiotics before resuming growth had a much better chance of surviving treatment.
Carbapenem resistant enterobacteriaceae are Gram-negative bacteria that are resistant to the carbapenem class of antibiotics, considered the drugs of last resort for such infections.
Klebsiella pneumoniae is a Gram-negative, nonmotile, encapsulated, lactose-fermenting, facultative anaerobic, rod-shaped bacterium. It appears as a mucoid lactose fermenter on MacConkey agar.
New Delhi metallo-beta-lactamase 1 is an enzyme that makes bacteria resistant to a broad range of beta-lactam antibiotics. These include the antibiotics of the carbapenem family, which are a mainstay for the treatment of antibiotic-resistant bacterial infections.
Maryn Mckenna what do we do when antibiotics don't work any more? (video and interactive text)
Using rank order to identify complex genetic interactions. Ranking pathogen mutants can help scientists understand how mutants evolve to resist drug treatments.
 Nudging Guideline-Concordant Antibiotic
Prescribing
Nudging Guideline-Concordant Antibiotic
PrescribingNudging physician prescription decisions by partitioning the order set: results of a vignette-based study.
Effect of Behavioral Interventions on Inappropriate Antibiotic Prescribing Among Primary Care Practices.
Supercharged Antibiotics could turn tide against Superbugs by modifying vancomycin’s membrane-binding properties to selectively bind to bacterial membranes rather than those of human cells, creating a series of supercharged vancomycin derivatives called vancapticins. Antibiotic-resistant bacteria – Superbugs cause 700,000 deaths worldwide each year, and a UK government review has predicted this could rise to 10 million by 2050.
Strontium Titanate is an oxide of strontium and titanium with the chemical formula SrTiO3. (neodymium titanate).
A new group of antibiotics with a unique approach to attacking bacteria has been discovered. The newly-found corbomycin and the lesser-known complestatin have a never-before-seen way to kill bacteria, which is achieved by blocking the function of the bacterial cell wall. The discovery comes from a family of antibiotics called glycopeptides that are produced by soil bacteria. The researchers also demonstrated in mice that these new antibiotics can block infections caused by the drug resistant Staphylococcus aureus which is a group of bacteria that can cause many serious infections. Antibiotics like penicillin kill bacteria by preventing building of the wall, but the antibiotics that we found actually work by doing the opposite -- they prevent the wall from being broken down. This is critical for cell to divide. In order for a cell to grow, it has to divide and expand. If you completely block the breakdown of the wall, it is like it is trapped in a prison, and can't expand or grow.
Antibiotic consumption is currently not the main driver of aminoglycoside resistance spread, study suggests. Drug resistance to aminoglycosides, a class of antibiotics, may be driven more by exchanges between ecosystems than by drug consumption. The spread of antibiotic resistance, where infectious bacteria are able to defeat the drugs intended to kill them, may not be primarily driven by antibiotic consumption, according to a new study.
New antibiotic cures superbugs without bacterial resistance. In a potential game changer for the treatment of superbugs, a new class of antibiotics was developed that cured mice infected with bacteria deemed nearly 'untreatable' in humans -- and resistance to the drug was virtually undetectable.
M Protein in Streptococcus is a virulence factor that can be produced by certain species of Streptococcus. Viruses, parasites and bacteria are covered in protein and sugar molecules that help them gain entry into a host by counteracting the host's defences. One such molecule is the M protein produced by certain streptococcal bacteria. M proteins embody a motif that is now known to be shared by many Gram-positive bacterial surface proteins. The motif includes a conserved pentapeptide LPXTG, which precedes a hydrophobic C-terminal membrane anchor, which itself precedes a cluster of basic residues. Strep's M protein alone wipes out macrophages, but not other types of immune cells. The macrophages' self-sacrifice serves as an early warning of infection to the rest of the immune system. White Blood Cells.
Neurodegeneration is the progressive loss of structure or function of neurons, including death of neurons. (Ly6Chi cells).
Antibodies linked to heart attacks. Levels of antiphospholipid antibodies, which are associated with rheumatic diseases, are also elevated in myocardial infarction without any autoimmune co-morbidity.
Antiphospholipid Syndrome is an autoimmune, hypercoagulable state caused by antiphospholipid antibodies. APS provokes blood clots (thrombosis) in both arteries and veins as well as pregnancy-related complications such as miscarriage, stillbirth, preterm delivery, and severe preeclampsia.Antiphospholipid syndrome can be primary or secondary. Primary antiphospholipid syndrome occurs in the absence of any other related disease. Secondary antiphospholipid syndrome occurs with other autoimmune diseases, such as systemic lupus erythematosus (SLE). In rare cases, APS leads to rapid organ failure due to generalised thrombosis; this is termed "catastrophic antiphospholipid syndrome" (CAPS or Asherson syndrome) and is associated with a high risk of death. Body Burden.
Frequent use of antimicrobial drugs in early life shifts bacterial profiles in saliva. The strongest associations were presented with azithromycin that is used for example to middle ear infections, strep throat and pneumonia. The human microbiota plays an important role in health and well-being by assisting in digestion, producing nutrients, resisting invading pathogens and regulating metabolism and the immune system. We use antimicrobial (AM) drugs to treat common infections even though they have an immediate effect on microbial diversity and composition.
Antibiotics that kill gut bacteria also stop growth of new brain cells. A type of white blood cell seems to act as a communicator between the brain, the immune system, and the gut.
Resistance to Antibiotics - Super Bugs
Super Bugs or antimicrobial resistance, is the ability of a microbe to resist the effects of medication that once could successfully treat the microbe. The term antibiotic resistance (AR or ABR) is a subset of AMR, as it applies only to bacteria becoming resistant to antibiotics. Resistant microbes are more difficult to treat, requiring alternative medications or higher doses of antimicrobials. These approaches may be more expensive, more toxic or both. Microbes resistant to multiple antimicrobials are called multidrug resistant (MDR). Those considered extensively drug resistant (XDR) or totally drug resistant (TDR) are sometimes called "superbugs". Resistance arises through one of three mechanisms: natural resistance in certain types of bacteria, genetic mutation, or by one species acquiring resistance from another. All classes of microbes can develop resistance. Fungi develop antifungal resistance. Viruses develop antiviral resistance. Protozoa develop antiprotozoal resistance, and bacteria develop antibiotic resistance. Resistance can appear spontaneously because of random mutations. However, extended use of antimicrobials appears to encourage mutations which can render antimicrobials ineffective. Preventive measures include only using antibiotics when needed, thereby stopping misuse of antibiotics or antimicrobials. Narrow-spectrum antibiotics are preferred over broad-spectrum antibiotics when possible, as effectively and accurately targeting specific organisms is less likely to cause resistance. For people who take these medications at home, education about proper use is essential. Health care providers can minimize spread of resistant infections by use of proper sanitation and hygiene, including hand washing and disinfecting between patients, and should encourage the same of the patient, visitors, and family members. Rising drug resistance is caused mainly by use of antimicrobials in humans and other animals, and spread of resistant strains between the two. Growing resistance has also been linked to dumping of inadequately treated effluents from the pharmaceutical industry, especially in countries where bulk drugs are manufactured. Antibiotics increase selective pressure in bacterial populations, causing vulnerable bacteria to die; this increases the percentage of resistant bacteria which continue growing. Even at very low levels of antibiotic, resistant bacteria can have a growth advantage and grow faster than vulnerable bacteria. With resistance to antibiotics becoming more common there is greater need for alternative treatments. Calls for new antibiotic therapies have been issued, but new drug development is becoming rarer. Antimicrobial resistance is increasing globally because of greater access to antibiotic drugs in developing countries. Estimates are that 700,000 to several million deaths result per year. Each year in the United States, at least 2 million people become infected with bacteria that are resistant to antibiotics and at least 23,000 people die as a result. There are public calls for global collective action to address the threat that include proposals for international treaties on antimicrobial resistance. Worldwide antibiotic resistance is not completely identified, but poorer countries with weaker healthcare systems are more affected. Bacteria Resistant to Antibiotics.
Drug-Resistant Bacteria — also known as superbugs — are on the rise globally, and they're now killing more people each year than either HIV/AIDS or malaria. In 2019 drug resistant infections directly killed 1.2 million people and played a role in 5 million more deaths worldwide. Deadly new strains of bacteria are causing untreatable blood infections, fatal pneumonia, relentless urinary tract infections, gangrenous wounds and terminal cases of sepsis, among other conditions. Antibiotic resistance are the highest in sub-Saharan Africa, causing 24 deaths per 100,000 population compared to an average fatality rate of 13 per 100,000 in high income countries. Australia has the lowest mortality rate globally from antibiotic resistance at 6 deaths per 100,000.antibiotics are often readily available to anyone without a prescription. Misuse and overuse of these fuels mutations in bacteria, leading to more resistance. The systems to flag and test for potentially drug resistant infections are not as robust as in some wealthier countries. While some new more powerful antibiotics are being developed, lower-income countries are still dependent on older, cheaper, less effective drugs. There was a lot of antibiotic use during the pandemic. More than 70, 80% of [COVID] patients that arrived to the hospital were already using antibiotics at home. But antibiotics target bacteria and wouldn't be of much help against a coronavirus.
Superbug impact on the Gut. Bacterial superbug Clostridioides difficile hijacks the human wound healing system in order to cause serious and persistent disease, opening up the development of new therapies to treat the disease.
Antibiotics Resistance: researchers succeed to block genes of resistance. One of the ways antibiotic resistance genes spread in hospitals and in the environment is that the genes are coded on plasmids that transfer between bacteria. A plasmid is a DNA fragment found in bacteria or yeasts. It carries genes useful for bacteria, especially when these genes encode proteins that can make bacteria resistant to antibiotics researchers screened a library of small chemical molecules for those that bind to the TraE protein, an essential component of the plasmid transfer machinery. Analysis by X-ray crystallography revealed the exact binding site of these molecules on TraE. Having precise information on the binding site enabled the researchers to design more potent binding molecules that, in the end, reduced the transfer of antibiotic-resistant, gene-carrying plasmids.
Germs with unusual Antibiotic Resistance widespread in U.S. More than 23,000 Americans die each year from infections caused by germs resistant to antibiotics.
Answer to Bacterial Antibiotic Resistance may be found in Plants. Plant secondary metabolites (PSMs). PSMs are highly diverse, with more than 12,000 alkaloids, 8,000 phenolic compounds, and 25,000 terpenoids currently known.
Polyamine both inhibits the MRSA superbug and renders it more vulnerable to antibiotics.
Antibiotic Resistance in Food Animals nearly tripled since 2000. Meat production accounts for 73% of global antibiotic use. Between 2000 and 2018, the proportion of antibiotics showing rates of resistance above 50% in developing countries increased in chickens from 0.15 to 0.41 and in pigs from 0.13 to 0.34, the researchers reported. This means that antibiotics that could be used for treatment failed more than half the time in 40 percent of chickens and one-third of pigs raised for human consumption.
Infectious Bacteria Hibernate to Evade Antibiotics, instead of developing antibiotic resistant variants, an enzyme in dormant bacteria is responsible for catalyzing hibernation, which allows the bacteria to avoid being attacked. Antibiotics usually target a bacteria cell's ability to grow, which means that a hibernating bacterium is exempt from attack.
Research advances knowledge of the battle between viruses and human cells. Discovery of protective RNA mechanism informs pursuit to develop anti-viral drugs. n the long-term battle between a herpesvirus and its human host, a virologist and her team of students have identified some human RNA able to resist the viral takeover -- and the mechanism by which that occurs. Kaposi sarcoma-associated herpesvirus (KSHV) hides for years inside the human body before seeking to gain control over human gene expression to complete the viral infection. At that point, people with a weakened immune system may develop Kaposi sarcoma cancer lesions in the mouth, skin or other organs. We show that RNA that escape have a chemical tag on them -- a post-transcriptional modification -- that makes them different from the others. By having this tag, M6A, they can recruit proteins that protect them from degradation.
Chromosome architecture constrains horizontal gene transfer in bacteria, may be the key for holding the line against the global threat of increasing antibiotic resistance.
Superbugs jumping frequently between Humans and Animals. In a recent study, researchers found that cows are a source of resistant staphylococcus strains causing infections in humans today.
Antimicrobial resistance is drastically rising. Researchers have shown that antimicrobial-resistant infections are rapidly increasing in animals in low and middle income countries. They produced the first global of resistance rates, and identified regions where interventions are urgently needed.
Cause of antibiotic resistance identified. Bacteria can lose its cell wall—the common target of many groups of antibiotics. Bacteria are able to change from a highly regular walled form to a completely random, cell wall-deficient L-form state- in effect, shedding the yellow jacket and hiding it inside themselves. In this form the body can't easily recognize the bacteria so doesn't attack them—and neither do antibiotics. L-form Bacteria are strains of bacteria that lack cell walls.
Low Antibiotic Concentration in the Environment enough to increase Antimicrobial Resistance in Laboratory Conditions.
Deadly 'Superbugs' Destroyed by Molecular Drills. Motorized molecules activated by light target and drill through highly antibiotic resistant bacteria and kill them within minutes. The molecules can open bacteria to attack by drugs they previously resisted. The strategy could be applied to bacterial infections or diseases on the skin, in the lungs or in the gastrointestinal tract.
Signs of Bacteria already in the Bovine Fetus.
Physicists pinpoint a simple mechanism that makes bacteria resistant to antibiotics. Researchers examined how the membranes of bacteria interacted with the antibiotic polymyxin B (PmB), which is commonly used to treat urinary tract infections, meningitis, blood and eye infections.
Methicillin-Resistant Staphylococcus Aureus refers to a group of gram-positive bacteria that are genetically distinct from other strains of Staphylococcus aureus. MRSA is responsible for several difficult-to-treat infections in humans. MRSA is any strain of S. aureus that has developed, through horizontal gene transfer and natural selection, multiple drug resistance to beta-lactam antibiotics. β-lactam antibiotics are a broad spectrum group which includes some penams – penicillin derivatives such as methicillin and oxacillin, and cephems such as the cephalosporins. Strains unable to resist these antibiotics are classified as methicillin-susceptible S. aureus, or MSSA. MRSA is common in hospitals, prisons, and nursing homes, where people with open wounds, invasive devices such as catheters, and weakened immune systems are at greater risk of hospital-acquired infection. MRSA began as a hospital-acquired infection, but has become community-acquired as well as livestock-acquired. The terms HA-MRSA (healthcare-associated or hospital-acquired MRSA), CA-MRSA (community-associated MRSA) and LA-MRSA (livestock-associated) reflect this. Staphylococcus Aureus is a Gram-positive, round-shaped bacterium that is a member of the Firmicutes, and it is a usual member of the microbiota of the body, frequently found in the upper respiratory tract and on the skin. Gram-Positive Bacteria are bacteria that give a positive result in the Gram stain test, which is traditionally used to quickly classify bacteria into two broad categories according to their cell wall. Gram Stain is a method of staining used to distinguish and classify bacterial species into two large groups (Gram-positive and Gram-negative, which are bacteria that do not retain the crystal violet stain used in the gram-staining method of bacterial differentiation. Gram-negative bacteria are found everywhere, in virtually all environments on Earth that support life.
Atomic structure of a staphylococcal bacteriophage using cryo-electron microscopy. Cryo-electron microscopy has exposed the structure of a bacterial virus with unprecedented detail. This is the first structure of a virus able to infect Staphylococcus epidermidis, and high-resolution knowledge of structure is a key link between viral biology and potential therapeutic use of the virus to quell bacterial infections.
Vancomycin-Resistant Enterococcus are bacterial strains of the genus Enterococcus that are resistant to the antibiotic vancomycin.
Antimicrobial Chemical Triclosan tied to antibiotic resistance genes in dust and linked to changes in its genetic makeup. The result is dust with organisms that could cause an antibiotic-resistant infection.
Triclosan is an antibacterial and antifungal agent present in some consumer products, including toothpaste, soaps, detergents, toys, and surgical cleaning treatments. It is similar in its uses and mechanism of action to triclocarban. Its efficacy as an antimicrobial agent, the risk of antimicrobial resistance, and its possible role in disrupted hormonal development remains controversial. Additional research seeks to understand its potential effects on organisms and environmental health. Triclosan was developed in the 1960s. In September 2016, the FDA announced that effective September 2017, it would prohibit the sale of "consumer antiseptic washes" containing triclosan or 18 other ingredients marketed as antimicrobials due to FDA findings of the lack of efficacy in these products.
Plant Secondary Metabolism produces a large number of specialized compounds (estimated 200,000) that do not aid in the growth and development of plants but are required for the plant to survive in its environment. Secondary metabolism is connected to primary metabolism by using building blocks and biosynthetic enzymes derived from primary metabolism. Primary metabolism governs all basic physiological processes that allow a plant to grow and set seeds, by translating the genetic code into proteins, carbohydrates, and amino acids. Specialized compounds from secondary metabolism are essential for communicating with other organisms in mutualistic (e.g. attraction of beneficial organisms such as pollinators) or antagonistic interactions (e.g. deterrent against herbivores and pathogens). They further assist in coping with abiotic stress such as increased UV-radiation. The broad functional spectrum of specialized metabolism is still not fully understood. In any case, a good balance between products of primary and secondary metabolism is best for a plant’s optimal growth and development as well as for its effective coping with often changing environmental conditions. Well known specialized compounds include alkaloids, polyphenols including flavonoids, and terpenoids. Humans use quite a lot of these compounds, or the plants from which they originate, for medicinal and nutraceutical purposes.
Chaos-inducing genetic approach stymies antibiotic-resistant superbugs. A genetic disruption strategy developed by University of Colorado Boulder researchers effectively stymies the evolution of antibiotic-resistant bacteria such as E. coli, giving scientists a crucial leg up in the ongoing battle against deadly superbugs. These multidrug-resistant pathogens -- which adapt to current antibiotics faster than new ones can be created -- infect nearly 2 million people and cause at least 23,000 deaths annually in the U.S., according to data from the Centers for Disease Control. In an effort to develop a sustainable long-term solution, CU Boulder researchers created the Controlled Hindrance of Adaptation of OrganismS (CHAOS) approach, which uses CRISPR DNA editing techniques to modify multiple gene expressions within the bacteria cells, stunting the pathogen's central processes and thwarting its ability to evolve defenses.
Biofilm comprises any syntrophic consortium of microorganisms in which cells stick to each other and often also to a surface. These adherent cells become embedded within a slimy extracellular matrix that is composed of extracellular polymeric substance. The cells within the biofilm produce the EPS components, which are typically a polymeric conglomeration of extracellular polysaccharides, proteins, lipids and DNA. Because they have three-dimensional structure and represent a community lifestyle for microorganisms, they have been metaphorically described as "cities for microbes". Biofilms may form on living or non-living surfaces and can be prevalent in natural, industrial and hospital settings. The microbial cells growing in a biofilm are physiologically distinct from planktonic cells of the same organism, which, by contrast, are single-cells that may float or swim in a liquid medium. Biofilms can form on the teeth of most animals as dental plaque, where they may cause tooth decay and gum disease. Microbes form a biofilm in response to various different factors, which may include cellular recognition of specific or non-specific attachment sites on a surface, nutritional cues, or in some cases, by exposure of planktonic cells to sub-inhibitory concentrations of antibiotics. A cell that switches to the biofilm mode of growth undergoes a phenotypic shift in behavior in which large suites of genes are differentially regulated. A biofilm may also be considered a hydrogel, which is a complex polymer that contains many times its dry weight in water. Biofilms are not just bacterial slime layers but biological systems; the bacteria organize themselves into a coordinated functional community. Biofilms can attach to a surface such as a tooth, rock, or surface, and may include a single species or a diverse group of microorganisms. The biofilm bacteria can share nutrients and are sheltered from harmful factors in the environment, such as desiccation, antibiotics, and a host body's immune system. A biofilm usually begins to form when a free-swimming bacterium attaches to a surface.
How Fatal Biofilms Form. The formation of organized communities of bacterial cells known as biofilms can be deadly during surgeries By severely curtailing the effects of antibiotics and in urinary tract infections. Researchers have just come a lot closer to understanding how these biofilms develop, and potentially how to stop them.
Dangerous bacterial biofilms have a natural enemy. Discovery could help prevent infections. Scientists have now discovered a chemical that plants produce when they're stressed prevents dangerous biofilm from forming. The breakthrough offers potential advances in healthcare as well as preventing equipment corrosion in industrial settings. You've probably seen them as the slimy layer on river rocks or the plaque on your teeth. While they're a natural part of many ecosystems, biofilms can cause big problems. In plants, this metabolite, MEcPP, plays a critical role not only in producing essential compounds but also in stress signaling. For example, when a plant is damaged in some way and too much oxygen enters its cells, it accumulates MEcPP. This molecule then triggers protective responses within the plant. The researchers discovered that this same molecule has a surprising effect on bacteria like E. coli: it disrupts biofilm development by interfering with its ability to attach to surfaces. In medical settings, biofilms grow on devices like catheters, stents, or implants, making infections harder to treat because the microbes in biofilms are highly resistant to antibiotics. In industrial contexts, they clog pipes, contaminate food processing equipment, and cause corrosion. Bacteria rely on hair-like structures called fimbriae to anchor themselves to surfaces, a critical step in biofilm initiation. Fimbriae help bacteria latch onto medical implants, pipes, or even teeth, where they secrete a protective matrix that shields them from antibiotics and cleaning agents. Without fimbriae, biofilm formation cannot begin. Through genetic screenings of more than 9,000 bacterial mutants, the research team identified a key gene called fimE, which acts as an "off switch" for fimbriae production. MEcPP enhances the activity of this gene and increases the expression of fimE. This, in turn, prevents the bacteria from producing fimbriae and forming biofilms.
How bacteria responds to threats. Researchers have discovered that bacteria can sense threats in advance through a general danger signal. Bacteria detect when nearby cells are dying and proactively form a protective biofilm. Understanding how bacteria communicate and respond to threats is crucial for combating infections.
Superbug killer: New nanotech destroys bacteria and fungal cells. Nanothin antimicrobial coating could prevent and treat potentially deadly infections. A new dual bug killer is one of the thinnest antimicrobial coatings to date. The coating works by tearing bacteria and fungal cells apart, offering a smart solution to the twin global health threats of drug-resistant bacterial and fungal infections.
Paleopharmaceuticals from Baltic amber might fight drug-resistant infections. For centuries, people in Baltic nations have used ancient amber for medicinal purposes. Even today, infants are given amber necklaces that they chew to relieve teething pain, and people put pulverized amber in elixirs and ointments for its purported beneficial properties. Now, scientists have pinpointed compounds that help explain Baltic amber's therapeutic effects and that could lead to new medicines to combat antibiotic-resistant infections. Each year in the U.S., at least 2.8 million people get antibiotic-resistant infections, leading to 35,000 deaths, according to the U.S. Centers for Disease Control and Prevention.
Colds - Flu - Viruses
 Virus is a small
infectious agent that replicates only inside the living
cells of other
organisms. Viruses can infect all
types of life forms, from animals and plants to
microorganisms, including
bacteria and archaea. A virus can not replicate on
its own, but bacteria can. Pathogen is any
disease-producing agent, especially a virus,
bacterium or other microorganism. Some viruses can play a deadly game of "hide
and seek" inside the human body by entering a state of dormancy
known as latency. These infections can last a
lifetime, with the potential to reactivate and cause disease again,
even years after the initial infection has resolved. When in a latent
state, these viruses express few or no proteins. Because viral proteins
are the primary way the immune system identifies infected cells, this lack
of expression prevents detection. Some viruses, like
HIV, integrate their own genetic material
(provirus) into the DNA of the host's immune cells. When the cell divides,
it copies the viral genes along with its own. This
hides the virus from antiretroviral therapy and immune
surveillance. Viruses can alter the expression of host genes to create a
more favorable environment for themselves. For example, some may suppress
genes that would trigger an immune response. Latent viruses can become
active again and cause disease when the host's immune system is weakened
or triggered. A virus can act like a
parasite because it relies entirely on a host cell to replicate,
lacking its own metabolic machinery. Viruses are considered obligate
intracellular parasites because they must enter a living cell to
reproduce, and they hijack the host's resources like ribosomes, enzymes,
and energy to make more virus particles. Outside of a host cell, a virus
is inert. It has no ability to generate energy or make proteins on its
own. Once inside a host cell, a virus delivers its genetic material (DNA
or RNA) and forces the cell to replicate it and produce viral proteins
using the cell's own ribosomes and other cellular machinery. The virus
depends on the host cell's metabolic and biosynthetic processes for all
stages of its life cycle, from replication to the creation of new viral
components. This parasitic nature even extends to other parasites, as some
viruses can infect and replicate within parasitic protozoa, a phenomenon
known as hyper parasitism.
Virus is a small
infectious agent that replicates only inside the living
cells of other
organisms. Viruses can infect all
types of life forms, from animals and plants to
microorganisms, including
bacteria and archaea. A virus can not replicate on
its own, but bacteria can. Pathogen is any
disease-producing agent, especially a virus,
bacterium or other microorganism. Some viruses can play a deadly game of "hide
and seek" inside the human body by entering a state of dormancy
known as latency. These infections can last a
lifetime, with the potential to reactivate and cause disease again,
even years after the initial infection has resolved. When in a latent
state, these viruses express few or no proteins. Because viral proteins
are the primary way the immune system identifies infected cells, this lack
of expression prevents detection. Some viruses, like
HIV, integrate their own genetic material
(provirus) into the DNA of the host's immune cells. When the cell divides,
it copies the viral genes along with its own. This
hides the virus from antiretroviral therapy and immune
surveillance. Viruses can alter the expression of host genes to create a
more favorable environment for themselves. For example, some may suppress
genes that would trigger an immune response. Latent viruses can become
active again and cause disease when the host's immune system is weakened
or triggered. A virus can act like a
parasite because it relies entirely on a host cell to replicate,
lacking its own metabolic machinery. Viruses are considered obligate
intracellular parasites because they must enter a living cell to
reproduce, and they hijack the host's resources like ribosomes, enzymes,
and energy to make more virus particles. Outside of a host cell, a virus
is inert. It has no ability to generate energy or make proteins on its
own. Once inside a host cell, a virus delivers its genetic material (DNA
or RNA) and forces the cell to replicate it and produce viral proteins
using the cell's own ribosomes and other cellular machinery. The virus
depends on the host cell's metabolic and biosynthetic processes for all
stages of its life cycle, from replication to the creation of new viral
components. This parasitic nature even extends to other parasites, as some
viruses can infect and replicate within parasitic protozoa, a phenomenon
known as hyper parasitism. Colds - Coughing - Sneezing - Allergies - Flu - Pneumonia - Congestion - Influenza - Bacteria - Viral Load - Interferon - Mucus - Infections - Number Needed to Treat
Colds aren't caused by a single virus. So creating a vaccine to prevent the common cold has been difficult to make, primarily because there are more than 200 different varieties of viruses that can cause colds, including adenoviruses, coronaviruses, parainfluenza, and rhinoviruses. Rhinoviruses are to blame for up to 50% of all common colds. But of these rhinoviruses, there are more than 150 strains circulating at any one time. Millions of cases of the common cold are reported across the United States each year. The Centers for Disease Control and Prevention or CDC estimates that the average adult catches at least two colds every year and that children can get up to 10. On the upside, colds are self-limiting and will go away on their own, typically within a week. Boost your body's natural resistance by eating well, getting adequate sleep, not smoking, and drinking plenty of water every day.
Rhinovirus is the most common viral infectious agent in humans and is the predominant cause of the common cold. Rhinovirus infection proliferates in temperatures of 33–35 °C (91–95 °F), the temperatures found in the nose. Rhinoviruses belong to the genus Enterovirus in the family Picornaviridae. The three species of rhinovirus (A, B, and C) include around 160 recognized types of human rhinovirus that differ according to their surface proteins or serotypes. They are lytic in nature and are among the smallest viruses, with diameters of about 30 nanometers. By comparison, other viruses, such as smallpox and vaccinia, are around ten times larger at about 300 nanometers; while flu viruses are around 80–120 nm.
Why Do Viruses Kill? - BBC - Archaea - Horizon (youtube)
Why some people get bad colds and others don’t. Scientists found that nasal cells act as a first line of defense against the common cold, working together to block rhinovirus soon after infection. A fast antiviral response can stop the virus before symptoms appear. If that response is weakened or delayed, the virus spreads and causes inflammation and breathing problems. The study highlights why the body’s reaction matters more than the virus alone.
Virology is the study of viruses – submicroscopic, parasitic particles of genetic material contained in a protein coat – and virus-like agents. It focuses on the following aspects of viruses: their structure, classification and evolution, their ways to infect and exploit host cells for reproduction, their interaction with host organism physiology and immunity, the diseases they cause, the techniques to isolate and culture them, and their use in research and therapy. Virology is considered to be a subfield of microbiology or of medicine.
Over 160,000 new viruses discovered by AI. Largest discovery of new viruses sheds light on hidden virosphere. 161,979 new RNA viruses have been discovered using a machine learning tool that researchers believe will vastly improve the mapping of life on Earth and could aid in the identification of many millions more viruses yet to be characterized.
Contagious - Wash Hands - Antimicrobial Materials - Symptoms
The Lung Microbiome, Immunity and the Pathogenesis of Chronic Lung Disease. Respiratory microbiome may influence your susceptibility to flu. Microbiome community linked to lower influenza susceptibility.
Human Virome is the collection of viruses in and on the human body. Defining the virome is thought to provide an understanding of microbes and how they affect human health and disease. Viruses in the human body infect both human cells as well as other microbes such as bacteria. Human Microbiome.
Virosphere is a list of all the known viruses. Hundreds of thousands of viruses in oceans. The oceans contain almost 200,000 different viral populations, according to the latest count.
1,445 viruses have been discovered in the most populous animals.
Thousands of unknown viruses hide in the DNA of unicellular organisms. Stowaways in the genome. Scientists have discovered over 30,000 viruses by using the high-performance computer cluster 'Leo' and sophisticated detective work. The viruses hide in the DNA of unicellular organisms. In some cases, up to 10% of microbial DNA consists of built-in viruses. LEO3 is a high performance compute cluster of the Research Area Scientific Computing at the University of Innsbruck in operation since September 2011. It consists of 1944 Intel Xeon (Gulftown) compute cores and is equipped with 24GB RAM per node, i.e., about 4TB of main memory altogether. The nodes and GPFS storage system are joined by a 40Gb/s Infiniband high speed interconnect. In addition, three of the nodes are equipped with NVidia Tesla M2090 graphics cards and 48 GB of main memory.
Biologists Discover How Viruses Hijack Cell’s Machinery - Viral Infection
A shapeshifting protein explains rabies’ deadly power. Rabies virus’s shape-shifting protein reveals how deadly viruses do so much with so little. Researchers discovered how rabies virus exerts massive control over host cells with very few genes. A key viral protein changes shape and binds RNA, allowing it to infiltrate different cellular systems. This adaptability could explain the power of other deadly viruses, including Nipah and Ebola. The breakthrough may lead to next-generation antivirals or vaccines. We discovered that one of rabies virus's key proteins, called P3-protein, gains a remarkable range of functions through its ability to change shape and to bind to RNA."
New vulnerability found in major human viruses. Discovery of a new feature of a large class of pathogenic viruses may allow development of new antiviral medications for the common cold, polio, and other illnesses, according to a new study. Picornaviruses include rhinoviruses and enteroviruses. Rhinoviruses cause millions of cases of upper respiratory infections ("colds") yearly and contribute to asthma, and enteroviruses are responsible for millions of infections including cases such as meningitis, encephalitis and polio. There are currently no antivirals that can be used for the treatment or prevention of any of the rhino- or enteroviruses.
Scientists confirm usually harmless virus attacks the heart's electrical system. Adenovirus, which typically can cause a common cold, has a far more dangerous impact if it reaches the heart.
Viruses can steal our genetic code to create new human-virus genes. A new study unveils a novel mechanism that allows viruses to produce unexpected proteins. Like a scene out of "Invasion of the Body Snatchers," a virus infects a host and converts it into a factory for making more copies of itself. Now researchers have shown that a large group of viruses, including the influenza viruses and other serious pathogens, steal genetic signals from their hosts to expand their own genomes. The cross-disciplinary team of virologists looked at a large group of viruses known as segmented negative-strand RNA viruses (sNSVs), which include widespread and serious pathogens of humans, domesticated animals and plants, including the influenza viruses and Lassa virus (the cause of Lassa fever). They showed that, by stealing genetic signals from their hosts, viruses can produce a wealth of previously undetected proteins. The researchers labeled them as UFO (Upstream Frankenstein Open reading frame) proteins, as they are encoded by stitching together the host and viral sequences. There was no knowledge of the existence of these kinds of proteins prior to this study. These UFO proteins can alter the course of viral infection and could be exploited for vaccine purposes. The capacity of a pathogen to overcome host barriers and establish infection is based on the expression of pathogen-derived proteins. To understand how a pathogen antagonizes the host and establishes infection, we need to have a clear understanding of what proteins a pathogen encodes, how they function, and the manner in which they contribute to virulence. Viruses cannot build their own proteins, so they need to feed suitable instructions to the machinery that builds proteins in their host's cells. Viruses are known to do this through a process called "cap-snatching," in which they cut the end from one of the cell's own protein-encoding messages (a messenger RNA, or mRNA) and then extend that sequence with a copy of one of their own genes. This gives a hybrid message to be read.
Virus that threatened humanity opens the future. Scientists have developed an innovative therapeutic platform by mimicking the intricate structures of viruses using artificial intelligence. Viruses are uniquely designed to encapsulate genetic material within spherical protein shells, enabling them to replicate and invade host cells, often causing disease. Inspired by these complex structures, researchers have been exploring artificial proteins modeled after viruses. These "nanocages" mimic viral behavior, effectively delivering therapeutic genes to target cells. However, existing nanocages face significant challenges: their small size restricts the amount of genetic material they can carry, and their simple designs fall short of replicating the multifunctionality of natural viral proteins.
Breakthrough microchip reveals how your body fights viruses—in just 90 minutes. By analyzing just a drop of blood, this microchip gives researchers quicker-than-ever insight into how a person’s antibodies are interacting with a virus or other pathogen. This game-changing technology, called mEM, condenses a week’s worth of lab work into 90 minutes, offering a powerful tool for tracking immune responses and fast-tracking vaccine development. Unlike earlier methods, it needs far less blood and delivers more detailed insights, even revealing previously undetected antibody targets on viruses like SARS-CoV-2 and influenza. With the new system, known as microfluidic EM-based polyclonal epitope mapping (mEM), researchers start with four microliters of blood extracted from a human or animal-about one hundred times less than what's required in original EMPEM. The blood is injected in a tiny, reusable chip where viral proteins are stuck to a special surface. As the blood flow through the chip, antibodies recognize and bind to those. Then, the viral proteins -- with any antibodies attached -- are gently released from the chip and prepared for imaging using standard electron microscopy. The entire process only takes about 90 minutes.
Dormant is a condition of biological rest or suspended animation that is temporally inactive but capable of becoming active and awake.
Dormancy is a period in an organism's life cycle when growth, development, and (in animals) physical activity are temporarily stopped. This minimizes metabolic activity and therefore helps an organism to conserve energy. Dormancy tends to be closely associated with environmental conditions. Organisms can synchronize entry to a dormant phase with their environment through predictive or consequential means. Predictive dormancy occurs when an organism enters a dormant phase before the onset of adverse conditions. For example, photoperiod and decreasing temperature are used by many plants to predict the onset of winter. Consequential dormancy occurs when organisms enter a dormant phase after adverse conditions have arisen. This is commonly found in areas with an unpredictable climate. While very sudden changes in conditions may lead to a high mortality rate among animals relying on consequential dormancy, its use can be advantageous, as organisms remain active longer and are therefore able to make greater use of available resources.
Latent is remaining in an inactive or hidden phase; dormant. Lying dormant or hidden until circumstances are suitable for development or manifestation.
Virus Latency is the ability of a pathogenic virus to lie dormant (latent) within a cell, denoted as the lysogenic part of the viral life cycle. A latent viral infection is a type of persistent viral infection which is distinguished from a chronic viral infection. Latency is the phase in certain viruses' life cycles in which, after initial infection, proliferation of virus particles ceases. However, the viral genome is not fully eradicated. The result of this is that the virus can reactivate and begin producing large amounts of viral progeny without the host being infected by new outside virus, denoted as the lytic part of the viral life cycle, and stays within the host indefinitely. Virus latency is not to be confused with clinical latency during the incubation period when a virus is not dormant.
How some gut microbes awaken 'zombie' viruses in their neighbors. Scientists have known for years that colibactin can wreak havoc on human cells. In 2006, a French team reported that mammalian cells that encountered the gut bacteria E. coli suffered fatal damage to their DNA. The researchers linked this damage to a cluster of E. coli genes encoding machinery for building a complex molecule. Dubbed colibactin, the molecule was extraordinarily difficult to study. After many tries, researchers simply couldn't isolate it from the E. coli making it.
Giant Viruses found on Greenland ice sheet. Viruses found on the Greenland ice sheet probably regulate the growth of snow algae on the ice by infecting them. Knowing how to control these viruses could help us reduce the rate of ice-melt.
Lytic Cycle is one of the two cycles of viral reproduction (referring to bacterial viruses or bacteriophages), the other being the lysogenic cycle. The lytic cycle results in the destruction of the infected cell and its membrane. A key difference between the lytic and lysogenic phage cycles is that in the lytic phage, the viral DNA exists as a separate molecule within the bacterial cell, and replicates separately from the host bacterial DNA. The location of viral DNA in the lysogenic phage cycle is within the host DNA, therefore in both cases the virus/phage replicates using the host DNA machinery, but in the lytic phage cycle, the phage is a free floating separate molecule to the host DNA.
Viruses that kill Bacteria. A bacteriophage is a virus that infects and replicates within a bacterium. Phage Therapy.
New findings on animal viruses with potential to infect humans. Study shows how virus family gains entry to mammal cells. Scientists investigating animal viruses with potential to infect humans have identified a critical protein that could enable spillover of a family of organisms called arteriviruses. In a new study, researchers identified a protein in mammals that welcomes arteriviruses into host cells to start an infection. The team also found that an existing monoclonal antibody that binds to this protein protects cells from viral infection. Results from this study demonstrated that FcRn is used for host cell entry by at least five arteriviruses that infect monkeys, pigs and horses, respectively: three diverse strains of simian arteriviruses, porcine reproductive and respiratory syndrome virus 2 (PRRSV-2), and equine arteritis virus (EAV).
A Host-Produced Quorum-Sensing Autoinducer Controls a Phage Lysis-Lysogeny Decision. When a virus infects bacteria, it's called a phage. When VP882 entered salmonella in experiments, it could sense information emitted from bacteria. Bacterial cells communicate by producing and releasing chemical signal molecules that other bacteria pick up, a process called "quorum sensing." The communication lets them figure out how many other bacteria are in the vicinity, allowing them to act as a group and increase the power of disease-causing bacteria to do damage. So in a way, the virus was "overhearing" bacterial conversations. Biologists turn eavesdropping viruses into bacterial assassins.
Protein Transport Channel offers new Target for thwarting Pathogen.
Gesundheit Machine is used to collect samples of a virus from the breath that sick people exhale.
Antiviral Drug are a class of medication used specifically for treating viral infections rather than bacterial ones. Most antivirals are used for specific viral infections, while a broad-spectrum antiviral is effective against a wide range of viruses. Unlike most antibiotics, antiviral drugs do not destroy their target pathogen; instead they inhibit their development.
By targeting flu-enabling protein, antibody may protect against wide-ranging strains. The findings could lead to a universal flu vaccine and more effective emergency treatments. The protein, located on the surface of the virus, enables infected host cells to release the virus so it can spread to other cells. Tamiflu, the most widely used drug for severe flu infection, works by inactivating neuraminidase. However, many forms of neuraminidase exist, depending on the flu strain, and such drugs aren't always effective -- particularly as resistance to the drugs is developing. Typically, anti-neuraminidase antibodies can be broad within a subtype, like H1N1, but an antibody with potent activity across subtypes was unheard of. At first, we did not believe our results. Especially the ability of the antibodies to cross between influenza A and influenza B viruses is just mind-boggling. It is amazing what the human immune system is capable of if presented with the right antigens. To find out whether the antibodies could be used to treat severe cases of flu, Krammer and colleagues tested them in mice that were given a lethal dose of influenza virus. All three antibodies were effective against many strains, and one antibody, called "1G01," protected against all 12 strains tested, which included all three groups of human flu virus as well as avian and other nonhuman strains. "All the mice survived, even if they were given the antibody 72 hours after infection," Ellebedy says. "They definitely got sick and lost weight, but we still saved them. It was remarkable. It made us think that you might be able to use this antibody in an intensive care scenario when you have someone sick with flu and it's too late to use Tamiflu." Tamiflu must be administered within 24 hours of symptoms. A drug that could be used later would help many people diagnosed after the Tamiflu window has closed. But before the researchers could even think of designing such a drug based on the antibody, they needed to understand how it was interfering with neuraminidase.
Double-stranded RNA Activated Caspase Oligomerizers is a group of experimental antiviral drugs under development at the Massachusetts Institute of Technology. DRACOs May Be Effective Against All Viruses.
Some Viruses produce Insulin-Like Hormones that can Stimulate Human Cells -- and have potential to cause disease. Scientists have identified four viruses that can produce insulin-like hormones that are active on human cells. The discovery brings new possibilities for revealing biological mechanisms that may cause diabetes or cancer. Every cell in your body responds to the hormone insulin, and if that process starts to fail, you get diabetes.
Retrovirus is a type of RNA virus that inserts a copy of its genome into the DNA of a host cell that it invades, thus changing the genome of that cell. Such viruses are specifically classified as single-stranded positive-sense RNA viruses. Once inside the host cell's cytoplasm, the virus uses its own reverse transcriptase enzyme to produce DNA from its RNA genome, the reverse of the usual pattern, thus retro (backwards). The new DNA is then incorporated into the host cell genome by an integrase enzyme, at which point the retroviral DNA is referred to as a provirus. The host cell then treats the viral DNA as part of its own genome, transcribing and translating the viral genes along with the cell's own genes, producing the proteins required to assemble new copies of the virus. It is difficult to detect the virus until it has infected the host. At that point, the infection will persist indefinitely. Rotavirus is the most common cause of diarrhoeal disease among infants and young children. The genome of a virus can be either single stranded RNA (ssRNA), double stranded RNA (dsRNA), single stranded DNA (ssDNA), double stranded DNA ds(DNA), or a mix of ssDNA and dsDNA. Influenza A virus subtype H1N1 (wiki) - HIV-1 (wiki) - HIV-2 (wiki).
Norovirus is a very contagious virus that causes vomiting and diarrhea. People of all ages can get infected and sick with norovirus. Norovirus spreads easily! People with norovirus illness can shed billions of norovirus particles. And only a few virus particles can make other people sick. Norovirus sometimes referred to as the winter vomiting bug, is the most common cause of gastroenteritis. This usually develops 12 to 48 hours after being exposed. Recovery typically occurs within 1 to 3 days. Complications may include dehydration. The virus is usually spread by the fecal–oral route. This may be by contaminated food or water or person-to-person contact. It may also spread via contaminated surfaces or through the air. Risk factors include unsanitary food preparation and sharing close quarters. Diagnosis is generally based on symptoms. Confirmatory testing may be done for public health purposes. Prevention involves proper hand washing and disinfection of contaminated surfaces. Alcohol-based hand sanitizers are less effective. A vaccine does not exist. There is no specific treatment. Efforts involve supportive care such as drinking sufficient fluids or intravenous fluids. Oral rehydration solutions are the preferred fluids to drink, although other drinks without caffeine or alcohol can help. Norovirus results in about 685 million cases of disease and 200,000 deaths globally a year. It is common both in the developed and developing world. Those under the age of five are most often affected and in this group it results in about 50,000 deaths in the developing world. Disease more commonly occurs in winter months. It often occurs in outbreaks, especially among those living in close quarters. In the United States, it is the cause of about half of foodborne disease outbreaks. The disease is named after Norwalk, Ohio, where an outbreak occurred in 1968.
Norovirus Evades Immune System by Hiding Out in Rare Gut Cells. Noroviruses are the leading cause of non-bacterial gastroenteritis in the world and are estimated to cause 267 million infections and 20,000 deaths each year. This virus causes severe diarrhea, nausea, and stomach pain.
95% of people carry Epstein-Barr Virus and scientists may have just found how to stop it. EBV is an extremely common infection linked to cancer and chronic disease, and scientists have developed a first-of-its-kind antibody to block Epstein-Barr virus. By using mice engineered with human antibody genes, researchers created powerful human-like antibodies that block the virus from attaching to and entering immune cells. One of these antibodies completely prevented infection in lab models with human immune systems, marking a breakthrough after years of difficulty tackling EBV’s ability to invade nearly all B cells. By working with mice engineered to produce human antibodies, the team created new monoclonal antibodies designed to stop the virus from attaching to and entering human immune cells. A major hurdle in developing these treatments has been identifying antibodies that can stop EBV without triggering an immune reaction against the therapy itself, which often happens when antibodies come from non-human sources. To address this, the researchers focused on two viral proteins, gp350 and gp42. The gp350 protein helps the virus attach to human cells, while gp42 allows it to fuse with and enter those cells.
Post-transplant lymphoproliferative disorders (PTLD) are a serious and sometimes life-threatening form of lymphoma that can develop after transplantation, most often driven by uncontrolled EBV infection.
Adenoviridae have more than 50 distinct adenoviral serotypes have been found to cause a wide range of illnesses, from mild respiratory infections in young children (known as the common cold) to life-threatening multi-organ disease in people with a weakened immune system.
Zoonosis are infectious diseases of animals (usually vertebrates) that can naturally be transmitted to humans.
Shope Papilloma Virus also known as cottontail rabbit papilloma virus or Kappapapillomavirus 2, is a papillomavirus which infects certain species of rabbit and hare, causing cancerous lesions (carcinomas) resembling horns, typically on or near the animal's head, thus the nick name Frankenstein Rabbit. The carcinomas can metastasize or become large enough to interfere with the host's ability to eat, causing starvation. In the 1930s, hunters in northwestern Iowa reported that the rabbits they shot had several "horn" protrusions on many parts of their bodies including their faces and necks. The papillomavirus life cycle begins with cells actively multiplying in epithelial cells of basal and parabasal layers. The differentiation of these cells is necessary for this virus to complete its life cycle. Transforming proteins E6 and E7 induce the S-phase in the lower epithelial layers. Viral replication proteins E1 and E2 are also required to form the papilloma and keep the episomal viral genome replication low. Rabbits re-infected with the virus exhibit some or complete immunity, and can transmit the virus to other wild rabbits, and from wild to domestic rabbits. A domestic strain cannot transmit it to another domestic rabbit, however. Immunologically, the papillomatosis virus is not related to fibroma or myxoma in rabbits.
Toxoplasma Gondii is an obligate intracellular, parasitic alveolate that causes the disease toxoplasmosis. Found worldwide, T. gondii is capable of infecting virtually all warm-blooded animals, but felids such as domestic cats are the only known definitive hosts in which the parasite can undergo sexual reproduction. Parasites.
Cytomegalovirus is a genus of viruses in the order Herpesvirales, in the family Herpesviridae, in the subfamily Betaherpesvirinae. Humans and monkeys serve as natural hosts.
Human Metapneumovirus is a negative-sense single-stranded RNA virus of the family Pneumoviridae and is closely related to the Avian metapneumovirus subgroup C. As of 2016, it was the second most common cause (after respiratory syncytial virus (RSV)) of acute respiratory tract illness in otherwise-healthy children under the age of 5 in a large US outpatient clinic. It is likely that transmission occurs by contact with contaminated secretions, via droplet, aerosol, or fomite vectors. No treatment is yet known. Chimps are dying of the common cold.
Ribavirin or tribavirin, is an antiviral medication used to treat RSV infection, hepatitis C and some viral hemorrhagic fevers.
Parasitism is a non-mutual relationship between species, where one species, the parasite, benefits at the expense of the other, the host.
Brain Eating Amoeba is a type of cell or organism which has the ability to alter its shape, primarily by extending and retracting pseudopods.
Virulence Factor are molecules produced by bacteria, viruses, fungi, and protozoa that add to their effectiveness and enable them to achieve the following: colonization of a niche in the host (this includes attachment to cells). Immunoevasion, evasion of the host's immune response. Immunosuppression, inhibition of the host's immune response. Entry into and exit out of cells (if the pathogen is an intracellular one), Obtain nutrition from the host. Specific pathogens possess a wide array of virulence factors. Some are chromosomally encoded and intrinsic to the bacteria (e.g. capsules and endotoxin), whereas others are obtained from mobile genetic elements like plasmids and bacteriophages (e.g. some exotoxins). Virulence factors encoded on mobile genetic elements spread through horizontal gene transfer, and can convert harmless bacteria into dangerous pathogens. Bacteria like Escherichia coli O157:H7 gain the majority of their virulence from mobile genetic elements. Gram-negative bacteria secrete a variety of virulence factors at host-pathogen interface, via membrane vesicle trafficking as bacterial outer membrane vesicles for invasion, nutrition and other cell-cell communications. It has been found that many pathogens have converged on similar virulence factors to battle against eukaryotic host defenses. These obtained bacterial virulence factors have two different routes used to help them survive and grow: The factors are used to assist and promote colonization of the host. These factors include adhesins, invasins, and antiphagocytic factors. The factors, including toxins, hemolysins, and proteases, bring damage to the host. Cold Weather and Freezing Temperatures affect the Body.
CRISPR protein might yield new tests for many viruses. All of the previously known CRISPR immune systems protect bacteria by deactivating genes from an invading virus. Now, a recently discovered CRISPR protein, called Cas12a2, has been found to act as a kind of multi-purpose self-destruct system for bacteria, capable of degrading single-stranded RNA, single-stranded DNA and double-stranded DNA. This ability could lead to a new approach to developing diagnostics for diseases such as COVID-19 and the flu. Using a high-resolution imaging technique called cryo-EM, the team discovered that when this protein, named Cas12a2, binds to a specific sequence of genetic material from a potentially dangerous virus, called a target RNA, a side portion of Cas12a2 swings out to reveal an active site, similar to a sprung-open switchblade knife. Then, the active site starts to indiscriminately cut any genetic material it comes into contact with. The researchers discovered that, with a single mutation to the Cas12a2 protein, the active site degrades only single-stranded DNA -- a feature especially useful in developing new diagnostics tailored for any of a wide range of viruses.
Simple nasal swab can provide early warning of emerging viruses. Researchers have found that testing for the presence of a single immune system molecule on nasal swabs can help detect stealthy viruses not identified in standard tests.
Coronavirus - COVID-19 - SARS-CoV-2
Coronavirus Disease 2019 is an infectious disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The disease was first identified in 2019 in Wuhan, China, and has since spread globally, resulting in the 2019–20 coronavirus pandemic. Common symptoms include fever, cough, and shortness of breath. Muscle pain, sputum production and sore throat are less common. While the majority of cases result in mild symptoms, some progress to severe pneumonia and multi-organ failure. 20% show no symptoms but are contagious. The rate of deaths per number of diagnosed cases is on average 3.4%, ranging from 0.2% in those under 20, to approximately 15% in those over 80 years old. Patients with preexisting conditions, including hypertension, diabetes mellitus, and cardiovascular disease, are most at risk and represent the vast majority of deaths. The infection is typically spread from one person to another via respiratory droplets produced during coughing and sneezing. Time from exposure to onset of symptoms is generally between 2 and 14 days, with an average of five days. The standard method of diagnosis is by reverse transcription polymerase chain reaction (rRT-PCR) from a nasopharyngeal swab. The infection can also be diagnosed from a combination of symptoms, risk factors and a chest CT scan showing features of pneumonia. Recommended measures to prevent infection include frequent hand washing, maintaining distance from others (social distancing), and keeping hands away from the face. The use of masks is recommended for those who suspect they have the virus and their caregivers, but not the general public. There is no vaccine or specific antiviral treatment for COVID-19. Management involves treatment of symptoms, supportive care, isolation, and experimental measures. The World Health Organization (WHO) declared the 2019–20 coronavirus outbreak a pandemic and a Public Health Emergency of International Concern (PHEIC). Evidence of local transmission of the disease has been found in many countries across all six WHO regions. Vaccines.
Coronavirus COVID-19 Global Cases Map (Johns Hopkins University) - WHO - CDC - Pandemic - Containment - ncov2019.live - Coronavirus in the U.S.: Latest Map and Case Count - COVID-19 School Response Dashboard
Death Rate or Mortality Rate is not the same as Number of Deaths. Mortality Rate or Death Rate is a measure of the number of deaths scaled to the size of that population, per unit of time. Mortality Rate is typically expressed in units of deaths per 1,000 individuals per year. Case Fatality Rate is the proportion of deaths from a certain disease compared to the total number of people diagnosed with the disease for a particular period. A CFR is conventionally expressed as a percentage and represents a measure of disease severity. CFRs are most often used for diseases with discrete, limited-time courses, such as outbreaks of acute infections. A CFR can only be considered final when all the cases have been resolved (either died or recovered). The preliminary CFR, for example, during an outbreak with a high daily increase and long resolution time would be substantially lower than the final CFR.
Infection Rate - Long Covid - Vulnerabilities - Asymptomatic
Excess Death Rate among Republican voters was 43% higher than the excess death rate among Democratic voters" after vaccine eligibility was opened. Excess mortality is a term used in epidemiology and public health that refers to the number of deaths from all causes during a crisis above and beyond what we would have expected to see under ‘normal’ conditions. We’re interested in how the number of deaths during the COVID-19 pandemic compares to the deaths we would have expected had the pandemic not occurred — a crucial quantity that cannot be known but can be estimated in several ways. Excess deaths are typically defined as the difference between the observed numbers of deaths in specific time periods and expected numbers of deaths in the same time periods.
Death Risk Factors - Vulnerable
How Doctors Can Predict Who Dies From COVID (youtube) - People who get infected with covid-19, around 15 percent require hospitalization or spend more than one day in the hospital. Less than 5 percent require ICU or breathing help. Around .05 percent to 1 percent die from the covid-19 virus, mostly from a cytokine storm, which is when an infection triggers your immune system to flood your bloodstream with inflammatory proteins called cytokines. They can kill tissue and damage your organs. Factors that increase your chances of hospitalization or death includes, if you're old age, if you're a smoker, if you're a male, if you have type A blood, or if you have co-morbidities such as diabetes, obesity and heart disease, just to name a few of the things that would weaken your immune system. A blood test could help by determining the level of hemoglobin platelets and white blood cells or neutrophils monocytes (neutrophilis, basophilis, eosinophils, monocytes, lymphocytes) (troponin, dimer, ferritin, CRP or c-reactive protein). Hypervirulent - Long Covid.
Comorbidity is the presence of one or more additional conditions often co-occurring (that is, concomitant or concurrent) with a primary condition. Comorbidity describes the effect of all other conditions an individual patient might have other than the primary condition of interest, and can be physiological or psychological.
Off-Target Immune System Response Could Predict COVID-19 Severity. Among the new study findings is that a subset of these autoimmune antibodies that bind to DNA or to a particular type of fat molecule, a lipid called phosphatidylserine, were more often twice as abundant at the start of coronavirus infection in those whose conditions worsened quickly than in those whose health did not decline. Patients with these elevated levels of autoimmune antibodies were five to seven times more likely to develop severe disease than those whose antibodies levels were stable.
Estimated pulse wave velocity predicts severe COVID. Researchers found that estimated Pulse Wave Velocity, a readily available marker of arterial stiffness, has been shown to be an effective addition in identifying patients at risk of mortality in hospital due to COVID-19.
Proteins may halt the severe cytokine storms seen in Covid-19 patients. Study finds specific cells in the lungs, nasal passages, and intestines that are more susceptible to infection. Scientists discovered that the viral "spike" protein binds to a receptor on human cells known as angiotensin-converting enzyme 2 or ACE2. Another human protein, an enzyme called TMPRSS2, helps to activate the coronavirus spike protein, to allow for cell entry. The combined binding and activation allows the virus to get into host cells. Expression of the ACE2 gene appeared to be correlated with activation of genes that are known to be turned on by interferon, a protein that the body produces in response to viral infection. Angiotensin-converting enzyme 2 is found in the heart, kidneys and other organs. In COVID-19, the respiratory disease caused by the novel coronavirus, it is thought to play a role in how the infection progresses into the lungs.
Common gene variant linked to COVID mortality. What manifests as minor, flu-like symptoms in some individuals spirals into severe disease, disability, and even death in others. Researchers demonstrated that mice with gene variants previously linked to Alzheimer's disease were at greater risk of dying when infected with COVID. Most people have a form called APOE3, but 40 percent of the population carries at least one copy of the APOE2 or APOE4 variant. Individuals with APOE2 or APOE4 produce proteins that differ from APOE3 protein by one or two amino acids. One or two amino acids make a difference. Individuals with APOE4 are at greater risk of developing Alzheimer's and atherosclerosis.
Antibody blocks infection by the SARS-CoV-2 in cells, scientists discover. Researchers report that they have identified a fully human monoclonal antibody that prevents the SARS-CoV-2 (COVID-19) virus from infecting cultured cells. The discovery is an initial step towards developing a fully human antibody to treat or prevent the respiratory disease COVID-19 caused by the novel coronavirus SARS-CoV-2.
New SP1-77 Antibody neutralizes all known SARS-CoV-2 variants in lab tests.
Strong activation of anti-bacterial T cells linked to severe COVID-19. A type of anti-bacterial T cells, so-called MAIT cells, are strongly activated in people with moderate to severe COVID-19 disease, according to a new study.
Vitamin D levels appear to play role in COVID-19 mortality rates. Patients with severe deficiency are twice as likely to experience major complications.
In laboratory dish tests, extracts from the flowers of tall goldenrod (Solidago altissima) and the rhizomes of the eagle fern (Pteridium aquilinum) each blocked SARS-CoV-2 from entering human cells. The active compounds are only present in miniscule quantities in the plants. It would be ineffective, and potentially dangerous, for people to attempt to treat themselves with them, the researchers stress. In fact, the eagle fern is known to be toxic, they warn. A new study led by Emory University has found that two common wild plants can inhibit the activity of the virus causing Covid-19 to infect human cells.
Spike mutations help SARS-CoV-2 infect the brain. This could help us understand neurological symptoms of COVID-19. New research has uncovered a series of mutations in the SARS-CoV-2 spike protein that enhanced the virus ability to infect the brains of mice. The findings may help scientists understand its neurological symptoms and the mystery of 'long COVID,' and they could one day even lead to specific treatments to protect and clear the virus from the brain.
Immune response study explains why some people don't get COVID-19. Using single-cell sequencing technology, researchers provide the most comprehensive timeline to date of how the body responds to SARS-CoV-2 exposure.
Why are some people more vulnerable to covid-19? Why are Black or African American persons, Hispanic or Latino persons, and American Indian or Alaska Native persons more vulnerable to covid-19 and have higher rates of hospitalizations and death? This goes beyond underlying medical conditions like Type 2 diabetes, high blood pressure, heart disease, and obesity, as well as children with obesity, diabetes, asthma or chronic lung disease, sickle cell disease, or immunosuppression. Researchers are continuing to learn about the complicated biological and social reasons why some people get sicker than others. Peru has the world's highest COVID death rate in November 2021. Why are some people immune to covid 19? Why do some people never have symptoms?
Anti-Body Testing
There are 2 Types of COVID-19 Antibody Tests: Spike Protein Test and a Nucleocapsid Test. Spike Protein Test can detect antibodies from a prior or recent infection, regardless of whether symptoms were present. A positive result means your body's immune system has generated a response to a prior COVID-19 infection. A positive result or a negative result may also occur after a COVID-19 vaccination. Nucleocapsid Test can only detect antibodies from a prior or recent infection. The test is designed to detect antibodies against the virus that causes COVID-19. Antibodies are proteins produced by the immune system in response to an infection and are specific to that particular infection. Antibodies also known as immunoglobulins. Antibody testing, also known as serology testing, is usually done after full recovery from COVID-19. Eligibility may vary, depending on the availability of tests. A health care professional takes a blood sample, usually by a finger prick or by drawing blood from a vein in the arm. Then the sample is tested to determine whether you've developed antibodies against the virus. The immune system produces these antibodies — proteins that are critical for fighting and clearing out the virus. Exemptions.
If you contracted the covid-19 virus and have had a test that confirms you have the anti-bodies, do you still need a vaccine? It depends on the person and the vaccine type. It also depends on if the person is at high risk because of a weak immune system. It also depends on if the person is at high risk of reinfection because of increased social contacts or because they are around many people throughout the day. It also depends on if the person is irresponsible and does not wear a mask or wash their hands, especially when the infection rate are still high. It also depends on if the person is at high risk because of a poor diet or because of other environmental factors that can cause the immune system to weaken. People who have had COVID-19 can get re-infected and people who had a vaccine can also get re-infected. The most important thing is, is the persons immune system strong enough to keep them out of the hospital or keep them from dying. To just rely on a positive covid-19 test or just to rely on a vaccine is extremely ignorant. There are many factors that a person needs to be educated about in order to fully protect themselves against diseases, and also protect themselves from misinformation.
Antibodies can take days or weeks to develop in the body following exposure to a SARS-CoV-2 (COVID-19) infection and it is unknown how long they stay in the blood. Serology test performance and antibody test accuracy. Serology tests detect the presence of antibodies in the blood from the body’s adaptive immune response to an infection, like COVID-19. They do not detect the virus itself. In the early days of an infection when the body's adaptive immune response is still building, antibodies may not be detected. This limits the test's effectiveness for diagnosing current COVID-19 and is one reason serology tests should not be used to diagnose or exclude acute COVID-19 infection. Serology tests play a role in the fight against COVID-19 by helping health care professionals identify individuals who may have developed an adaptive immune response to SARS-CoV-2. However, to use serology tests properly, it is important to understand their performance characteristics and limitations. The performance of these tests is described by their "sensitivity," or their ability to identify those with antibodies to SARS-CoV-2 (true positive rate), and their "specificity," or their ability to identify those without antibodies to SARS-CoV-2 (true negative rate). A test's sensitivity can be estimated by determining whether or not it is able to detect antibodies in blood samples from patients who have been confirmed to have COVID-19 with a nucleic acid amplification test, or NAAT. November 06, 2020, The U.S. Food and Drug Administration authorized the first serology test that detects neutralizing antibodies from recent or prior SARS-CoV-2 infection, which are antibodies that bind to a specific part of a pathogen and have been observed in a laboratory setting to decrease SARS-CoV-2 viral infection of cells. Rapid antibody testing finger prick blood test. Antibody tests are aimed at finding evidence of your body's immune response to a past infection with the virus, and some testes can actually give you scores that reflect your levels. The tests may give you numerical readings that indicate the level of antibodies in your blood that bind to specific SARS-CoV-2 proteins. The higher your number is, the more likely you are to be protected. But the immune system is more than just antibodies, so even with low detectable levels in your blood does not necessary mean that you're not defenseless. And consumers need to be aware that some tests on the market are not standardized. They can have varying degrees of sensitivity and look for different antibodies. A positive result means that the test detected antibodies to the virus that causes COVID-19, and it is possible that you had a recent or prior COVID-19 infection and you have developed an adaptive immune response to the virus. But a positive antibody test does not necessarily mean you are immune from SARS-CoV-2 infection, as it is not known whether having antibodies to SARS-CoV-2 will protect you from getting infected again. A negative result on a SARS-CoV-2 antibody test means antibodies to the virus were not detected in your sample. It could mean that you have not been infected with COVID-19 previously, or you had COVID-19 in the past but you did not develop or have not yet developed detectable antibodies. Many people who have COVID-19 have mild or no symptoms, antibody tests may be the best way to find out how far the new coronavirus has spread. These blood tests can show who's been exposed to the virus and who hasn't. It is vital to develop anti-SARS-CoV-2 immunity via natural infection or by vaccination. However, in COVID-19 recovered individuals, a sharp decline in humoral immunity has been observed after 6 – 8 months of symptom onset. We can't use antibody tests to show that vaccines are working because many COVID-19 antibody tests are not designed to specifically detect antibodies that develop as a result of vaccination, and thus cannot show whether antibodies are of the right quantity or quality for protection against infection or illness. Antibody testing is not currently recommended to assess immunity after COVID-19 vaccination.
Cross-Neutralization of SARS-CoV-2 by a human monoclonal SARS-CoV antibody.
Cross-Reactivity is the reactivity of an observed agent which initiates reactions outside the main reaction expected. Cross Reactive Immunity.
New testing system using Janus particles rapidly and accurately detects COVID-19. A research group has developed a new COVID-19 testing system using Janus particles -- microparticles with two sides possessing distinctive molecular properties. These particles are engineered to bind specifically to target antigens, such as viral proteins, creating a low-cost, accurate, and rapid means of testing for viral diseases. The system's versatility means it can potentially be used to test for other diseases and biomarkers linked to other conditions. A group of researchers has developed a new quantitative testing system called the "Express Biochecker," which provides a simple, rapid, and low-cost method for detecting the coronavirus N protein.
CDC does not recommend checking for antibodies after vaccination. Their reasoning includes the fact that, while there are several COVID-19 antibody tests being used by commercial labs, most look for antibodies that are different than the ones produced by the vaccines in use, so they won't offer much information. When most people sign up for a test, most laboratories and providers are typically testing for anti-nucleocapsid antibodies. The problem with that is those are not antibodies that would be created by the vaccine, but only through natural infection. So in other words, many of the antibody tests available now would only be able to tell you whether you have antibodies as a result of getting COVID, and not from having received a vaccine. The test results will show the number of antibodies the person has to the spike protein, but we have no idea yet how many antibodies a person needs to be protected. Someone could have no antibodies, but that doesn't necessarily mean they have no protection against the virus. It could be that if exposed, other helper cells, such as B and T cells, would come to the rescue as a result of vaccination. If an immunocompromised patient does not have antibodies, doctors may consider bolstering their protection with another dose of the vaccine, continued masking and other precautions. Some countries are requiring antibody tests to the spike protein as a condition for entering the country, which is usually more than $100 at one of the country's private labs. But that's not a measure of how protected you are. while there are antibody tests to verify protection from vaccines for diseases such as mumps and measles, those took decades to develop, and with COVID-19 we're only at a year and a half. Viral Load - Vaccines.
Protective T cells remain 20 months after COVID-19, study finds. Patients infected with SARS-CoV-2 develop protective immune responses, mediated by virus-specific T cells and antibodies, shortly after the infection.
Pox Party or flu parties are social activities in which children are deliberately exposed to infectious diseases such as chickenpox. Such parties originated to "get it over with" before vaccines were available for a particular illness or because childhood infection might be less severe than infection during adulthood, according to proponents. For example, measles is more dangerous to adults than to children over five years old. Deliberately exposing people to diseases has since been discouraged by public health officials in favor of vaccination, which has caused a decline in the practice of pox parties, although flu parties saw a resurgence in the early 2010s. Another, more modern, method of intentional contagion involves shipping infectious material. In many parts of the world, shipping infectious items is illegal or tightly regulated. Hygiene Hypothesis.
Intentional Contagion of Infection is the act by which a human being deliberately infects another with a pathogen knowing that they will be infected. In some legislations of some countries this act has been criminalized, managing to prosecute it and consider it as aggravating for fraud or recklessness. One of the most frequent cases of intentional contagion is that of viruses and bacteria that are considered sexually transmitted infections, being commonly the most common methods through the malicious use of syringes and the unsafe sexual act, such as the criminal transmission of HIV. Intentional contagion of infection is also called voluntary contagion, conscious contagion, or intentional transmission.
Mutations- Variants - Strains
Mutations in SARS-CoV-2 offer insights into virus evolution. By analyzing virus genomes from over 7,500 people infected with COVID-19, researchers have characterized patterns of diversity of SARS-CoV-2 virus genome, offering clues to direct drugs and vaccine targets. The study identified close to 200 recurrent genetic mutations in the virus, highlighting how it may be adapting and evolving to its human hosts. The new coronavirus, like all other viruses, mutates, or undergoes small changes in its genome. D614G Mutation. A recently published study suggested that the new coronavirus, SARS-CoV-2, had already mutated into one more and one less aggressive strain. Another possibility is that SARS-CoV-2 will mutate in a potentially beneficial way, making it more difficult for the virus to infect people. (600 mutations and several new strains). Replication errors are the main source of mutations. It has been estimated that uncorrected replication errors occur with a frequency of 10-9 - 10-11 for each nucleotide added by DNA polymerases. Since a cell division requires synthesis of 6 X 109 nucleotides, the mutation rate is about one per cell division. Silent' Mutations Gave the Coronavirus an Evolutionary Edge. RNA folding may help explain how the coronavirus became so hard to stop after it spilled over from wildlife to humans. Researchers have identified a number of 'silent' mutations in the roughly 30,000 letters of the COVID-19 virus's genetic code that helped it thrive once it made the leap from bats and other wildlife to humans -- and possibly helped set the stage for the global pandemic. New Mathematical Model improves Tracking of Epidemics by accounting for Mutations in Diseases. Containment.
Delta Variant is highly contagious, more than 2x as contagious as previous variants. The B.1.617.2 (delta) variant of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus that causes coronavirus disease 2019 (Covid-19), has contributed to a surge in cases in India and has now been detected across the globe, including a notable increase in cases in the United Kingdom.
Omicron variant is a variant of SARS-CoV-2, the virus that causes COVID-19. It was first reported to the World Health Organization (WHO) from South Africa on 24 November 2021. On 26 November 2021, the WHO designated it as a variant of concern and named it "Omicron", the fifteenth letter in the Greek alphabet (Greek letters are used to identify specific variants of SARS-CoV-2). The variant has an unusually large number of mutations, several of which are novel.
Variant is a subtype of a microorganism that is genetically distinct from a main strain, but not sufficiently different to be termed a distinct strain. A similar distinction is made in botany between different cultivated varieties of a species of plant, termed cultivars.
There are 200 different varieties of viruses that can cause the common cold.
Strain is a genetic variant, a subtype or a culture within a biological species. Strains are often seen as inherently artificial concepts, characterized by a specific intent for genetic isolation. This is most easily observed in microbiology where strains are derived from a single cell colony and are typically quarantined by the physical constraints of a Petri dish. Strains are also commonly referred to within virology, botany, and with rodents used in experimental studies.
New Variants and Strains. B.1.1.7 Coronavirus Variant has 17 recent mutations that change or delete amino acids in viral proteins. At the heart of each coronavirus is its genome, a twisted strand of nearly 30,000 “letters” of RNA. These genetic instructions force infected human cells to assemble up to 29 kinds of proteins that help the coronavirus multiply and spread. As viruses replicate, small copying errors known as mutations naturally arise in their genomes. A lineage of coronaviruses will typically accumulate one or two random mutations each month. Some mutations have no effect on the coronavirus proteins made by the infected cell. Other mutations might alter a protein’s shape by changing or deleting one of its amino acids, the building blocks that link together to form the protein. Through the process of natural selection, neutral or slightly beneficial mutations may be passed down from generation to generation, while harmful mutations are more likely to die out. B.1.1.7 gained many of its mutations within a single person. People with weakened immune systems can remain infected with replicating coronaviruses for several months, allowing the virus to accumulate many extra mutations. Why Are the New Strains of COVID-19 More Contagious? Mutation N501Y is in the receptor binding domain of the Spike protein of the virus. Scientists believe that this mutation may cause it to bind more tightly to the human angiotensin-converting enzyme 2 receptor. Other changes in the Spike protein may allow this mutation to evade detection by certain polymerase chain reaction, which may cause a greater infectivity, or less susceptibility to vaccine. More severe illness hasn't been seen with the new variant. But if more people get infected, it follows that more will get sick and need hospital care. 501.V2 Strain.
Coronavirus variants predicts virus evolving to escape current vaccines. A new study suggests current vaccines and monoclonal antibody therapies provide less neutralizing activity against the U.K. and South Africa variants of SARS-CoV-2.
Scientists identify mechanism that may influence infectivity of SARS-CoV-2 variants. An enzyme process alters spike protein function. Scientists have found that a process in cells may limit infectivity of SARS-CoV-2, and that mutations in the alpha and delta variants overcome this effect, potentially boosting the virus's ability to spread. Scientists studied the effects of GALNT activity on spike protein in fruit fly and mammalian cells. The experiments showed that one enzyme, GALNT1, adds sugars to wild-type spike protein, and this activity reduces furin cleavage. By contrast, mutations to the spike protein, like those in the alpha and delta variants, decrease GALNT1 activity and increase furin cleavage. This suggested that GALNT1 activity may partially suppress furin cleavage in wild-type virus, and that the alpha and delta mutations overcome this effect, allowing furin cleavage to go unchecked.
How human disease-causing genes prevent adaptations to remove them.
COVID-19 is a reminder of the challenges of emerging infectious diseases. The emergence and rapid increase in cases of coronavirus disease 2019 (COVID-19), a respiratory illness caused by a novel coronavirus, pose complex challenges to the global public health, research and medical communities, write scientists.
Symptoms
What Coronavirus Symptoms Look Like, Day By Day (youtube) - After being exposed to the virus that causes COVID-19, it can take as few as two and as many as 14 days for symptoms to develop. Cases range from mild to critical. The average timeline from the first symptom to recovery is about 17 days, but some cases are fatal. Here's what it looks like to develop COVID-19, day by day. Coronavirus could attack immune system like HIV by targeting protective cells. Researchers in China and the US find that the virus that causes Covid-19 can destroy the T cells that are supposed to protect the body from harmful invaders. The reason, they suspected, was the lack of a membrane fusion function. Sars, which killed hundreds in a 2003 outbreak, can only infect cells carrying a specific receptor protein known as ACE2, and this protein has an extremely low presence in T cells. New antibody tests can detect whether people have had the coronavirus after they recover, but scientists still aren't sure whether people can get re-infected. Way more people may have gotten coronavirus than we thought. Serological Test Validation. April 23, 2020 - New York's first survey of coronavirus antibodies showed that 13.9% of those tested had coronavirus antibodies in their system, meaning they have contracted and recovered from the virus, New York Governor Andrew Cuomo said Thursday. That suggests that 2.7 million people have been infected statewide. The survey was taken from a sample size of about 3,000 people found outside their homes, shopping at essential businesses, such as grocery stores, which remain open. Results show antibodies in 12% of women and 15.9% of men, but a disproportionate rate of antibodies in black and Latino New Yorkers. Masks.
Losing Sense of Smell - Is it just a Cold? - Brain Fog
COVID-19 Animation: What Happens If You Get Coronavirus? (youtube) - The virus exploits the ribosomes and the packaging structure in your cells membrane. You breathe in air through the trachea or wind pipe into the lungs that consists of five lobes, then through large tubes called bronchi. Then through smaller tubes called bronchioles, then into tiny sacs called alveoli, which are flexible. The capillaries surround your alveoli, this is where 02 and co2 are transported. Mucus in your airways help catch pathogens. But when to much inflammation the alveoli can fill up with mucus from the immune response. Lobar pneumonia where one lobe is infected. Bronchopneumonia wher4 both lobes are infected.
Asymptomatic - No Symptoms
Asymptomatic Carriers. 30 percent of people with COVID-19 show no symptoms. Asymptomatic people carry as much virus in their nose and throat and lungs as people exhibiting symptoms. They also carry, and spread it, for almost as long. Asymptomatic people were contagious for about 17 days and those with symptoms were contagious for up to 20 days. One theory suggests that some people have partial immunity to the coronavirus due to so-called "memory" T cells—white blood cells that run the immune system and are in charge of recognizing invaders. Researchers at NIH are looking into a theory that suggests ACE2 receptors may affect the severity of illness a person develops from the new coronavirus. The coronavirus can "latch" onto ACE2 receptors, which in healthy people keep blood pressure stable, then travel through the body and replicate. Researchers are intrigued by the receptors because they've theorized that minimizing those receptors may obstruct the virus' ability to replicate or "trick the virus into attaching itself to a drug" instead, so it's not able to replicate and travel through the body. Another possibility is that allergic reactions may protect you by down-regulating the receptor. Another theory suggests that childhood vaccines may have provided partial immunity against the new coronavirus for some patients.
Atypical Pneumonia
Walking Pneumonia is a less serious form of the lung infection pneumonia and is any type of pneumonia not caused by one of the pathogens most commonly associated with the disease. It's often caused by bacteria called Mycoplasma pneumoniae, but other bacteria or viruses can also cause it. Most kids with this type of pneumonia don't feel sick enough to stay home — hence, the name "walking" pneumonia. There are no signs and symptoms of lobar consolidation, meaning that the infection is restricted to small areas, rather than involving a whole lobe. As the disease progresses, however, the look can tend to lobar pneumonia. Despite general symptoms and problems with the upper respiratory tract (such as high fever, headache, a dry irritating cough followed later by a productive cough with radiographs showing consolidation), there are in general few physical signs. The patient looks better than the symptoms suggest. Silent hypoxia may occur and not be noticed, but will be picked up by pulse oximetry. There is no response to common antibiotics such as sulfonamide and beta-lactams like penicillin. Absence of leukocytosis. Extrapulmonary symptoms, related to the causing organism. Moderate amount of sputum, or no sputum at all (i.e. non-productive). Lack of alveolar exudate.
Reinfection Rates. There are few real-world epidemiologic studies that exist to support the benefit of vaccination for previously infected persons.
Angiotensin-converting enzyme 2 is an enzyme attached to the membrane of cells located in the intestines, kidney, testis, gallbladder, and heart. ACE2 lowers blood pressure by catalyzing the hydrolysis of angiotensin II (a vasoconstrictor peptide) into angiotensin (1–7) (a vasodilator). ACE2 counters the activity of the related angiotensin-converting enzyme (ACE) by reducing the amount of angiotensin-II and increasing Ang(1-7), making it a promising drug target for treating cardiovascular diseases. ACE2 also serves as the entry point into cells for some coronaviruses, including HCoV-NL63, SARS-CoV, and SARS-CoV-2. The SARS-CoV-2 spike protein itself is known to damage the epithelium via downregulation of ACE2. The human version of the enzyme can be referred to as hACE2.
Coronavirus Spreads Quickly and Sometimes Before People Have Symptoms. Researchers found that the average serial interval for the novel coronavirus in China was approximately four days. This also is among the first studies to estimate the rate of asymptomatic transmission. The speed of an epidemic depends on two things -- how many people each case infects and how long it takes for infection between people to spread. The first quantity is called the reproduction number; the second is the serial interval. The short serial interval of COVID-19 means emerging outbreaks will grow quickly and could be difficult to stop. Ebola, with a serial interval of several weeks, is much easier to contain than influenza, with a serial interval of only a few days. Public health responders to Ebola outbreaks have much more time to identify and isolate cases before they infect others. Asymptomatic cases. According to various estimates, between 20 and 45 percent of the people who get COVID-19 — and possibly more, according to a recent study from the Centers for Disease Control and Prevention — sail through a coronavirus infection without realizing they ever had it. No fever or chills. No loss of smell or taste. No breathing difficulties. They don't feel a thing.
Lingering Covid-19 Symptoms Lasting for Over a Month. Anywhere from 10% to 30% of people who get infected with the coronavirus will have persistent symptoms lasting at least one month, according to the Centers for Disease Control and Prevention. Many with long COVID continue to deal with symptoms for many months, even more than a year after the initial infection. One theory some scientists are looking into is viral persistence. The idea is that someone catches the SARS-CoV-2 virus and eventually gets over the initial infection, but it's possible the virus sticks around in some parts of the body, causing the kinds of persistent symptoms seen in long COVID patients. Other viruses are known to linger in parts of the body for months or even years, creating a "viral reservoir" in places where the immune system is not as likely to root it out. Pathogens can hide in tissue and they have a lot of mechanisms to do that. The proteins they create allow them to better burrow into tissue. Some studies suggest the coronavirus remains in parts of the body, including the gut, well after someone has recovered, although this doesn't necessarily mean the person can spread the virus easily. It's possible the virus has triggered autoimmunity in some long COVID patients. This is when a person's own immune system gets confused and attacks tissues and organs in the body. Researchers have found that a coronavirus infection can lead the body to create certain proteins, called autoantibodies, that can end up being harmful. Autoantibodies are seen in many autoimmune diseases. It could be that other viruses people had before getting the coronavirus reemerge during the infection and start to cause problems. These viruses may have been kept in check when the person was healthy, but it's possible that fighting the SARS-CoV-2 virus dysregulates and throws off their immune system. This provides a very good atmosphere for these other viruses to reactivate and potentially infect new nerves, new tissue or the central nervous system, even in the brain. Researchers found that about 36% of those studied still reported COVID-like symptoms three and six months after diagnosis. Most previous studies have estimated lingering post-COVID symptoms in 10% to 30% of patients. Chest/throat pain, abnormal breathing, abdominal symptoms, fatigue, depression, headaches, cognitive dysfunction and muscle pain. Post-viral syndrome, or post-viral fatigue, refers to a sense of tiredness and weakness that lingers after a person has fought off a viral infection.
Brain Fog - Mitochondria - Fatigue - Attention Deficient - Cognitive Impairment
Scientists find immune cell linked to long COVID fatigue and symptoms. Long COVID remains a frustrating medical mystery, affecting up to 1 in 10 people long after the initial infection fades. Now, scientists have uncovered a crucial clue hidden deep within the immune system. By analyzing individual immune cells, they identified a distinct molecular state in key white blood cells—especially common in patients who initially had mild or moderate COVID. Their large-scale data analysis pointed to a distinct molecular state in a type of white blood cell known as CD14+ monocytes, which play a key role in immune defense.
COVID-19 and Vagus Nerve Inflammation contributes to Dysautonomia. Dysautonomia is a broad term for disorders of the autonomic nervous system, which controls involuntary functions like heart rate, blood pressure, digestion, and temperature regulation. It causes chronic, often debilitating symptoms such as dizziness, fainting, fatigue , and tachycardia. While no cure exists for some forms, management involves lifestyle adjustments and medications. Vagus Nerve and Covid.
Researchers discover key social factors that triple long COVID risk. People with financial and social hardships are up to three times more likely to develop long COVID, researchers find. New research led by Mass General Brigham reveals that people facing social challenges—like food insecurity, financial strain, and limited healthcare access—are two to three times more likely to develop long COVID.
Scientists finally reveal what’s behind long COVID’s mysterious brain fog. Researchers in Japan have pinpointed a biological cause of Long COVID brain fog using advanced PET brain imaging. They discovered widespread increases in AMPA receptor density linked to cognitive impairment and inflammation. The findings confirm brain fog as a measurable, biological condition and reveal new targets for treatment. This could open the door to effective diagnostics and therapies.
Ultra-powered MRI scans show damage to brain's 'control center' is behind long-lasting COVID-19 symptoms. Damage to the brainstem -- the brain's 'control center' -- is behind long-lasting physical and psychiatric effects of severe Covid-19 infection, a study suggests.
Individuals with long COVID face significantly higher rates of gut-brain interaction disorders, alongside worse mental health and quality of life. A new global study reveals a striking post-pandemic surge in gut-brain disorders like IBS and functional dyspepsia. Researchers compared data from 2017 and 2023 and discovered sharp increases—IBS up 28% and dyspepsia nearly 44%. Those suffering from long COVID were especially vulnerable, reporting more anxiety, depression, and worse quality of life. These findings spotlight the urgent need for deeper investigation into the gut-brain axis and revised care models in a post-COVID world.
Long covid could cost the economy billions every year. Working days lost to long covid could be costing the economy billions of pounds every year as patients struggle to cope with symptoms and return to work, finds a new study.
If you pretend that you are infected, and you always wear a mask and wash your hands, and you also avoid non-mask people, then the virus could be within a controllable level within two months. Imagine that, at this instant, you are exposed to and infected with the coronavirus. You now have COVID-19—it is day zero—but it is impossible for you or anyone else to know it. In the following days, the virus will silently propagate in your body, hijacking your cells and making millions of copies of itself. Around day three of your infection, there might be enough of the virus in your nasal passages and saliva that a sample of either would test positive via PCR. Soon, your respiratory system will be so crowded with the virus that you will become contagious, spraying the virus into the air whenever you talk or yell. But you likely will not think yourself sick until around day five, when you start to develop symptoms, such as a fever, dry cough, or lost sense of smell. For the next few days, you will be at your most infectious.
Coronavirus disease 2019 (COVID-19) is stable for several hours to days in aerosols and on surfaces. Scientists found that severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) was detectable in aerosols for up to three hours, up to four hours on copper, up to 24 hours on cardboard and up to two to three days on plastic and stainless steel.
How do I know if I'm Infected?
 COVID-19 Testing for the respiratory illness coronavirus disease 2019
(COVID-19) and the associated SARS-CoV-2 virus is possible with two main
methods:
Molecular Recognition and
Serology
Testing. Molecular methods leverage
polymerase chain reaction (PCR)
along with nucleic acid tests, and other advanced analytical techniques,
to detect the genetic material of the virus using real-time reverse
transcription polymerase chain reaction for diagnostic purposes.
Serology
testing, leverages
ELISA
antibody test kits to detect the presence of antibodies produced by the
host immune system against the virus. Typically two ELISA tests against
two different proteins produced by the virus on between 2 and 4 samples
taken from sputum and
swabs taken nasally and from the mouth. If
either test is positive, a microneutralization assay test is performed to
confirm the positive result. The microneutralization assay is highly
specific, but significantly more labor and time intensive. Since
antibodies continue to circulate even after the infection is cleared,
serology tests continue to be positive for individuals who have been
previously exposed and developed an immune response, which means a
positive test may not indicate an active infection. Serology
antibody
testing is being used both for surveillance and investigational purposes
including, in China, confirmation of recovery, only while the molecular
test methodologies are used to diagnosis active infections. According to
news reports, diagnostic tests developed by the
Centers for Disease Control and Prevention were sent out by early
February 2020 to public health labs in the
U.S. Days later, however, labs were reporting back that the tests weren’t
working due to a manufacturing defect. The defective tests, coupled with
regulatory red tape that prevented state laboratories from using their own
tests, caused further delay.
Testing for COVID-19 (CDC). The South Korean company
Kogenebiotech developed a clinical grade,
PCR based SARS-CoV-2 detection
kit (PowerChek Coronavirus) on 28 January 2020. It looks for the "E" gene
shared by all beta coronaviruses, and the RdRp gene specific to
SARS-CoV-2. Other companies in the country, such as Solgent and Seegene,
also developed versions of clinical grade detection kits, named DiaPlexQ
and Allplex 2019-nCoV Assay, respectively, in February 2020. In China, BGI
Group was one of the first companies to receive emergency use approval
from China's National Medical Products Administration for a PCR-based
SARS-CoV-2 detection kit. In the United States, the Centers for Disease
Control and Prevention (CDC) is distributing its 2019-Novel Coronavirus
(2019-nCoV) Real-Time RT-PCR Diagnostic Panel to public health labs
through the International Reagent Resource. One of three genetic tests in
older versions of the test kits caused inconclusive results due to faulty
reagents, and a bottleneck of testing at the CDC in Atlanta; this resulted
in an average of fewer than 100 samples a day being successfully processed
throughout the whole of February 2020. Tests using two components were not
determined to be reliable until 28 February 2020, and it was not until
then that state and local laboratories were permitted to begin testing.
The test was approved by the Food and Drug Administration under an
Emergency Use Authorization.
False-Negative COVID-19 test results may lead to False Sense of Security
- Laboratory Testing
(screening).
COVID-19 Testing for the respiratory illness coronavirus disease 2019
(COVID-19) and the associated SARS-CoV-2 virus is possible with two main
methods:
Molecular Recognition and
Serology
Testing. Molecular methods leverage
polymerase chain reaction (PCR)
along with nucleic acid tests, and other advanced analytical techniques,
to detect the genetic material of the virus using real-time reverse
transcription polymerase chain reaction for diagnostic purposes.
Serology
testing, leverages
ELISA
antibody test kits to detect the presence of antibodies produced by the
host immune system against the virus. Typically two ELISA tests against
two different proteins produced by the virus on between 2 and 4 samples
taken from sputum and
swabs taken nasally and from the mouth. If
either test is positive, a microneutralization assay test is performed to
confirm the positive result. The microneutralization assay is highly
specific, but significantly more labor and time intensive. Since
antibodies continue to circulate even after the infection is cleared,
serology tests continue to be positive for individuals who have been
previously exposed and developed an immune response, which means a
positive test may not indicate an active infection. Serology
antibody
testing is being used both for surveillance and investigational purposes
including, in China, confirmation of recovery, only while the molecular
test methodologies are used to diagnosis active infections. According to
news reports, diagnostic tests developed by the
Centers for Disease Control and Prevention were sent out by early
February 2020 to public health labs in the
U.S. Days later, however, labs were reporting back that the tests weren’t
working due to a manufacturing defect. The defective tests, coupled with
regulatory red tape that prevented state laboratories from using their own
tests, caused further delay.
Testing for COVID-19 (CDC). The South Korean company
Kogenebiotech developed a clinical grade,
PCR based SARS-CoV-2 detection
kit (PowerChek Coronavirus) on 28 January 2020. It looks for the "E" gene
shared by all beta coronaviruses, and the RdRp gene specific to
SARS-CoV-2. Other companies in the country, such as Solgent and Seegene,
also developed versions of clinical grade detection kits, named DiaPlexQ
and Allplex 2019-nCoV Assay, respectively, in February 2020. In China, BGI
Group was one of the first companies to receive emergency use approval
from China's National Medical Products Administration for a PCR-based
SARS-CoV-2 detection kit. In the United States, the Centers for Disease
Control and Prevention (CDC) is distributing its 2019-Novel Coronavirus
(2019-nCoV) Real-Time RT-PCR Diagnostic Panel to public health labs
through the International Reagent Resource. One of three genetic tests in
older versions of the test kits caused inconclusive results due to faulty
reagents, and a bottleneck of testing at the CDC in Atlanta; this resulted
in an average of fewer than 100 samples a day being successfully processed
throughout the whole of February 2020. Tests using two components were not
determined to be reliable until 28 February 2020, and it was not until
then that state and local laboratories were permitted to begin testing.
The test was approved by the Food and Drug Administration under an
Emergency Use Authorization.
False-Negative COVID-19 test results may lead to False Sense of Security
- Laboratory Testing
(screening).U.S. Coronavirus Testing Still Falls Short - Test Types (pdf) - Will the COVID Swab Touch the Brain (youtube)
Diagnostic Biosensor quickly detects SARS-CoV-2 from nasopharyngeal swabs. Researchers have developed a field-effect transistor-based biosensor that detects SARS-CoV-2 in nasopharyngeal swabs from patients with COVID-19, in less than one minute.
Reverse Transcription Polymerase Chain Reaction is a laboratory technique combining reverse transcription of RNA into DNA (in this context called complementary DNA or cDNA) and amplification of specific DNA targets using polymerase chain reaction (PCR). It is primarily used to measure the amount of a specific RNA. This is achieved by monitoring the amplification reaction using fluorescence, a technique called real-time PCR or quantitative PCR (qPCR). Combined RT-PCR and qPCR are routinely used for analysis of gene expression and quantification of viral RNA in research and clinical settings. The close association between RT-PCR and qPCR has led to metonymic use of the term qPCR to mean RT-PCR. Such use may be confusing, as RT-PCR can be used without qPCR, for example to enable molecular cloning, sequencing or simple detection of RNA. Conversely, qPCR may be used without RT-PCR, for example to quantify the copy number of a specific piece of DNA.
Phylogenetic Analysis and Structural Modeling of SARS-CoV-2 Spike Protein Reveals an Evolutionary Distinct and Proteolytically Sensitive Activation Loop.
Unique and Conserved Features of Genome and Proteome of SARS-coronavirus, an Early Split-off From the Coronavirus Group 2 Lineage.
Molnupiravir is sold under the brand name Lagevrio, which is an antiviral medication that inhibits the replication of certain RNA viruses, and is used to treat COVID-19 in those infected by SARS-CoV-2. Molnupiravir is a prodrug of the synthetic nucleoside derivative N4-hydroxycytidine (also called EIDD-1931), and exerts its antiviral action through introduction of copying errors during viral RNA replication.
PF-07321332 or Paxlovid or Ritonavir was found to reduce the risk of hospitalization or death by 89% compared to placebo in non-hospitalized. PF-07321332 is an antiviral drug developed by Pfizer which acts as an orally active 3CL protease inhibitor. It is a covalent inhibitor, binding directly to the catalytic cysteine (Cys145) residue of the enzyme. As Paxlovid, it is in phase 3 trials for the treatment of COVID-19 in combination with ritonavir. In this combination, ritonavir serves to slow down metabolism of PF-07321332 by cytochrome enzymes to maintain higher circulating concentrations of the main drug. In November 2021, Pfizer announced positive phase 2/3 results, including 89% reduction in hospitalizations when given within three days after symptom onset. Despite not being fully approved yet in either country, The UK has begun stockpiling PF-07321332, and Australia has preordered 500,000 courses of the drug.
Convalescent Plasma refers to anyone recovering from a disease. Plasma is the yellow, liquid part of blood that contains antibodies. People who have fully recovered from COVID-19 for at least two weeks are encouraged to consider donating plasma, which may help save the lives of other patients. COVID-19 convalescent plasma must only be collected from recovered individuals if they are eligible to donate blood.
BioFire System Panels test for viruses, bacteria, parasites, yeast, and antimicrobial resistance genes. Whether you're trying to determine optimal therapy for a septic patient or pinpoint which respiratory pathogen is making a young child sick, the BioFire System can provide definitive answers—fast.
Dogs can sniff out coronavirus with impressive accuracy. In a proof-of-concept study, dogs identified positive samples with 96 percent accuracy. The team found that after three weeks of training all nine dogs were able to readily identify SARS-CoV-2 positive samples, with 96% accuracy on average. Their sensitivity, or ability to avoid false negatives, however, was lower, in part, the researchers believe, because of the stringent criteria of the study: If the dogs walked by a port containing a positive sample even once without responding, that was labeled a "miss." The researchers ran into many complicating factors in their study, such as the tendency of the dogs to discriminate between the actual patients, rather than between their SARS-CoV-2 infection status. The dogs were also thrown off by a sample from a patient that tested negative for SARS-CoV-2 but who had recently recovered from COVID-19.
Levels of SARS-CoV-2 RNA in sewage rose with COVID-19 cases in Dutch cities. Scientists have detected RNA from the new coronavirus, SARS-CoV-2, in the feces of people with COVID-19. So it stands to reason that the viral RNA could end up in city sewage, where it could be used to monitor prevalence of the disease. Although infectious SARS-CoV-2 has been detected in stool samples, the virus spreads primarily through respiratory droplets when an infected person coughs, sneezes, laughs, speaks or breathes, according to recent studies.
Remdesivir is an antiviral medication developed by the American biopharmaceutical company Gilead Sciences. It is a nucleotide analog, specifically an adenosine analogue, which inserts into viral RNA chains, causing their premature termination. It is being studied as a possible post-infection treatment for COVID-19 (caused by an RNA virus) and on 29 April 2020, the US National Institute of Allergy and Infectious Diseases announced the preliminary results of a study showing remdesivir reduced the time to recovery for hospitalized patients with advanced COVID-19 and lung involvement. Remdesivir was originally developed to treat Ebola virus disease (also caused by an RNA virus).
Patients showing up at hospitals with serious cardiovascular emergencies such as strokes and heart attacks has shrunk dramatically. We normally see 100 patients a day, and then you know, overnight, we were down to 30 or 40. Lack of Pollution - Lack of Stress from Commuting.
What do the Coronavirus Numbers Really Mean? The U.S. data on coronavirus infections are deeply flawed, the quantification of the outbreak obscures more than it illuminates. How the data on coronavirus is presented and discussed is a serious problem. Extremely limited testing capacity of the U.S., combined with restrictive testing criteria, has curtailed the number of people who should be tested. How dramatic is the undercount? Knowing the actual cases is only the number that have been tested, and most people test negative than positive, and some tests are inaccurate. Increasing numbers of people being infected is not being clearly defined. Is it from more people being tested or from more people getting infected? Or a little of both? How many false-negative test results were there for the coronavirus? You just can't give a number, you have to give a warning or a brief description about how the data was taken and how it should not be interpreted. You just can't give a word without a definition. People need to agree on the definitions of words so that they can effectively communicate. And people need to understand how information should be interpreted and how it should not be interpreted. People can be easily mislead. Like with nutritional values on food labels being based on a serving amount instead of being based on eating the whole package. A possible infected person under investigation can mean different things. A confirmed positive is a person who has been found positive by a state lab that had that test confirmed by the CDC. A presumptive positive is a person who has been found positive only in state testing. Understanding the Coronavirus Numbers.
Preventing Spread of SARS Coronavirus-2 in Humans. Infection researchers identify potential drug. Infection biologists have investigated how the novel coronavirus SARS-CoV-2 penetrates cells. They have identified a cellular enzyme that is essential for viral entry into lung cells: the protease TMPRSS2. A clinically proven drug known to be active against TMPRSS2 was found to block SARS-CoV-2 infection and might constitute a novel treatment option.
Coronavirus primarily infects the upper respiratory and gastrointestinal tract of mammals and birds. Seven different currently known strains of coronaviruses infect humans. Coronaviruses are believed to cause a significant percentage of all common colds in human adults and children. Coronaviruses cause colds with major symptoms, e.g. fever, throat congestion and adenoids, in humans primarily in the winter and early spring seasons. Coronaviruses can cause pneumonia, either direct viral pneumonia or a secondary bacterial pneumonia, and bronchitis, either direct viral bronchitis or a secondary bacterial bronchitis. Coronaviruses in Humans and Animals.
How the SARS-CoV-2 virus hijacks and rapidly causes damage to human lung cells. Researchers have identified host proteins and pathways in lung cells whose levels change upon infection by the SARS-CoV-2, providing insights into disease pathology and new therapeutic targets to block COVID-19. They found a crucial type of protein modification called "phosphorylation" becomes aberrant in these infected lung cells. The researchers examined lung alveolar cells from one to 24 hours after infection with SARS-CoV-2 to understand what changes occur in lung cells immediately (at one, three and six hours after infection by SARS-CoV-2) and what changes occur later (at 24 hours after infection).
Why COVID-19 is hitting us now — and how to prepare for the next outbreak (video and text) - Coronaviruses are a specific subset of virus, and they have some unique characteristics as viruses. They use RNA instead of DNA as their genetic material, and they're covered in spikes on the surface of the virus. They use those spikes to invade cells. Those spikes are the corona in coronavirus. COVID-19 is known as a novel coronavirus because, until December, we'd only heard of six coronaviruses. COVID-19 is the seventh. It's new to us. It just had its gene sequencing, it just got its name. That's why it's novel. If you remember SARS, Severe Acute Respiratory Syndrome, or MERS, Middle Eastern Respiratory Syndrome, those were coronaviruses. And they're both called respiratory syndromes, because that's what coronaviruses do. Coronaviruses are zoonotic, which means that they transmit from animals to people. Some coronaviruses, like COVID-19, also transmit person to person. The person-to-person ones travel faster and travel farther, just like COVID-19. Zoonotic illnesses are really hard to get rid of, because they have an animal reservoir. One example is avian influenza, where we can abolish it in farmed animals, in turkeys, in ducks, but it keeps coming back every year because it's brought to us by wild birds. You don't hear a lot about it because avian influenza doesn't transmit person-to-person, but we have outbreaks in poultry farms every year all over the world. COVID-19 most likely skipped from animals into people at a wild animal market in Wuhan, China. This is not the last major outbreak we're ever going to see. There's going to be more outbreaks, and there's going to be more epidemics. That's not a maybe. That's a given.
May 5th, more than 9,000 U.S. health-care workers have contracted the new coronavirus and nearly three-quarters of them are women.
Governments knew for years that an outbreak was coming
The Whitehouse was warned and aware of the threat and vulnerability of the Coronavirus.
2017 - The Department of Defense and the Pentagon warned the White House about a shortage of ventilators, face masks, and hospital beds—but the Trump administration did nothing. The Pentagon was aware of the likelihood of a pandemic brought on by a novel coronavirus years ago. Department of Defense Implementation Plan for Pandemic Influenza (August 2006).
In the Spring of 2017, the Trump administration formally stripped OSHA's airborne infectious disease rule from the regulatory agenda. When President Trump took office in 2017, his team stopped work on new federal regulations that would have forced the health care industry to prepare for an airborne infectious disease pandemic such as COVID-19. That decision is documented in federal records. If that rule had gone into effect, then every hospital, every nursing home would essentially have to have a plan where they made sure they had enough respirators and they were prepared for this sort of pandemic. There are still no specific federal regulations protecting health care workers from deadly airborne pathogens such as influenza, tuberculosis or the coronavirus. Studies conducted after the H1N1 crisis found voluntary federal safety guidelines designed to limit the spread of airborne pathogens in medical facilities often weren't being followed. There were also shortages of personal protective equipment. The federal government reports that at least 43,000 front-line health care workers have gotten sick, many infected, while caring for COVID-19 patients in facilities where personal protective equipment was being rationed.
2019 - Intelligence communication intercepts and overhead images showed an increase of activity at health facilities. The intelligence was distributed to some federal public health officials in the form of a "situation report" in late November. But there was no assessment that a lethal global outbreak was brewing at that time, a defense official said. But the current and former officials told NBC News that while no formal assessment was produced in November — and hence no "intelligence product," in the jargon of the spy agencies — there was intelligence that caught the attention of public health analysts and fueled formal assessments that were written in December. That material and other information, including some from news and social media reports, ultimately found its way into President Donald Trump's intelligence briefing book in January. It is unknown whether he read the information. Even after public health authorities began sounding the alarm in January, the U.S. took few steps to ready itself for a pandemic. There was no effort to boost national stockpiles of medical equipment or encourage social distancing, for example. While Trump touts his decision to stop flights from China coming to the U.S. on Jan. 31, about 381,000 people had flown from China to the U.S. in January, according to an analysis by The New York Times. In the U.S., the Centers for Disease Control and Prevention warned Americans on Jan. 6 to take precautions if they were traveling to China. The next day, the CDC's Emergency Operation Center activated a COVID-19 Incident Management System, an emergency management tool used to direct operations, deliver resources and share information. It's sad that America has an ignorant leader that does not respond quick enough or listen to advice. But instead watches thousands of people die and millions of people lose their jobs, and then takes relief funds for people in need to enrich himself and also gives money to his scumbag criminal friends who will use it in devious ways to undermine democracy. So you don't have to engineer new weapons, all you have to do is just use the weapons you have to mass murder people and steal their money, the republican way.
Novel coronavirus circulated undetected months before first COVID-19 cases in Wuhan, China. Study dates emergence to as early as October 2019; Simulations suggest in most cases zoonotic viruses die out naturally before causing a pandemic. Using molecular dating tools and epidemiological simulations, researchers estimate that the SARS-CoV-2 virus likely circulated undetected for two months before the first human cases of COVID-19 were described in Wuhan, China in late-December 2019. Regional newspaper reports suggest COVID-19 diagnoses in Hubei date back to at least November 17, 2019, suggesting the virus was already actively circulating when Chinese authorities enacted public health measures. In the new study, researchers used molecular clock evolutionary analyses to try to home in on when the first, or index, case of SARS-CoV-2 occurred. "Molecular clock" is a term for a technique that uses the mutation rate of genes to deduce when two or more life forms diverged -- in this case, when the common ancestor of all variants of SARS-CoV-2 existed, estimated in this study to as early as mid-November 2019.
The First Confirmed Case of Coronavirus in the United States was announced by the state of Washington on January 21, 2020. Washington made the first announcement of a death from the disease in the U.S. on February 29 and later announced that two deaths there on February 26 was also due to COVID-19. U.S. Lags in Coronavirus Testing After Slow Response to Outbreak. You could easily say that China under estimated the seriousness of the virus in early January, that happened right before one of the worlds most busiest travel seasons. But what are the excuses for all the other countries who also under estimated the virus? China went into lockdown on January 23rd, 2020.
Nearly 8 million kids lost a parent or primary caregiver to the pandemic. A new international study estimates that from January 1, 2020, to May, 1, 2022, nearly 8 million kids age 18 and under lost a parent or primary caregiver to a pandemic-related cause. When the researchers included the deaths of secondary caregivers like grandparents or other older relatives, the number of kids affected rose to 10.5 million. Global Orphanhood Associated with COVID-19.
Mission: Impossible 2 is a 2000 action spy film where bio-chemical expert Dr. Vladimir Nekhorvich warns that his employer at Biocyte Pharmaceuticals forced him to develop a biological weapon to profit from the cure. He arranges to meet with Ethan to deliver the chimeric virus, which is a virus that contains genetic material derived from two or more distinct viruses. The remedy for the chimera virus is Bellerophon.
No Time to Die is a film that started development in 2016. The principal photography took place from April to October 2019. The film is about Project Heracles, a bioweapon containing nanobots that infect like a virus upon touch and are coded to an individual's DNA, rendering it lethal to the target and their relatives but harmless to others. The spy film was released in 2021.
There are many movies about viruses being used as weapons. So you have to wonder, where do people get their ideas from? Inferno is a 2016 American action mystery thriller film where people have to stop a madman from unleashing a virus that could wipe out half of the world's population.
COVID-19 Coronavirus Epidemic has a Natural Origin. The novel SARS-CoV-2 coronavirus that emerged in the city of Wuhan, China, last year and has since caused a large scale COVID-19 epidemic and spread to more than 70 other countries is the product of natural evolution, according to findings published today in the journal Nature Medicine. The analysis of public genome sequence data from SARS-CoV-2 and related viruses found no evidence that the virus was made in a laboratory or otherwise engineered. Coronaviruses are a large family of viruses that can cause illnesses ranging widely in severity. The first known severe illness caused by a coronavirus emerged with the 2003 Severe Acute Respiratory Syndrome (SARS) epidemic in China. A second outbreak of severe illness began in 2012 in Saudi Arabia with the Middle East Respiratory Syndrome (MERS). On December 31 2019, Chinese authorities alerted the World Health Organization of an outbreak of a novel strain of coronavirus causing severe illness, which was subsequently named SARS-CoV-2. As of February 20, 2020, nearly 167,500 COVID-19 cases have been documented, although many more mild cases have likely gone undiagnosed. The virus has killed over 6,600 people. Shortly after the epidemic began, Chinese scientists sequenced the genome of SARS-CoV-2 and made the data available to researchers worldwide. The resulting genomic sequence data has shown that Chinese authorities rapidly detected the epidemic and that the number of COVID-19 cases have been increasing because of human to human transmission after a single introduction into the human population. Andersen and collaborators at several other research institutions used this sequencing data to explore the origins and evolution of SARS-CoV-2 by focusing in on several tell-tale features of the virus. The scientists found that the RBD portion of the SARS-CoV-2 spike proteins had evolved to effectively target a molecular feature on the outside of human cells called ACE2, a receptor involved in regulating blood pressure. The SARS-CoV-2 spike protein was so effective at binding the human cells, in fact, that the scientists concluded it was the result of natural selection and not the product of genetic engineering, but that doesn't mean that the virus can not be grown in labs after it's discovered, and that doesn't mean that people would not maliciously spread the virus and then blame it on other people for the problems it caused, or would it stop an idiot from lying to the public about how dangerous the virus is, as well as downplaying the risks so that needed actions are not taken in time, or would it stop an ignorant leader from intentionally ignoring known threats of the virus so that they can use the destruction that it causes to commit more crimes, especially knowing that it would hurt minorities more than white people. And it would not stop criminals from profiting from the problems that the virus caused, or would it stop morons from decreasing funding for needed research and emergency response and preparedness systems, so they can use their own criminal negligence as another way to profit from the chaos and exploit people in need, the republican way. White House adviser to 60 Minutes: Show me your pandemic story (youtube) - 60 Minutes opens the archive on previous stories on U.S. pandemic preparedness after being challenged by White House trade adviser Peter Navarro, who is now confirmed to be an ignorant moron and a criminal. The Trump administration paid $55 million for N95 masks to a bankrupt company Panthera Worldwide LLC, which the company never manufactured. The company has had zero employees since May 2018. Panthera, which describes itself as a tactical training company for the US military and other government agencies, has no record of producing medical supplies or equipment. And at the same time delay funding for people and business in need, while big corporations get millions and banks collect large fees.
Other countries did a lot better than America
When responding to the Covid19 Virus and controlling the spread of the Covid19 Virus, other countries did a lot better. We are learning some extremely important lessons from the covid-19 virus, but not everyone is learning these lessons, so we are wasting an opportunity to protect ourselves and protect future generations. This means that our vulnerabilities are still present. Why The United States Is Experiencing Mass Layoffs But Europe Isn't. South Korea fought and controlled this virus without using a vaccine or a pill. How New Zealand got its Coronavirus Cases down to zero in seven weeks. Jordan's Prime Minister Says His Country Contained COVID-19 By 'Helping The Weakest'. Taiwan and Thailand also had effective responses to the virus. This clearly shows the power of people. When people work together we can solve problems and survive difficult situations. This experience must not be forgotten. Just like our immune cells, we want our immune system to never forget this virus. This is why communication and accurate information is so extremely valuable. When people are not informed or inoculated with knowledge, then people will not be able to work together effectively or efficiently, or will people be able to defend themselves against threats or viruses, which is why the virus was able to spread so quickly. Lack of communication and lack of information is deadly and costly, as clearly seen. Some countries are using different methods and plans to deal with this virus, and we will see what works and what does not work. Germany in mid-January, long before most Germans had given the virus much thought, Charité hospital in Berlin had already developed a test and posted the formula online. By the time Germany recorded its first case of Covid-19 in February, laboratories across the country had built up a stock of test kits to do an extremely large number of lab diagnoses. Germany is conducting around 350,000 coronavirus tests a week, far more than any other European country. Early and widespread testing has allowed the authorities to slow the spread of the pandemic by isolating known cases while they are infectious. It has also enabled lifesaving treatment to be administered in a more timely way, thus Germany had fewer deaths. When I have an early diagnosis and can treat patients early, for example put them on a ventilator before they deteriorate, the chance of survival is much higher. To streamline the procedure, some hospitals have started doing block tests, using the swabs of 10 employees, and following up with individual tests only if there is a positive result. At the end of April, health authorities also plan to roll out a large-scale antibody study, testing random samples of 100,000 people across Germany every week to gauge where immunity is building up. Free Testing. One key to ensuring broad-based testing is that patients pay nothing for it. A young person with no health insurance and an itchy throat is unlikely to go to the doctor and therefore risks infecting more people. United States, testing is largely limited to the sickest patients, so the man probably would have been refused a test. In January, Germany had some 28,000 intensive care beds equipped with ventilators, or 34 per 100,000 people. By comparison, that rate is 12 in Italy and 7 in the Netherlands. In April, there are 40,000 intensive care beds available in Germany. The time it takes for the number of infections to double has slowed to about nine days. If it slows a little more, to between 12 and 14 days, the models suggest that triage could be avoided. Germany has a universal multi-payer health care system paid for by a combination of statutory health insurance, ensuring free healthcare for all. In addition, you can also take out private health insurance. Germany, on the other hand, spent $5, 848 on health care for each of its citizens. Despite spending less per capita, Germany still manages to cover 100% of its population. In the United States, about 8.8% of the population remains uninsured, which equates to about 28 million people. The United States has no single nationwide system of health insurance.
Trump was incompetent and criminally negligent and corrupt in his handling of the response to the covid-19 virus. He knew this virus was extremely dangerous and that it would be a threat to the economy and a threat to peoples lives, especially to the lives of minorities, which he has shown several times to be prejudice towards. But trump ignored the facts and played it down so he could politicize the virus and use the damage that the virus caused as another way to divide the country and create turmoil, while at the same time, trying to profit from the virus. This was an ignorant excuse to justify the killing over 700,000 Americans. Trump should go to prison for life, as well as the people who helped influence him to be criminally negligent. Covid-19 was a weapon of mass destruction and a genocide against the vulnerable.
Trump deliberately sabotaged the nation’s response to the pandemic. Interference and undermining the Covid response. To begin with, the White House shut down public briefings by the Centers for Disease Control and Prevention. On Feb. 25, 2020, Nancy Messonnier, the CDC official in charge of respiratory diseases, warned Americans that a pandemic was coming and that they should prepare for school and workplace closures. Trump responded by threatening to fire her. For months thereafter, the White House refused to authorize CDC briefings. In transcribed interviews, CDC officials told the subcommittee that in April 2020, the White House rejected the agency’s request to hold a briefing to present the scientific case for wearing masks. Instead, Trump delivered his own COVID briefing, at which he said of masks: “You don’t have to do it. I’m choosing not to do it.” That statement and others, according to CDC officials who spoke to the subcommittee, gravely undermined the agency’s efforts to control the pandemic. Second, the White House altered CDC guidance to religious congregations, deleting recommendations to wear masks and take other precautions. In a May 2020 email obtained by the committee, Jay Butler, a CDC official, reported that the White House had stripped out crucial elements of the guidance. “All references to face coverings are missing in the WH version,” Butler wrote. In addition, he noted, “References to considering virtual events are absent from the WH version.” Third, the administration tried to limit COVID testing in order to hide the extent of the pandemic and keep businesses open. At a political rally on June 20, 2020, Trump said he had told “my people” to “slow the testing down.” He later claimed that he was half-joking, but the report found evidence that in subsequent months, Trump’s people tried to do exactly as he had instructed. On Aug. 24, 2020, the administration changed CDC’s guidance to say that most people who didn’t have COVID symptoms shouldn’t get tested, even if they had been exposed to a known carrier. An Aug. 27, 2020, email from Paul Alexander, an advisor to the Department of Health and Human Services, explained that the guidance had been altered because tests of asymptomatic people, if they came out positive, would end up “preventing the workforce from working,” and “widespread testing of schools and colleges/universities” would “not allow them to optimally re-open.” Republicans are attacking the White House with a new talking point: More Americans have died of COVID-19 under Joe Biden’s presidency, they point out, than under Donald Trump’s. Mathematically, that’s true. When Trump left office, the U.S. death toll was around 400,000 people; now it’s above 800,000. The comparison is misleading for many reasons, however. One is that Biden has been dealt two new variants, Delta and Omicron, that spread more aggressively than the original Wuhan virus did. Furthermore, while Biden has begged Americans to get vaccinated, Republican politicians have constantly undermined him by banning or blocking vaccine mandates. But there’s another crucial difference between the two administrations, and it’s outlined in a new report from the House Select Subcommittee on the Coronavirus Crisis. Trump’s administration, unlike Biden’s, deliberately sabotaged the nation’s response to the pandemic. The report, issued on Friday, documents multiple channels of interference by Trump and his underlings. To begin with, the White House shut down public briefings by the Centers for Disease Control and Prevention. On Feb. 25, 2020, Nancy Messonnier, the CDC official in charge of respiratory diseases, warned Americans that a pandemic was coming and that they should prepare for school and workplace closures. Trump responded by threatening to fire her. For months thereafter, the White House refused to authorize CDC briefings. In transcribed interviews, CDC officials told the subcommittee that in April 2020, the White House rejected the agency’s request to hold a briefing to present the scientific case for wearing masks. Instead, Trump delivered his own COVID briefing, at which he said of masks: “You don’t have to do it. I’m choosing not to do it.” That statement and others, according to CDC officials who spoke to the subcommittee, gravely undermined the agency’s efforts to control the pandemic. Second, the White House altered CDC guidance to religious congregations, deleting recommendations to wear masks and take other precautions. In a May 2020 email obtained by the committee, Jay Butler, a CDC official, reported that the White House had stripped out crucial elements of the guidance. “All references to face coverings are missing in the WH version,” Butler wrote. In addition, he noted, “References to considering virtual events are absent from the WH version.” Third, the administration tried to limit COVID testing in order to hide the extent of the pandemic and keep businesses open. At a political rally on June 20, 2020, Trump said he had told “my people” to “slow the testing down.” He later claimed that he was half-joking, but the report found evidence that in subsequent months, Trump’s people tried to do exactly as he had instructed. On Aug. 24, 2020, the administration changed CDC’s guidance to say that most people who didn’t have COVID symptoms shouldn’t get tested, even if they had been exposed to a known carrier. An Aug. 27, 2020, email from Paul Alexander, an advisor to the Department of Health and Human Services, explained that the guidance had been altered because tests of asymptomatic people, if they came out positive, would end up “preventing the workforce from working,” and “widespread testing of schools and colleges/universities” would “not allow them to optimally re-open.” Fourth, from September 2020 to January 2021, the White House ignored urgent entreaties from its COVID task force coordinator, Dr. Deborah Birx. She told the subcommittee that during these months, she had repeatedly circulated internal reports pleading for more promotion of mask use, better access to monoclonal infusion and other therapies, immediate provision of vaccines to elderly people based on “compassionate use,” and “aggressive testing” to find and alert carriers before they infected others. By comparing states that implemented such measures to those that didn’t, Birx estimated that if her pleas had been heeded, fatalities could have been reduced by 30 percent to 40 percent. The report also details other ways in which the White House impeded or corrupted the public health response. Trump’s political appointees tried to pressure the Food and Drug Administration to authorize hydroxychloroquine and other ineffective therapies. And early in the pandemic, when Americans faced a dangerous shortage of masks, a White House adviser, Steven Hatfill, rebuffed opportunities to get them overseas. In an email on March 27, 2020, a volunteer on the administration’s pandemic response team asked Hatfill: “Are you interested in talking to people who have or say they have large numbers (hundreds of thousands or millions) of N95 or KN95 mask available from abroad?” Hatfill wrote back: “Nothing that is not US based.” Two weeks later, the volunteer offered to connect Hatfill to a “US based sewing company that has manufacturing capacity in Mexico and Central America.” Hatfield replied that masks had to be “US made.” Trump was directly involved in much of the administration’s malfeasance, as investigations by news organizations have previously revealed. But the subcommittee report links to emails, transcripts, and other documents that show how the president’s anti-mask, anti-testing rhetoric was translated into policy and magnified the death toll. There’s no evidence of such corruption in the Biden administration. On the contrary, Biden has implored the public to get vaccinated or mask up, while Republican politicians have undermined him by prohibiting mask mandates and suing to block his vaccine mandates. So let’s be clear about why so many Americans have needlessly died in the past two years. One party has been pressing the brakes on COVID-19. The other has been pressing the accelerator.
Haiti has one of the lowest death rates from COVID-19 in the world. As of the end of April 2021, only 254 deaths were attributed to COVID-19 in Haiti over the course of the entire pandemic. The Caribbean nation, which often struggles with infectious diseases, has a COVID-19 death rate of just 22 per million. In the U.S. the COVID-19 death rate is 1,800 per million, and in parts of Europe. the fatality rate is approaching 3,000 deaths per million. Last June, the country of 11 million was hit with a significant wave of infections. Hospital wards filled with COVID-19 patients. At the time, the country only had two places that could test for the virus, so the actual number of infections is unknown. Now, testing is far more available, but Pape says very few cases are detected each day. The pandemic may have had less of an impact in Haiti, she says, because it's a young country. The average age is 23. COVID-19 infections tend to be less severe in younger people. It's also possible, she says, that a significant number of people were infected by the virus last summer, showed no symptoms and built up immunity. Also houses tend to be open with plenty of ventilation – air flow can knock the pathogen out of the picture.
Difference in Infection Rates for mostly Republican States vs. mostly Democratic States.
Difference in Infection Rates for Vermont when compared to South Dakota.
A new study estimates that the number of people who have died of COVID-19 in the U.S. is more than 900,000, a number 57% higher than official figures. Worldwide, the study's authors say, the COVID-19 death count is nearing 7 million, more than double the reported number of 3.24 million.
Universal Mask Wearing could have saved 130,000 Lives In The U.S., Study Suggests. There will be an estimated 385,611 COVID-19 Deaths based on current projection scenario by February 1, 2021.
Measles
Measles is a highly contagious infectious disease caused by the measles virus. Symptoms usually develop 10–12 days after exposure to an infected person and last 7–10 days. Initial symptoms typically include fever, often greater than 40 °C (104.0 °F), cough, runny nose, and inflamed eyes. Small white spots known as Koplik's spots may form inside the mouth two or three days after the start of symptoms. A red, flat rash which usually starts on the face and then spreads to the rest of the body typically begins three to five days after the start of symptoms. Complications occur in about 30% of cases and may include diarrhea, blindness, inflammation of the brain, and pneumonia, among others. Rubella, which is sometimes called German measles, and roseola are different diseases caused by unrelated viruses. Measles is an airborne disease which spreads easily through the coughs and sneezes of infected people. It may also be spread through contact with saliva or nasal secretions. Nine out of ten people who are not immune and share living space with an infected person will catch it. People are infectious to others from four days before to four days after the start of the rash. Most people do not get the disease more than once. Testing for the measles virus in suspected cases is important for public health efforts. Measles is a highly contagious virus that lives in the nose and throat mucus of an infected person. Measles is so contagious that if one person has it, 90% of the people close to that person who are not immune will also become infected. How do you cure the measles? Use acetaminophen to relieve fever and muscle aches. Rest to help boost your immune system. Drink plenty of fluids (six to eight glasses of water a day). Use humidifier to ease a cough and sore throat. Take vitamin A supplements. Take it easy. Get rest and avoid busy activities. Sip something. Drink plenty of water, fruit juice and herbal tea to replace fluids lost by fever and sweating. Seek respiratory relief. Use a humidifier to relieve a cough and sore throat. Rest your eyes. The first symptoms of a measles infection are usually a hacking cough, runny nose, high fever, and red eyes. The fever and rash slowly go away after a few days. One out of every 1,000 measles cases will develop acute encephalitis, which is an inflammation of the brain tissue. The most common cause is viral infections. In rare cases it can be caused by bacteria or even fungi. Measles spread by coughing and sneezing via close personal contact or direct contact with secretions. The virus remains active and contagious in the air or on infected surfaces for up to 2 hours. It can be transmitted by an infected person from 4 days prior to the onset of the rash to 4 days after the rash erupts. Risk factors for severe measles is Malnutrition. The measles virus resides in the mucus in the nose and throat of infected people. Severe complications from measles can be avoided through supportive care that ensures good nutrition, adequate fluid intake and treatment of dehydration with WHO-recommended oral rehydration solution. This solution replaces fluids and other essential elements that are lost through diarrhea or vomiting. Antibiotics should be prescribed to treat eye and ear infections, and pneumonia. All children diagnosed with measles should receive two doses of vitamin A supplements, given 24 hours apart. This treatment restores low vitamin A levels during measles that occur even in well-nourished children and can help prevent eye damage and blindness. Vitamin A supplements have been shown to reduce the number of deaths from measles by 50%. Investments into vaccine campaigns is not effective enough. You need to invest in educating the public, it's the only proven way for protecting people. The overwhelming majority (more than 95%) of measles deaths occur in countries with low per capita incomes and weak health infrastructures. No specific antiviral treatment exists for measles virus.
Measles Virus is a single-stranded, negative-sense, enveloped (non-segmented) RNA virus of the genus Morbillivirus within the family Paramyxoviridae. Humans are the natural hosts of the virus; no animal reservoirs are known to exist. The measles virus evolved from the formerly widespread rinderpest virus, which infects cattle. Sequence analysis has suggested that the two viruses most probably diverged in the 11th and 12th centuries, though the periods as early as the 5th century fall within the 95% confidence interval of these calculations. Entry. The measles virus has two envelope glycoproteins on the viral surface—hemagglutinin (H) and membrane fusion protein (F). These proteins are responsible for host cell binding and invasion. Three receptors for the H protein have been identified to date: complement regulatory molecule CD46, the signaling lymphocyte activation molecule (SLAM) and the cell adhesion molecule Nectin-4. People who have been vaccinated can still get the measles, but there is only a small chance of this happening. About 3 percent of people who receive two doses of the measles vaccine will get measles if they come in contact with someone who has the virus, according to the CDC. About three out of 100—who get two doses of measles vaccine will still get measles if exposed to the virus. Some people are immune to measles, meaning that their body has already learned how to fight off the virus, and they won’t become sick from it. People can become immune to measles if they’ve already had measles earlier in life, then they are immune and won’t get it again. The only way to tell for sure that a person is protected (immune) is by a blood test. The blood test shows whether the body has antibodies to fight off the virus. Pets do not get infected with or spread the measles virus.
How measles wipes out the body's immune memory. Study details the mechanism and scope of measles-induced immune amnesia in the wake of infection. A new study shows that measles wipes out 20 to 50 percent of antibodies against an array of viruses and bacteria, depleting a child's previous immunity. A measles-ravaged immune system must 'relearn' how to protect the body against infections. The study details the mechanism and scope of this measles-induced 'immune amnesia.' The findings underscore the importance of measles vaccination, suggesting those infected with measles may benefit from booster shots of all previous childhood vaccines.
Respiratory Syncytial Virus are also called human respiratory syncytial virus or hRSV and human orthopneumovirus, which is a very common, contagious virus that causes infections of the respiratory tract. It is a negative-sense, single-stranded RNA virus, and its name is derived from the large cells known as syncytia that form when infected cells fuse together. While RSV is the single most common cause of respiratory hospitalization in infants, reinfection remains common in later life, and it is an important pathogen in all age groups. Infection rates are typically higher during the cold winter months, causing bronchiolitis in infants, common colds in adults, and more serious respiratory illnesses such as pneumonia in the elderly and immunocompromised. RSV is spread through contaminated air droplets and can cause outbreaks both in the community and in hospital settings. Following initial infection via the eyes or nose, the virus will infect the epithelial cells of the upper and lower airway, causing inflammation, cell damage, and airway obstruction. A variety of methods are available for viral detection and diagnosis of RSV including antigen testing, molecular testing, and viral culture. While the main prevention measures include hand washing and avoiding close contact with infected individuals, a prophylactic medication called palivizumab is available to prevent RSV infection in high-risk infants. Currently, there is no vaccine against RSV, although many are under development. Treatment for severe illness is primarily supportive, including oxygen therapy and more advanced breathing support with CPAP or nasal high flow oxygen, as required. In cases of severe respiratory failure, intubation and mechanical ventilation may be required. Ribavirin is the only antiviral medication currently licensed for the treatment of RSV in children, although its use remains controversial.
Monkeypox Virus is part of the same family of viruses as variola virus, the virus that causes smallpox. Monkeypox is a viral zoonosis or a virus transmitted to humans from animals with symptoms similar to those seen in the past in smallpox patients. Monkeypox can spread to anyone through close, personal, often skin-to-skin contact, including: Direct contact with monkeypox rash, scabs, or body fluids from a person with monkeypox. Touching objects, fabrics (clothing, bedding, or towels), and surfaces that have been used by someone with monkeypox. A rash that may be located on or near the genitals (penis, testicles, labia, and vagina) or anus (butthole) but could also be on other areas. On Sept. 22, 2017, an 11-year-old boy had very large lesions affecting his face and all over his body. This was the first known case of the international monkeypox outbreak, currently spreading in 78 countries. The rash looked a bit like chickenpox. But the boy already had chickenpox.
Negative-Strand RNA Viruses or-ssRNA viruses are a group of related viruses that have negative-sense, single-stranded genomes made of ribonucleic acid. They have genomes that act as complementary strands from which messenger RNA (mRNA) is synthesized by the viral enzyme RNA-dependent RNA polymerase (RdRp). During replication of the viral genome, RdRp synthesizes a positive-sense antigenome that it uses as a template to create genomic negative-sense RNA. Negative-strand RNA viruses also share a number of other characteristics: most contain a viral envelope that surrounds the capsid, which encases the viral genome, -ssRNA virus genomes are usually linear, and it is common for their genome to be segmented. Negative-strand RNA viruses constitute the phylum Negarnaviricota, in the kingdom Orthornavirae and realm Riboviria. They are descended from a common ancestor that was a double-stranded RNA (dsRNA) virus, and they are considered to be a sister clade of reoviruses, which are dsRNA viruses. Within the phylum, there are two major branches that form two subphyla: Haploviricotina, whose members are mostly non-segmented and which encode an RdRp that synthesizes caps on mRNA, and Polyploviricotina, whose members are segmented and which encode an RdRp that snatches caps from host mRNAs. A total of six classes in the phylum are recognized. Negative-strand RNA viruses are closely associated with arthropods and can be informally divided between those that are reliant on arthropods for transmission and those that are descended from arthropod viruses but can now replicate in vertebrates without the aid of arthropods. Prominent arthropod-borne -ssRNA viruses include the Rift Valley fever virus and the tomato spotted wilt virus. Notable vertebrate -ssRNA viruses include the Ebola virus, hantaviruses, influenza viruses, the Lassa fever virus, and the rabies virus.
Morbillivirus is a genus of viruses in the order Mononegavirales, in the family Paramyxoviridae. Humans, dogs, cats, cattle, and cetaceans serve as natural hosts. This genus currently included seven species. Diseases in humans associated with viruses classified in this genus include measles: fever, and rash; in animals, they include acute febrile respiratory tract infection.
Paramyxoviridae is a family of viruses in the order Mononegavirales. Vertebrates serve as natural hosts; no known plants serve as vectors. There are currently 49 species in this family, divided among 7 genera. Diseases associated with this negative-sense single-stranded RNA virus family include measles, mumps, and respiratory tract infections.
Sense in molecular biology and genetics, the sense of nucleic acid molecules (often DNA or RNA) is the nature of their roles and their complementary molecules' nucleic acid units' roles in specifying amino acids. Depending on the context within molecular biology, sense may have slightly different meanings. For example, DNA is positive-sense if an RNA version of the same sequence is translated or translatable into protein, negative-sense if not. RNA sense in viruses: In virology, the genome of an RNA virus can be said to be either positive-sense, also known as a "plus-strand", or negative-sense, also known as a "minus-strand". In most cases, the terms sense and strand are used interchangeably, making such terms as positive-strand equivalent to positive-sense, and plus-strand equivalent to plus-sense. Whether a virus genome is positive-sense or negative-sense can be used as a basis for classifying viruses. Positive-sense: (5' to 3') viral RNA signifies that a particular viral RNA sequence may be directly translated into the desired viral proteins. Therefore, in positive-sense RNA viruses, the viral RNA genome can be considered viral mRNA, and can be immediately translated by the host cell. Unlike negative-sense RNA, positive-sense RNA is of the same sense as mRNA. Some viruses (e.g., Coronaviridae) have positive-sense genomes that can act as mRNA and be used directly to synthesize proteins without the help of a complementary RNA intermediate. Because of this, these viruses do not need to have an RNA polymerase packaged into the virion. Negative-sense: (3' to 5') viral RNA is complementary to the viral mRNA and thus from it a positive-sense RNA must be produced by an RNA-dependent RNA polymerase prior to translation. Negative-sense RNA (like DNA) has a nucleotide sequence complementary to the mRNA that it encodes. Like DNA, this RNA cannot be translated into protein directly. Instead, it must first be transcribed into a positive-sense RNA that acts as an mRNA. Some viruses (Influenza, for example) have negative-sense genomes and so must carry an RNA polymerase inside the virion.
Complementarity in molecular biology, complementarity describes a relationship between two structures each following the lock-and-key principle. In nature complementarity is the base principle of DNA replication and transcription as it is a property shared between two DNA or RNA sequences, such that when they are aligned antiparallel to each other, the nucleotide bases at each position in the sequences will be complementary, much like looking in the mirror and seeing the reverse of things. This complementary base pairing allows cells to copy information from one generation to another and even find and repair damage to the information stored in the sequences. The degree of complementarity between two nucleic acid strands may vary, from complete complementarity (each nucleotide is across from its opposite) to no complementarity (each nucleotide is not across from its opposite) and determines the stability of the sequences to be together. Furthermore, various DNA repair functions as well as regulatory functions are based on base pair complementarity. In biotechnology, the principle of base pair complementarity allows the generation of DNA hybrids between RNA and DNA, and opens the door to modern tools such as cDNA libraries. While most complementarity is seen between two separate strings of DNA or RNA, it is also possible for a sequence to have internal complementarity resulting in the sequence binding to itself in a folded configuration.
Agglutination in biology is the clumping of particles. Agglutination is the process that occurs if an antigen is mixed with its corresponding antibody called isoagglutinin. This term is commonly used in blood grouping This occurs in biology in three main examples: The clumping of cells such as bacteria or red blood cells in the presence of an antibody or complement. The antibody or other molecule binds multiple particles and joins them, creating a large complex. This increases the efficacy of microbial elimination by phagocytosis as large clumps of bacteria can be eliminated in one pass, versus the elimination of single microbial antigens. When people are given blood transfusions of the wrong blood group, the antibodies react with the incorrectly transfused blood group and as a result, the erythrocytes clump up and stick together causing them to agglutinate. The coalescing of small particles that are suspended in a solution; these larger masses are then (usually) precipitated.
Nipah virus infection is a viral infection caused by the Nipah virus. Symptoms from infection vary from none to fever, cough, headache, shortness of breath, and confusion. This may worsen into a coma over a day or two, and 50% to 75% of those infected die. Complications can include inflammation of the brain and seizures following recovery. Nipah virus is a bat-borne virus that causes Nipah virus infection in humans and other animals, a disease with a high mortality rate. Numerous disease outbreaks caused by Nipah virus have occurred in South and Southeast Asia. Nipah virus belongs to the genus Henipavirus along with the Hendra virus, which has also caused disease outbreaks. Symptoms include Fever, Headache, Muscle Pain (myalgia), Vomiting and Sore Throat. These symptoms can be followed by more serious conditions including: Dizziness, Drowsiness, Altered Consciousness, Acute Encephalitis, Atypical Pneumonia, Severe Respiratory and Seizures.
Bacteria
Bacteria is a large domain of prokaryotic microorganisms. Typically a few micrometres in length, bacteria have a number of shapes, ranging from spheres to rods and spirals. Bacteria also live in symbiotic and parasitic relationships with plants and animals. Most bacteria have not been characterized, and only about half of the bacterial phyla have species that can be grown in the laboratory. The study of bacteria is known as bacteriology, a branch of microbiology.
Bacterial vs. Viral Infections: How do they differ?
Pathogenic Bacteria are bacteria that can cause infection. Although most bacteria are harmless or often beneficial, some can produce disease.
Cyanobacteria - Bacteria Gas
Gram-Positive Bacteria are bacteria that give a positive result in the Gram stain test, which is traditionally used to quickly classify bacteria into two broad categories according to their cell wall. Gram-Negative Bacteria are a group of bacteria that do not retain the crystal violet stain used in the Gram staining method of bacterial differentiation. They are characterized by their cell envelopes, which are composed of a thin peptidoglycan cell wall sandwiched between an inner cytoplasmic cell membrane and a bacterial outer membrane.
Meningitis is an acute inflammation of the protective membranes covering the brain and spinal cord, known collectively as the meninges. The most common symptoms are fever, headache and neck stiffness. Other symptoms include confusion or altered consciousness, vomiting, and an inability to tolerate light or loud noises. Young children often exhibit only nonspecific symptoms, such as irritability, drowsiness, or poor feeding. If a rash is present, it may indicate a particular cause of meningitis; for instance, meningitis caused by meningococcal bacteria may be accompanied by a characteristic rash. Infections.
Compound from medicinal herb kills brain-eating amoebae in lab studies. Primary amoebic meningoencephalitis or PAM, a deadly disease caused by the 'brain-eating amoeba' Naegleria fowleri, is becoming more common in some areas of the world, and it has no effective treatment. Now, researchers have found that a compound isolated from the leaves of a traditional medicinal plant, Inula viscosa or 'false yellowhead,' kills the amoebae by causing them to commit cell suicide in lab studies, which could lead to new treatments.
Newly discovered virus can kill resistant bacteria. Viruses exist in nature and are the world's most widespread organism. They are everywhere and part of all kinds of microbial cycles and ecosystems. Many viruses are so-called bacteriophages (or phages), meaning that they kill bacteria, and Fyn8 is no exception. It can attack and kill the bacteria Pseudomonas aeruginosa. Pseudomonas aeruginosa is a bacterium found naturally in soil and water. It is normally harmless towards healthy people, but like many other bacteria it has developed resistance to antibiotics and is found in hospitals.
Bacteria's extensive weaponry. A new study tackles the mystery of why bacteria often carry diverse ranges of weapons. The findings show that different weapons are best suited to different competition scenarios. Short-range weapons help bacteria to invade established communities; long-range weapons are useful once established.
Sepsis is a life-threatening condition that arises when the body's response to infection causes injury to its own tissues and organs. Common signs and symptoms include fever, increased heart rate, increased breathing rate, and confusion. There may also be symptoms related to a specific infection, such as a cough with pneumonia, or painful urination with a kidney infection. In the very young, old, and people with a weakened immune system, there may be no symptoms of a specific infection and the body temperature may be low or normal, rather than high. Severe sepsis is sepsis causing poor organ function or insufficient blood flow. Insufficient blood flow may be evident by low blood pressure, high blood lactate, or low urine output. Septic shock is low blood pressure due to sepsis that does not improve after fluid replacement. Sepsis is caused by an inflammatory immune response triggered by an infection. Most commonly, the infection is bacterial, but it may also be fungal, viral, or protozoan. Common locations for the primary infection include the lungs, brain, urinary tract, skin, and abdominal organs. Septic Shock is a serious medical condition that occurs when sepsis, which is organ injury or damage in response to infection, leads to dangerously low blood pressure and abnormalities in cellular metabolism. Sepsis is the presence of pus-forming bacteria or their toxins in the blood or tissues.
Macrophage Nano-Sponges could keep Sepsis in check. Researchers have developed macrophage 'nanosponges' -- nanoparticles cloaked in the cell membranes of macrophages -- that can safely remove sepsis-causing molecules from the bloodstream. Immune System.
Sepsis need not be fatal. Researchers have identified molecular biomarkers, pathways and immune cell dynamics associated with sepsis that could be therapeutically targeted to prevent the condition from leading to death. Sepsis, the body's life-threatening response to infection affecting about 1.7 million adults in the United States each year, can lead to multisystem organ failure with a high mortality rate. No targeted therapeutics against this condition have been developed in the last decades.
Toxic Shock Syndrome is a condition caused by bacterial toxins. Symptoms may include fever, rash, skin peeling, and low blood pressure. There may also be symptoms related to the specific underlying infection such as mastitis, osteomyelitis, necrotising fasciitis, or pneumonia. TSS is caused by bacteria of either the Streptococcus pyogenes or Staphylococcus aureus type. Streptococcal toxic shock syndrome (STSS) is sometimes referred to as toxic shock-like syndrome (TSLS). The underlying mechanism involves the production of superantigens during an invasive streptococcus infection or a localized staphylococcus infection. Risk factors for the staphylococcal type include the use of very absorbent tampons and skin lesions in young children. Diagnosis is typically based on symptoms. Treatment includes antibiotics, incision and drainage of any abscesses, and possibly intravenous immunoglobulin. The need for rapid removal of infected tissue via surgery in those with a streptococcal cause while commonly recommended is poorly supported by the evidence. Some recommend delaying surgical debridement. The overall risk of death in streptococcal disease is about 50% while in staphylococcal disease it is around 5%. Death may occur within 2 days.
Burkholderia Pseudomallei is a Gram-negative, bipolar, aerobic, motile rod-shaped bacterium. It is a soil-dwelling bacterium endemic in tropical and subtropical regions worldwide, particularly in Thailand and northern Australia. It infects humans and animals and causes the disease melioidosis. It is also capable of infecting plants.
Melioidosis is an infectious disease caused by a Gram-negative bacterium, Burkholderia pseudomallei, found in soil and water. It is of public health importance in endemic areas, particularly in northeast Thailand, Vietnam, and northern Australia. It exists in acute and chronic forms. Signs and symptoms may include pain in chest, bones, or joints; cough; skin infections, lung nodules, and pneumonia.
Ancient DNA used to map evolution of fever-causing bacteria. Researchers have analyzed ancient DNA from Borrelia recurrentis, a type of bacteria that causes relapsing fever, pinpointing when it evolved to spread through lice rather than ticks, and how it gained and lost genes in the process.
Scientists discover how potent bacterial toxin kills MRSA bacteria. The lysostaphin is able to increase the number of its molecules bound to the surface of the MRSA cell and this allows the enzyme to 'walk' along the cell walls and cause rapid breakdown.
Methicillin-resistant Staphylococcus aureus or MRSA refers to a group of Gram-positive bacteria that are genetically distinct from other strains of Staphylococcus aureus. MRSA is responsible for several difficult-to-treat infections in humans.
Newly identified bacteria-killing protein needs vitamin A to work. RELMa is the first example of an antimicrobial protein that requires dietary vitamin A for its bacterial killing activity.
Visible light triggers molecular machines to treat infections. Chemists have created light-activated molecular machines and shown they can drill holes through the membranes of gram-negative and gram-positive bacteria, killing them in as little as two minutes. Their study offers a potential new strategy for fighting antibiotic-resistant bacteria, which have no natural defenses against the mechanical invaders.
Certain bacteria can override a defense mechanism of the immune system, so-called programmed cell death, through inhibition of death effector molecules by their outer membranes components. Shigella bacteria, which cause diarrhoea, use lipopolysaccharides (LPS) on their surface to block the effector caspases. Lipopolysaccharides are a component of the bacterial outer membrane. This strategy enables the bacteria to multiply within the cell. Various bacterial pathogens can escape our immune system by staying and multiplying within our body cells (intracellularly). The intracellular propagation of pathogens later leads to cell breakdown and the release of microorganisms that infect neighbouring cells spread and cause tissue damage and infectious disease. However, the body has a response to this bacterial strategy: programmed cell death, or apoptosis, reacts to cellular stress situations during infections and causes quick suicide of the infected cells. Due to this rapid self-destruction programme of our body cells, pathogens cannot multiply - the immune system successfully eliminates them. Scientists have observed in the past that pathogens can effectively block apoptosis, allowing them to reproduce and spread intracellularly. However, the molecular mechanism responsible for how these bacteria 'outsmarted' the immune system was largely unknown. Kashkar lab has now shown that the pathogen that causes shigellosis (Shigella), a typical cause of acute inflammatory diarrhoea, blocks apoptosis by efficiently blocking certain enzymes, so-called caspases, which act as engines that initiate apoptosis. The biologists showed that lipopolysaccharides bind and block the caspase. Bacteria without complete LPS, on the other hand, spark apoptosis, which blocks them from reproducing intracellularly. They are successfully eliminated by the immune system and thus no longer able to cause infectious diseases. Kashkar lab's work has thus deciphered an important bacterial strategy to prevent the rapid death of the host cell and establish a niche to spread.
Study IDs bacterial weapons that could be harnessed to treat human disease. Discovery of ancient immune-fighting machinery paves way toward more 'CRISPR'-like technologies
When it comes to fighting off invaders, bacteria operate in a remarkably similar way to human cells, possessing the same core machinery required to switch immune pathways on and off, according to new research. Proteins called Cap2 and Cap3 (CD-NTase-associated protein 2 and 3) -- which serve, respectively, as on and off switches for the cGAS response.
Scientists test 'smart' red blood cells to deliver antibiotics that target specific bacteria. Physicists have identified a natural delivery system which can safely carry potent antibiotics throughout the body to selectively attack and kill bacteria by using red blood cells as a vehicle. Researchers have developed a way to open red blood cells and remove the inner components, leaving only a membrane -- known as a liposome -- which can be loaded with drug molecules and injected back into the body. The process also involves coating the outside of the membrane with antibodies, allowing it to stick to bacteria and deliver the antibody safely.
Variable Bacteria living in your Mouth. Researchers take a closer look at the genomes of microbial communities in the human mouth. Researchers have examined the human oral microbiome and discovered tremendous variability in bacterial subpopulations living in certain areas of the mouth. In many cases, the team was able to identify a handful of genes that might explain a particular bacterial group's habitat specificity. The team scoured public databases and downloaded 100 genomes that represented four species of bacteria commonly found in the mouth, Haemophilus parainfluenzae and the three oral species of the genus Rothia, and used them as references to investigate their relatives sampled in hundreds of volunteers' mouths from the Human Microbiome Project (HMP).
Bacterial cells transmit memories to offspring. Bacterial cells can 'remember' brief, temporary changes to their bodies and immediate surroundings, a new study has found. And, although these changes are not encoded in the cell's genetics, the cell still passes memories of them to its offspring -- for multiple generations. Temporary stress can cause heritable changes without altering the genetics, study finds.
How the oceans' most abundant bacteria impact global nutrient flows. If you were to collect all the organisms from the ocean surface down to 200 meters, you'd find that SAR11 bacteria, though invisible to the naked eye, would make up a fifth of the total biomass. These bacteria, also known as Pelagibacterales, have evolved to thrive in nutrient-poor marine environments and play a significant role in global nutrient cycles. Despite their importance, the mechanisms behind their impact on the planetary ecosystem have remained unclear. But now, a recent article sheds light on a crucial aspect of these bacteria.
Bacteria's secret weapon revealed. Scientists have discovered a previously unknown method used by bacteria to evade immune responses. The study showed that immune cells sense that their mitochondria are no longer functional during infections, which triggers apoptosis. Ironically, it is the activation of host cell death factors that deliver the final blow to mitochondria which induces apoptosis, not the bacterial toxins themselves.
Sneezing
 Sneezing is a semi-autonomous, convulsive expulsion of air from the
lungs through the nose and mouth, usually caused by foreign particles
irritating the nasal mucosa. A sneeze expels air forcibly from the mouth
and nose in an explosive, spasmodic involuntary action resulting chiefly from irritation of the
nasal mucous
membrane. Sneezing is possibly linked to sudden exposure to bright light,
sudden change or fall in temperature, breeze of cold air, a particularly
full stomach, or viral infection, and can lead to the spread of disease.
Sneezing is a semi-autonomous, convulsive expulsion of air from the
lungs through the nose and mouth, usually caused by foreign particles
irritating the nasal mucosa. A sneeze expels air forcibly from the mouth
and nose in an explosive, spasmodic involuntary action resulting chiefly from irritation of the
nasal mucous
membrane. Sneezing is possibly linked to sudden exposure to bright light,
sudden change or fall in temperature, breeze of cold air, a particularly
full stomach, or viral infection, and can lead to the spread of disease.Photo on the right is what a sneeze looks like in slow motion, discharging mucus containing foreign particles.
Photic Sneeze Reflex causes variable difficulty to control sneezing in response to numerous stimuli, like the Sun. Maxillary Nerve transmits sensations from the nasal cavity and sinuses.
To sneeze gently without throwing out your back, avoid bending forward, which increases spinal disc pressure. Instead, stand up straight or sit up straight with a neutral spine, and lightly brace your core muscles, and bend your knees slightly. If possible, support your upper body by leaning on a table or chair. Engage your abdominal muscles before the sneeze to support your lumbar spine. If sitting, place your hands on your lap for support. Sneeze up rather than forward to avoid high-impact forward bending. Keep your core engaged for a few seconds after the sneeze to continue supporting your spine, as back pain often happens immediately after the pressure is released.
Allergies - Pollution - Germs - Clay (soil science) - Biology - Immune System - Washing your Hands
Cough is a sudden and often repetitively occurring reflex which helps to clear the large breathing passages from fluids, irritants, foreign particles and microbes. The cough reflex consists of three phases: an inhalation, a forced exhalation against a closed glottis, and a violent release of air from the lungs following opening of the glottis, usually accompanied by a distinctive sound. Coughing is either voluntary or involuntary. Coughing Dangers (image). Instead of cough syrup, consider sipping hot lemon tea with honey instead. A common cold may be the source of your throat tickle. This viral condition causes symptoms in your upper respiratory tract, including your throat. A cold symptom that may lead to a throat tickle is postnasal drip, which causes mucus to run down the back of your throat. Coughing is a sudden noisy expulsion of air from the lungs that clears the air passages. A common symptom of upper respiratory infection, bronchitis, pneumonia or tuberculosis. Exhale abruptly, as when one has a chest cold or congestion.
Common Cold is a viral infectious disease of the upper respiratory tract that primarily affects the nose. The throat, sinuses, and voice box may also be affected. Signs and symptoms may begin less than two days following exposure. They include coughing, sore throat, runny nose, sneezing, headache, and fever. People usually recover in seven to ten days. Some symptoms may last up to three weeks. In those with other health problems, pneumonia may occasionally develop.
Cold Remedies (Mayoclinic) - Webmd Remedies
Cold Weather and Freezing Temperatures affect the Body. Exposure to cold and dry air may adversely impact the body's immune system. Breathing in cold and dry air causes the blood vessels in the upper respiratory tract to narrow to conserve heat. This may prevent white blood cells from reaching the mucous membrane, making it harder for the body to fight off germs and allowing them to slip past our defenses unnoticed. Cold weather acts as a vasoconstrictor, which means it narrows blood vessels. It could be for this reason that we tend to catch a cold if we go outside with wet hair. Blood pressure increases during the winter, which can cause a wintertime increase in the death rate from heart attacks, strokes, and other cardiovascular causes of death. Older adults are at risk for hypothermia, in which the body's internal temperature falls too low. Shivering is another familiar defense mechanism against falling body temperatures. The rapid, rhythmic muscle contractions throw off heat that helps the rest of the body stay warm. Taller people tend to get cold faster than shorter people because a larger surface area means more heat loss. Brown fat is the heat-producing, calorie-burning fat that babies need to regulate their body temperatures. Flu season is a winter event, and flu viruses spread more readily once the air is dry and chilly. And during winter months, people spend more time inside and in close contact with each other, meaning that we’re in closer contact with other people who may be carrying germs. Viruses from coughs and sneezes can hang around in the air for days because of the drier air in the winter. Sun-exposed skin makes vitamin D, a vitamin that seems to have all kinds of health benefits. During the winter, when days are short and the sun is at a low angle, levels of the vitamin in the body tend to dip. Cold temperatures and low vitamin D levels may be a bad combination because it lowers the body’s immune system. Dry winter air can suck the moisture from your skin, which could cause dehydration, and not just dry skin. Washing Hands. Air Conditioners in summer can also be a problem.
Flu Virus' best friend: Low Humidity. Low humidity hinders the immune response of the animals in three ways. It prevented cilia, which are hair-like structures in airways cells, from removing viral particles and mucus. It also reduced the ability of airway cells to repair damage caused by the virus in the lungs. The third mechanism involved interferons, or signaling proteins released by virus-infected cells to alert neighboring cells to the viral threat. In the low-humidity environment, this innate immune defense system failed.
Why some people exposed to the Cold Virus get ill while others don't? A Yale research team has revealed how cells in different parts of the human airway vary in their response to the common cold virus. Researchers triggered the virus surveillance pathway -- known as the RIG-I pathway -- in both nasal and lung cells. They found that both cell types generated an antiviral response and a defense response against oxidative stress, a form of cell damage induced by viruses and other inhaled irritants such as cigarette smoke or tree pollen. In nasal cells, the antiviral response was stronger, but in bronchial cells, defense against oxidative stress was more pronounced. In additional experiments, the research team found evidence for a tradeoff: The defense response against oxidative stress shut off antiviral defenses. To probe this further, the team exposed nasal cells to oxidative stress in the form of cigarette smoke, and then to the cold virus, and found that the nasal cells were more susceptible to the virus. They survive the cigarette smoke but can't fight the virus as well.
You Get Less Colds as you get older. You're less likely to get sick with colds and other minor viral infections after midlife because each time your body is exposed to a virus, it develops antibodies that make you immune to that virus in the future. This means that more you age, the more likely it is that you'll be immune to many — but not all — cold viruses. There are more than 200 different viruses that cause colds. "But by the time you reach your 60s or 70s with a lifetime of colds behind you, you've developed immunity to many of the circulating cold viruses. After age 50, the body reacts with less vehemence to hay fever and other seasonal allergies, perhaps because older bodies produce less of the allergic ntibody IgE.
Mucus - Phlegm - Congestion - Nasal Sinuses
 Nasal Congestion is the blockage of the
nasal passages usually due to membranes lining the nose becoming swollen
from inflamed blood vessels.
Nasal Congestion is the blockage of the
nasal passages usually due to membranes lining the nose becoming swollen
from inflamed blood vessels.
Relieve Stuffy Nose Instantly (youtube) - Relieve Head Congestion - Relieve Ear Congestion - Immune Response - Nose Breathing
Nasal Cycle is the result of alternating congestion and decongestion of the nasal conchae or turbinates, predominantly the inferior turbinates, which are by far the largest of the turbinates in each nasal fossa. The cycle, which is controlled by the autonomic nervous system, has a mean duration of two and a half hours. It has been shown that the cilia of the congested side suspend their motility until that side decongests. Thus the cycle ensures that one side of the nose is always moist, to facilitate humidification, which is one of the three functions of the nose, the other two being filtration and warming of inspired air prior to its entering the lungs.
 Sinusitis
is inflammation of the sinuses resulting in symptoms.
Sinusitis
is inflammation of the sinuses resulting in symptoms.
Sinus Infection - Colloidal Silver
Nasal Irrigation is a personal hygiene practice in which the nasal cavity is washed to flush out excess mucus and debris from the nose and sinuses. The practice is generally well-tolerated and reported to be beneficial with only minor side effects. Nasal irrigation in a wider sense can also refer to the use of saline nasal spray or nebulizers to moisten the mucous membranes.
It is the Mucus that Binds Us - Ace Ventura, Binding Mucus Scene (youtube)
Phlegm is a liquid secreted by the mucous membranes of mammals. Its definition is limited to the mucus produced by the respiratory system, excluding that from the nasal passages, and particularly that which is expelled by coughing (sputum). Phlegm is in essence a water-based gel consisting of glycoproteins, immunoglobulins, lipids and other substances. Its composition varies depending on climate, genetics, and state of the immune system. Its color can vary from transparent to pale or dark yellow and green, from light to dark brown, and even to dark grey depending on the constituents.
Get Rid of Phlegm in Your Throat Without Medicine. Boil cup of water. Add 1/4 cup apple cider vinegar. One tablespoon of Honey. A dash of Cayenne Pepper. A little Lemon Juice. Let it get to room temperature and drink one cup in the morning and one at night.
Make sure that you drink plenty of liquids such as water, juice or tea with honey, and gargle daily with warm salt water to thin out mucus. Another easy fix to get rid of excess mucus, is to add eucalyptus oil to a tub of boiling water and inhale the vapors which will help to drain the mucus from the throat and chest.
Mucus is a slippery aqueous secretion produced by, and covering, mucous membranes. It is typically produced from cells found in mucous glands, although it may also originate from mixed glands, which contain both serous and mucous cells. It is a viscous colloid containing inorganic salts, antimicrobial enzymes (such as lysozymes), immunoglobulins, and glycoproteins such as lactoferrin and mucins, which are produced by goblet cells in the mucous membranes and submucosal glands. Mucus serves to protect epithelial cells (that line the tubes) in the respiratory, gastrointestinal, urogenital, visual, and auditory systems; the epidermis in amphibians; and the gills in fish, against infectious agents such as fungi, bacteria and viruses. Most of the mucus produced is in the gastrointestinal tract.
How mucus tames microbes. Specialized sugar molecules called glycans can disarm opportunistic pathogens and prevent infection. New research reveals that glycans -- branched sugar molecules found in mucus -- can prevent bacteria from communicating with each other and forming infectious biofilms, effectively rendering the microbes harmless.
Researchers identify how cells move faster through mucus than blood. Researchers have discovered that certain cells move surprisingly faster in thicker fluid because their ruffled edges sense the viscosity of their environment and adapt to increase their speed. Their combined results in cancer and fibroblast cells suggest that the viscosity of a cell's surrounding environment is an important contributor to disease, and may help explain tumor progression, scarring in mucus-filled lungs affected by cystic fibrosis, and the wound-healing process.
Goblet Cell are simple columnar epithelial cells that secrete gel-forming mucins, like mucin MUC5AC. The goblet cells mainly use the merocrine method of secretion, secreting vesicles into a duct, but may use apocrine methods, budding off their secretions, when under stress. The term goblet refers to the cell's goblet-like shape. The apical portion is shaped like a cup, as it is distended by abundant mucus laden granules; its basal portion lacks these granules and is shaped like a stem. The goblet cell is highly polarized with the nucleus and other organelles concentrated at the base of the cell and secretory granules containing mucin, at the apical surface. The apical plasma membrane projects microvilli to give an increased surface area for secretion. Goblet cells are typically found in the respiratory, reproductive and gastrointestinal tracts and are surrounded by stratified squamous cells. Differentiation of epithelial cells into goblet cells plays a key role in the excessive mucus production seen in many diseases, such as asthma and cancer.
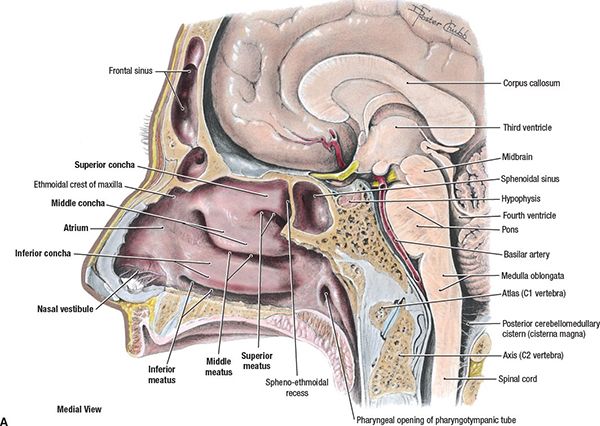 Nasal Cavity is a
large, air-filled space above and behind the nose in the middle of the
face. The nasal septum divides the cavity into two cavities, also known as
fossae. Each cavity is the continuation of one of the two nostrils. The
nasal cavity is the uppermost part of the respiratory system and provides
the nasal passage for inhaled air from the nostrils to the nasopharynx and
rest of the respiratory tract. The paranasal sinuses surround and drain
into the nasal cavity. The nasopharynx is the upper part of the throat (pharynx)
that lies behind the nose. It's a box-like chamber about 1½ inches on each
edge. It lies just above the soft part of the roof of the mouth (soft
palate) and just in back of the nasal passages.
Swab Test.
Nasal Cavity is a
large, air-filled space above and behind the nose in the middle of the
face. The nasal septum divides the cavity into two cavities, also known as
fossae. Each cavity is the continuation of one of the two nostrils. The
nasal cavity is the uppermost part of the respiratory system and provides
the nasal passage for inhaled air from the nostrils to the nasopharynx and
rest of the respiratory tract. The paranasal sinuses surround and drain
into the nasal cavity. The nasopharynx is the upper part of the throat (pharynx)
that lies behind the nose. It's a box-like chamber about 1½ inches on each
edge. It lies just above the soft part of the roof of the mouth (soft
palate) and just in back of the nasal passages.
Swab Test.Mucous Membrane is a membrane that lines various cavities in the body and surrounds internal organs. It consists of one or more layers of epithelial cells overlying a layer of loose connective tissue. It is of entodermal origin and is continuous with the skin at various body openings such as the eyes, ears, inside the nose, inside the mouth, lip, the urethral opening and the anus, frenulum of tongue, tongue. Some mucous membranes secrete mucus, a thick protective fluid. The function of the membrane is to stop pathogens and dirt from entering the body and to prevent bodily tissues from becoming dehydrated.
The following actions can help to eliminate excess mucus and phlegm: Keeping the air moist. Drinking plenty of Clean Water. Applying a warm, wet washcloth to the face. Keeping the head elevated. Not suppressing a cough. Discreetly getting rid of phlegm. Using a saline nasal spray or rinse. Gargling with salt water. Hold the breath for 2-3 seconds. Use your stomach muscles to forcefully expel the air. Avoid a hacking cough or merely clearing the throat. A deep cough is less tiring and more effective in clearing mucus out of the lungs.
Postnasal Drip happens when your body starts producing extra mucus. Excess mucus moving into your stomach can cause nausea. Swallowing mucus produced with a respiratory infection is not harmful. The stomach works to neutralise bacteria and recycle the other cellular debris. Some people do report a queasy feeling in the stomach during such infections. Postnasal drip makes you feel like you constantly want to clear your throat. It also can trigger a cough, which often gets worse at night. A simple way to thin it out is to drink more water. Other methods you can try include: Take a medication such as guaifenesin (Mucinex). Use saline nasal sprays or irrigation , like a neti pot, to flush mucus, bacteria, allergens, and other irritating things out of the sinuses. (Postnasal drainage).
Phlegm is a slightly different substance than mucus. It's a form of mucus produced by the lower airways — not by the nose and sinuses — in response to inflammation. You may not notice phlegm unless you cough it up as a symptom of bronchitis or pneumonia. Histamine causes the tissue in your nasal passages to swell and produce more, thinner mucus. This usually leads to a runny nose, as well as sneezing, itching, and nasal stuffiness. Having thick mucus can make it seem like more mucus is being produced and can create problems, such as postnasal drip.
Laryngopharyngeal Reflux is a condition in which acid that is made in the stomach travels up the esophagus (swallowing tube) and gets to the throat. Symptoms include sore throat and an irritated larynx (voice box). Treatments consist mostly of lifestyle changes.
Congestion tends to be worse at night because it is harder for the nose and sinuses to drain. This means that mucus pools in the head, making it harder to breathe and potentially causing a sinus headache in the morning. Try elevating the head on a few pillows to help the sinuses drain more easily.
Sinuses can be affected by atmospheric pressure. When the outside barometric pressure changes, it can create a difference between the pressure in the outside air and the air in your sinuses, which can result in pain. Barometric pressure changes can affect inflammation in the nose and sinuses, and then can be experienced by individuals as pressure and/or pain. When experiencing aerosinusitis, the pressure difference causes the mucosal lining of the sinuses to swell.
Aerosinusitis is a painful inflammation and sometimes bleeding of the membrane of the paranasal sinus cavities, normally the frontal sinus. It is caused by a difference in air pressures inside and outside the cavities.
Mucus Causing or Mucus-Thickening Foods to Consider Removing from your Diet: Red meat, Milk, Cheese, Yogurt, Ice Cream, Butter, Eggs, Bread, Pasta, Cereal, Bananas, Cabbage, Potatoes, Corn and corn products, Soy products, Sweet desserts, Candy, Coffee, Tea, Soda, Alcoholic beverages. (results may vary from person to person).
Foods that may Reduce Mucus: Salmon, Tuna, Sardines, Flounder, Pumpkin, Pumpkin seeds, Grapefruit, Pineapple, Watercress, Celery, Pickles, Onion, Garlic, Honey or Agar, Ginger, Licorice, Berries, Echinacea, Pomegranate, Oral Zinc, Lemon, Cayenne pepper, Chamomile, Olive oil, Broth, Decaf tea, Guava Tea. Allergies.
Molecules found in mucus can thwart fungal infection. Harnessing the strength of these specialized sugar molecules could help researchers develop new antifungal drugs.
Flu - Pneumonia - Influenza
Pneumonia is an inflammatory condition of the lung affecting primarily the microscopic air sacs known as alveoli. Typical signs and symptoms include a varying severity and combination of productive or dry cough, chest pain, fever, and trouble breathing, depending on the underlying cause. Pneumonia is usually caused by infection with viruses or bacteria and less commonly by other microorganisms, certain medications and conditions such as autoimmune diseases. Risk factors include other lung diseases such as cystic fibrosis, COPD, and asthma, diabetes, heart failure, a history of smoking, a poor ability to cough such as following a stroke, or a weak immune system. Diagnosis is often based on the symptoms and physical examination. Chest X-ray, blood tests, and culture of the sputum may help confirm the diagnosis. The disease may be classified by where it was acquired with community, hospital, or health care associated pneumonia. Vaccines to prevent certain types of pneumonia are available. Other methods of prevention include hand washing and not smoking. Treatment depends on the underlying cause. Pneumonia believed to be due to bacteria is treated with antibiotics. Walking pneumonia is a non-medical term for a mild case of pneumonia that isn't severe enough to require bed rest or hospitalization. If the pneumonia is severe, the affected person is generally hospitalized. Oxygen therapy may be used if oxygen levels are low. Pneumonia affects approximately 450 million people globally (7% of the population) and results in about 4 million deaths per year. Contagious.
Differences between the Flu and Pneumonia. The flu usually comes on suddenly, while pneumonia takes longer to develop and can be a complication from the flu. The flu is caused by a viral infection, while pneumonia can be caused by either a bacterial infection or viral infection. Pneumonia is a lung infection, it typically has more respiratory symptoms, while the flu is accompanied by muscular aches and pains and fatigue. Flu symptoms include: Body aches and pains, Dry cough, Extreme fatigue, Fever above 100.4 degrees, Headache. Pneumonia symptoms include: Bluish fingernails and lips, Chills, Confusion (most common in older adults), Coughing, Decreased appetite, Extreme fatigue, Fever up to 105 degrees, Pain when breathing deeply, Quick heartbeat and breathing, Sweating, Trouble catching your breath, Wheezing (common in children), Yellow, greenish or bloody mucus when you cough.
A New Hypervirulent (Hypermucoviscous) variant of Klebsiella Pneumoniae has emerged. Defining clinical features are the ability to cause serious, life-threatening community-acquired infection in younger healthy hosts, including liver abscess, pneumonia, meningitis and endophthalmitis and the ability to metastatically spread, an unusual feature for enteric Gram-negative bacilli in the non-immunocompromised. Despite infecting a healthier population, significant morbidity and mortality occurs. Although epidemiologic features are still being defined, colonization, particularly intestinal colonization, appears to be a critical step leading to infection. However the route of entry remains unclear. Colds.
Hypervirulent means that something is extremely infectious, malignant, or poisonous. Used of a disease or toxin. Capable of causing disease by breaking down protective mechanisms of the host. Used of a pathogen. Intensely irritating, obnoxious, or harsh.
Hypersensitivity Pneumonitis is an inflammation of the alveoli within the lung caused by hypersensitivity to inhaled organic dusts. Sufferers are commonly exposed to the dust by their occupation or hobbies. Symptoms include fever, chills, malaise, cough, chest tightness, dyspnea, rash, swelling and headache. Symptoms resolve within 12 hours to several days upon cessation of exposure. (sometimes called wet lung).
Why virus hits some people harder than others. People's ability to fight off the flu virus is determined not only by the subtypes of flu they have had throughout their lives, but also by the sequence in which they are been infected by the viruses. People whose first childhood exposure was to H2N2, a close cousin of H1N1, did not have a protective advantage when they later encountered H1N1. Most infected travelers are undetectable, meaning that they have no symptoms yet, and are unaware that they have been exposed. Vulnerabilities.
Alveolar macrophages help CD8+ T cells go (anti-)viral. Researchers have found that antigen-specific killer T cells or CD8+ T cells rapidly expand in the lungs when primed by antigen-presenting lung-resident alveolar macrophages or AMs. This interaction helps protect against viral infection and could form the basis for developing 'cell transplant'-type vaccines in the future. The human immune system is a highly complex network of cells, signals, and responses that is tightly regulated to ensure that the body can fight off infection without damaging its own tissues. Now, researchers from Japan report a new way in which the immune system protects lung tissue from viral infections. CD8+ T cells confer protective immunity against infection with respiratory viruses, such as influenza A virus (IAV) and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), by killing infected cells. In order to target the correct cells for killing, naive CD8+ T cells must be primed by contact with antigen-presenting cells (APCs), which mediate the uptake of virus-infected cells and present their antigens, in a process known as cross-presentation. The primed CD8+ T cells then clonally expand and differentiate into effector or long-lived antigen-specific memory T cells.
New study shows environmental and social factors contribute to higher rates of pneumonia in children. A new study demonstrates that children who are exposed to a certain type of environmental air pollution are more likely to contract community acquired pneumonia, or CAP, and to be hospitalized for longer periods of time. Social factors, including race and socioeconomic status, were also found to be associated with living in high-risk areas for CAP.
Why older people are more susceptible to the flu. An inflammation-controlling lipid appears to weaken the lungs' immune defenses. These macrophages are immune cells that attack invaders like the flu virus and live in the small air sacs, or alveoli, inside the lungs. Importantly, these cells appear to be lost with aging. Signs pointed to a lipid immune modulator known as prostaglandin E2 (PGE2) with wide ranging effects, from labor induction in pregnancy to inflammation with arthritis. The study team discovered there is more PGE2 in the lungs with age. This increase in PGE2, Chen explained, acts on the macrophages in the lung, limiting their overall health and ability to generate. The team suspects that the buildup of PGE2 is yet another marker of a biological process called senescence, which is often seen with age. Senescence serves as insurance against the runaway division of damaged cells; cells that are senescent are no longer able to replicate.
Oseltamivir is an antiviral medication used to treat and prevent influenza A and influenza B (flu), which is sold under the brand name Tamiflu. Many medical organizations recommend it in people who have complications or are at high risk of complications within 48 hours of first symptoms of infection. They recommend it to prevent infection in those at high risk, but not the general population. The Centers for Disease Control and Prevention (CDC) recommends that clinicians use their discretion to treat those at lower risk who present within 48 hours of first symptoms of infection. It is taken by mouth, either as a pill or liquid. Common side effects include vomiting, diarrhea, headache, and trouble sleeping. Other side effects may include psychiatric symptoms and seizures. In the United States it is recommended for influenza infection during pregnancy. It has been taken by a small number of pregnant women without signs of problems. Dose adjustment may be needed in those with kidney problems. Oseltamivir was approved for medical use in the US in 1999. It was the first neuraminidase inhibitor available by mouth. It is on the World Health Organization's List of Essential Medicines but was downgraded to "complementary" status in 2017. A generic version was approved in the US in 2016. In 2018, it was the 93rd most commonly prescribed medication in the United States, with more than 8 million prescriptions. Neuraminidase inhibitor are a class of drugs which block the neuraminidase enzyme. Neuraminidase or Sialidase enzymes are glycoside hydrolase enzymes that cleave or cut the glycosidic linkages of neuraminic acids.
Acute Respiratory Distress Syndrome is characterized by widespread inflammation in the lungs triggered by various pathologies such as trauma, pneumonia, and sepsis. The hallmark of ARDS is diffuse injury to cells which form the barrier of the microscopic air sacs of the lungs, surfactant dysfunction, activation of the innate immune system response, and dysfunction of the body's regulation of clotting and bleeding. In effect, ARDS impairs the lungs' ability to exchange oxygen and carbon dioxide with the blood across a thin layer of the lungs' microscopic air sacs known as alveoli.
Lung cell transplant boosts healing after the flu in mice. The method is also applicable in other models of lung injury. The transplant -- achieved by taking specialized lung cells called Alveolar Type-Two Cells from the healthy animals and then allowing the sick animals to simply breathe in the cells -- led to improved blood-oxygen levels.
Pulmonary Alveolus is a hollow cup-shaped cavity found in the lung parenchyma where gas exchange takes place. Lung alveoli are found in the acini at the ends of the respiratory tree. They are located sparsely on the respiratory bronchioles, and walls of the alveolar ducts, and are more numerous in the blind-ended alveolar sacs. The acini mark the beginning of the respiratory zone, are the basic units of respiration, with gas exchange taking place in all the alveoli present. The alveolar membrane is the gas exchange surface, surrounded by a network of capillaries. Across the membrane oxygen is diffused into the capillaries and carbon dioxide released from the capillaries into the alveoli to be breathed out.
Motility motility is the ability to move spontaneously and actively, consuming energy in the process. It is not to be confused with mobility, which describes the ability of an object to be moved. Motility is genetically determined.
Klebsiella is a genus of nonmotile, Gram-negative, oxidase-negative, rod-shaped bacteria with a prominent polysaccharide-based capsule. Klebsiella species are found everywhere in nature. They can be found in water, soil, plants, insects, animals, and humans.
Breathing - Lungs
Influenza commonly known as "The Flu", is an infectious disease caused by an influenza virus. Symptoms can be mild to severe. The most common symptoms include: a high fever, runny nose, sore throat, muscle pains, headache, coughing, and feeling tired. These symptoms typically begin two days after exposure to the virus and most last less than a week. The cough, however, may last for more than two weeks. In children, there may be nausea and vomiting, but these are not common in adults. Nausea and vomiting occur more commonly in the unrelated infection gastroenteritis, which is sometimes inaccurately referred to as "stomach flu" or "24-hour flu". Complications of influenza may include viral pneumonia, secondary bacterial pneumonia, sinus infections, and worsening of previous health problems such as asthma or heart failure.
Flu Near You - Flu Cast - Flu.gov - Pandemic
1918 Influenza Pandemic was the most severe pandemic in recent history. It was caused by an H1N1 virus with genes of avian origin. The number of deaths was estimated to be at least 50 million worldwide with about 675,000 occurring in the United States. 80,000 people died in U.S. of flu last winter in 2018, highest death toll in 40 years.
Flu Researchers discover new mechanism for battling influenza.
Emergency Preparedness for Disease Outbreaks (containment)
Influenza A virus kills 12,000 to 56,000 people in the United States annually. Human protein called TRIM25, also a "restriction factor, is a special protein present in the fastest-acting arm of the immune system, before spreading infection occurs. Restriction factors lie in wait, and should a virus be detected in one of your cells, they have immediate destructive ability. TRIM25 plays important role in the human immune response to flu infection; and a protein called NS1 present in all strains of the influenza A virus and shown to bind TRIM25 to keep it from doing its job. TRIM25 acts earlier than previously believed, latching on to a critical and unique flu virus structure like a "molecular clamp" to keep the virus from replicating as soon as TRIM25 detects this unique structure. NS1 produced by the flu virus can block this function of TRIM25, enabling flu to circumvent the immune response and cause infection. Previous research had suggested that TRIM25 fought off flu by switching on what is known as the "interferon response" -- a complex signaling pathway that arms cells through the body to fight off pathogens. But not all strains of influenza block this interferon signaling pathway. TRIM25 (previously believed to be present only in the cell cytoplasm) is also present in the cell nucleus, which is the same cellular location where flu replication occurs.
Estimated Influenza Disease Burden — United States (wiki)
Flu Season Hospitalizations Deaths
2010 – 2011 (270,000 – 350,000) (32,000 – 51,000)
2011 – 2012 (130,000 – 190,000) (11,000 – 23,000)
2012 – 2013 (530,000 – 680,000) (37,000 – 57,000)
2013 – 2014 (320,000 – 390,000) (33,000 – 50,000)
2014 – 2015 (540,000 – 680,000) (44,000 – 64,000)
2015 – 2016 (220,000 – 480,000) (17,000 – 35,000)
2016 – 2017 (380,000 – 860,000) (29,000 – 61,000)
2017 – 2018* (620,000 – 1,400,000) (46,000 – 95,000)
2018 – 2019* (387,283 – 766,472) (26,339 – 52,664)
During the 2019-2020 influenza season, CDC estimates that influenza was associated with 38 million illnesses, 18 million medical visits, 405,000 hospitalizations, and 22,000 deaths. The influenza burden was higher in young children (0-4 years) and adults (18-49 years) compared with a recent season with the 2017-2018 season, a recent season with high severity, and provides evidence to support how severe seasonal influenza can be at any age. Covid.
Natural compound coupled with specific gut microbes may prevent severe flu. A Gut microbe can prevent severe flu infections in mice, likely by breaking down naturally occurring compounds called flavonoids, which are commonly found in foods such as black tea, red wine and blueberries. Desaminotyrosine or DAT kept the immune system from harming the lung tissue.
2022, highly contagious bird flu virus triggering the deaths of some 52.7 million animals. The highly pathogenic avian influenza has ravaged farm flocks and chicken yards in 46 states since February, when the first cases were reported in commercial flocks. The vast majority are being culled through flock depopulation, to try to stop the virus from spreading. That includes millions of chickens and turkeys in barns and backyards that had been raised to provide eggs or meat. 2022 Detections of Highly Pathogenic Avian Influenza in Wild Birds.
The first U.S. case of a person infected with avian influenza A or H5N1 virus was reported in April in Colorado. The patient recovered after experiencing a few days of fatigue.
Infections
Infection is the physical condition or pathological state resulting from the invasion of the body by pathogenic microorganisms. An incident in which an infectious disease is transmitted.
Hospital Infections - Fungal Infections - Bacteria - Inflammation - Immune System - Resistance - Fever - Pandemic - Contagion
Infection is the invasion of an organism's body tissues by disease-causing agents, their multiplication, and the reaction of host tissues to these organisms and the toxins they produce. Infectious disease, also known as transmissible disease or communicable disease, is illness resulting from an infection. Infections are caused by infectious agents including viruses, viroids, prions, bacteria, nematodes such as parasitic roundworms and pinworms, arthropods such as ticks, mites, fleas, and lice, fungi such as ringworm, and other macroparasites such as tapeworms and other helminths. Hosts can fight infections using their immune system. Mammalian hosts react to infections with an innate response, often involving inflammation, followed by an adaptive response. Ignorance is one of the most deadliest infections in the world, and knowledge is the cure.
Anaerobic Infection are caused by anaerobic bacteria. Obligately anaerobic bacteria do not grow on solid media in room air (0.04% carbon dioxide and 21% oxygen); facultatively anaerobic bacteria can grow in the presence or absence of air. Microaerophilic bacteria do not grow at all aerobically or grow poorly, but grow better under 10% carbon dioxide or anaerobically. Anaerobic bacteria can be divided into strict anaerobes that can not grow in the presence of more than 0.5% oxygen and moderate anaerobic bacteria that are able of growing between 2 and 8% oxygen. Anaerobic bacteria usually do not possess catalase, but some can generate superoxide dismutase which protects them from oxygen.
Respiratory Tract Infection refers to any of a number of infectious diseases involving the respiratory tract. An infection of this type is normally further classified as an upper respiratory tract infection (URI or URTI) or a lower respiratory tract infection (LRI or LRTI). Lower respiratory infections, such as pneumonia, tend to be far more serious conditions than upper respiratory infections, such as the common cold. Air Pollution.
Most infants receiving ICU-level care for RSV. Most infants admitted to the intensive care unit or high acuity unit for respiratory syncytial virus or RSV infections during fall 2022, were previously healthy and had no underlying medical condition and were born at term, according to a new study.
Subclinical Infection is an infection that, being subclinical, is nearly or completely asymptomatic with no signs or symptoms. A subclinically infected person is thus an asymptomatic carrier of a microbe, intestinal parasite, or virus that usually is a pathogen causing illness, at least in some individuals. Many pathogens spread by being silently carried in this way by some of their host population. Such infections occur both in humans and nonhuman animals. An example of an asymptomatic infection is a mild common cold that is not noticed by the infected individual. Since subclinical infections often occur without eventual overt sign, their existence is only identified by microbiological culture or DNA techniques such as polymerase chain reaction.
Hospital Infections - No Symptoms
Contagious Infectious Disease is the invasion of an organism's body tissues by disease-causing agents, their multiplication, and the reaction of host tissues to these organisms and the toxins they produce. Infectious disease, also known as transmissible disease or communicable disease, is illness resulting from an infection. Infections are caused by infectious agents including viruses, viroids, prions, bacteria, nematodes such as parasitic roundworms and pinworms, arthropods such as ticks, mites, fleas, and lice, fungi such as ringworm, and other macroparasites such as tapeworms and other helminths. Hosts can fight infections using their immune system. Mammalian hosts react to infections with an innate response, often involving inflammation, followed by an adaptive response. Specific medications used to treat infections include antibiotics, antivirals, antifungals, antiprotozoals, and antihelminthics. Infectious diseases resulted in 9.2 million deaths in 2013 (about 17% of all deaths). The branch of medicine that focuses on infections is referred to as infectious disease.
Co-Infection is the simultaneous infection of a host by multiple pathogen species. In virology, coinfection includes simultaneous infection of a single cell by two or more virus particles. An example is the coinfection of liver cells with hepatitis B virus and hepatitis D virus, which can arise incrementally by initial infection followed by superinfection. Global prevalence or incidence of coinfection among humans is unknown, but it is thought to be commonplace, sometimes more common than single infection. Coinfection with helminths affects around 800 million people worldwide. Coinfection is of particular human health importance because pathogen species can interact within the host. The net effect of coinfection on human health is thought to be negative. Interactions can have either positive or negative effects on other parasites. Under positive parasite interactions, disease transmission and progression are enhanced and this is also known as syndemism. Negative parasite interactions include microbial interference when one bacterial species suppresses the virulence or colonisation of other bacteria, such as Pseudomonas aeruginosa suppressing pathogenic Staphylococcus aureus colony formation. The general patterns of ecological interactions between parasite species are unknown, even among common coinfections such as those between sexually transmitted infections. However, network analysis of a food web of coinfection in humans suggests that there is greater potential for interactions via shared food sources than via the immune system. A globally common coinfection involves tuberculosis and HIV. In some countries, up to 80% of tuberculosis patients are also HIV-positive. The potential for dynamics of these two infectious diseases to be linked has been known for decades. Other common examples of coinfections are AIDS, which involves coinfection of end-stage HIV with opportunistic parasites and polymicrobial infections like Lyme disease with other diseases. Coinfections sometimes can epitomize a zero sum game of bodily resources, and precise viral quantitation demonstrates children co-infected with rhinovirus and respiratory syncytial virus, metapneumovirus or parainfluenza virus have lower nasal viral loads than those with rhinovirus alone.
Super-Infection is a second infection superimposed on an earlier one, especially by a different microbial agent of exogenous or endogenous origin, that is resistant to the treatment being used against the first infection. Examples of this in bacteriology are the overgrowth of endogenous Clostridium difficile that occurs following treatment with a broad-spectrum antibiotic, and pneumonia or sepsis from Pseudomonas aeruginosa in some immunocompromised patients. In virology, the definition is slightly different. Superinfection is the process by which a cell that has previously been infected by one virus gets co-infected with a different strain of the virus, or another virus, at a later point in time. Viral superinfections may be resistant to the antiviral drug or drugs that were being used to treat the original infection. Viral superinfections may also be less susceptible to the host's immune response. Recent metagenomic analyses have demonstrated that the novel coronavirus, SARS-CoV-2 can be associated with superinfection and colonization of other pathogens, such as rhinovirus species and Moraxella spp. In parasitology, superinfection is reinfection of the same genus of parasite, as a person infected by Fasciola hepatica again infected by Fasciola gigantica. Super Bugs.
Viral Load is a measurement of the amount of a virus in an organism, typically in the bloodstream, usually stated in virus particles per milliliter. A numerical expression of the quantity of virus in a given volume of fluid; sputum and blood plasma being two bodily fluids. For example, the viral load of norovirus can be determined from run-off water on garden produce. Norovirus has not only prolonged viral shedding and has the ability to survive in the environment but a minuscule infectious dose is required to produce infection in humans: less than 100 viral particles. Viral load is often expressed as viral particles, or infectious particles per mL depending on the type of assay. A higher viral burden, titre, or viral load often correlates with the severity of an active viral infection. The quantity of virus / mL can be calculated by estimating the live amount of virus in an involved fluid. For example, it can be given in RNA copies per millilitre of blood plasma. Tracking viral load is used to monitor therapy during chronic viral infections, and in immunocompromised patients such as those recovering from bone marrow or solid organ transplantation. Currently, routine testing is available for HIV-1, cytomegalovirus, hepatitis B virus, and hepatitis C virus. Viral load monitoring for HIV is of particular interest in the treatment of people with HIV, as this is continually discussed in the context of management of HIV/AIDS.
Sepsis - Bacteria
A potential target for developing broad-spectrum antiviral therapies. Study finds inhibiting enzyme boosts the innate immune response. Researchers have identified a promising strategy for development of broad-spectrum antiviral therapies that centers around promoting a strong immune response capable of stopping a number of viruses in their infectious tracks. a key enzyme in that process, called NSUN2, to stop the RNA change. Suppressing NSUN2 using gene knockdown techniques and experimental agents, they found, sets off a cascade of cell activities that leads to robust production of type 1 interferon, one of the most potent fighters in the innate antiviral response.
Potential secret to viral resistance unearthed. Scientists have unearthed a secret that may explain why some people are able to resist viral infections, having screened the immune systems of women exposed to hepatitis C (HCV) through contaminated anti-D transfusions given over 40 years ago in Ireland. The extraordinary work has wide-ranging implications from improving our fundamental understanding of viral resistance to the potential design of therapies to treat infected people. Between 1977-79 in Ireland, several thousand women were exposed to the hepatitis C virus through contaminated anti-D, which is a medication made using plasma from donated blood and given to Rhesus negative women who are pregnant with a Rhesus positive fetus. The medication prevents the development of antibodies that could be dangerous in subsequent pregnancies. Some of the anti-D used during the 1977-79 period was contaminated with hepatitis C. We hypothesised that women who seemed to resist HCV infection must have an enhanced innate immune response, which is the ancient part of the immune system that acts as a first line of defence. By comparing the response of the resistant women to those who became infected, we found that resistant donors had an enhanced type I interferon response after stimulation. Type I interferons are a key family of antiviral immune mediators that play an important role in defence against viruses including hepatitis C and SARS-CoV-2, or COVID-19.
Fungal Infection is a fungus that invades the tissue can cause a disease that's confined to the skin, spreads into tissue, bones, and organs, or affects the whole body. Fungal infections often start in the lungs or on the skin.
Starving Fungi could save millions of lives each year. Researchers have identified a potentially new approach to treating lethal fungal infections that claim more than 1.6 million lives each year. Despite high levels of phosphate in the human body, the research showed that the infecting fungi are very poor at absorbing it. This causes the fungi to produce more transporters to try to bring in more phosphate -- a process known as the 'phosphate starvation response'. By blocking this phosphate starvation response -- and stopping the fungi from producing more transporters to get more nutrients -- the research team starved the fungi, preventing their spread of infection in mice.
Potential novel breakthrough treatment for fungal infections. Fungal infections are killing thousands of Americans each year, some with a morbidity rate of nearly 80%. To make matters worse, only a handful of antifungal treatments are available, and even those are becoming less effective as fungi become more resistant. However, researchers recently published findings indicating that a novel breakthrough treatment may have been discovered.
This simple blood protein could stop a deadly black fungus. Albumin, the most abundant protein in human blood. In a major international study, researchers found that people who develop mucormycosis — a fast-moving and often fatal “black fungus” infection — have strikingly low levels of albumin, and that this deficiency strongly predicts death.
Toxic Shock Syndrome is an infection that usually occurs when bacteria enter your body through an opening in your skin, such as a cut, sore, or other wound. Toxic Shock Syndrome is a condition caused by bacterial toxins. Symptoms may include fever, rash, skin peeling, and low blood pressure. There may also be symptoms related to the specific underlying infection such as mastitis, osteomyelitis, necrotising fasciitis, or pneumonia.
Hijacker parasite blocked from infiltrating blood. World's most widespread malaria parasite Plasmodium vivax (P. vivax) infects humans by hijacking a protein the body cannot live without.
Infectious Diseases Emergency Preparedness Plan.
Bioelectricity new weapon to fight dangerous infection. Drugs already approved for other uses in people help frogs survive deadly E. coli by changing their cells’ electrical charge.
Meningococcal Disease refers to any sickness caused by Neisseria meningitidis. The infection can lead to both meningitis and a serious infection of the bloodstream called septicemia, or blood poisoning.
Intranasal herpes infection may produce neurobehavioral symptoms. A study finds that herpes infection through the nose can lead to anxiety, motor impairment and cognitive issues. The research shows that by exploiting a cellular enzyme, the virus can produce behavioral symptoms. The finding emphasizes the need for prevention and treatment of a virus carried by billions of people worldwide.
How the brain responds to infection and controls symptoms of sickness. Researchers have discovered a small population of neurons near the base of the brain that can induce symptoms of sickness, including fever, appetite loss, and warm-seeking behavior. When someone gets an infection, most people think it's the immune system kicking into gear when they feel some of the body's natural defenses like a fever, chills, or fatigue. What most people don't know is that it's actually the brain behind all of this. The nervous system talks to the immune system to figure out that the body has an infection and then orchestrates a series of behavioral and physiological alterations that manifest as the unpleasant symptoms of sickness.
Scientists discover small RNA that regulates bacterial infection. Researchers have identified the major mechanism behind the transition between chronic and acute P. aeruginosa infections. Their research findings can inform the development of future treatments for life-threatening acute infections.
DNA Virus is a virus that has DNA as its genetic material and replicates using a DNA-dependent DNA polymerase. The nucleic acid is usually double-stranded DNA (dsDNA) but may also be single-stranded DNA (ssDNA).
R Gene are genes in plant genomes that convey plant disease resistance against pathogens by producing R proteins.
Bacterial DNA
Bacteria provide immunity against giant viruses. Chlamydia protect protozoa from deadly viral infections. Amoebae receive surprising support in defense against viruses. The bacteria they are infected with prevent them from being destroyed by giant viruses. Microbiologists have investigated how a virus infection proceeds when the amoebae are simultaneously infected with chlamydia. The research team shows for the first time that intracellular bacteria known as symbionts protect their host against viruses. Amoebae are protists, i.e. single-celled microorganisms with a cell nucleus. Protists play a key role in food webs and ecosystem processes. Consequently, the results of the study suggest that the interaction between symbionts and viruses influence the flow of nutrients in ecosystems.
Dangerous Amoebas are Spreading Globally. Scientists are warning that a little-known group of microbes called free-living amoebae may pose a growing global health threat. Found in soil and water, some species can survive extreme heat, chlorine, and even modern water systems—conditions that kill most germs. One infamous example, the “brain-eating amoeba,” can cause deadly infections after contaminated water enters the nose. Even more concerning, these amoebae can act as hiding places for dangerous bacteria and viruses, helping them evade disinfection and spread. A team explains that these microscopic organisms are gaining ground worldwide, driven by climate change, deteriorating water systems, and limited monitoring and detection efforts. The researchers also point out that amoebae can act as protective hosts for other disease-causing microbes. Bacteria and viruses can survive inside amoebae, shielded from disinfection processes that would normally eliminate them. This so called Trojan horse effect allows harmful pathogens to persist and spread through drinking water systems and may also play a role in the rise of antibiotic resistance.
Plasmid is a small DNA molecule within a cell that is physically separated from a chromosomal DNA and can replicate independently. They are most commonly found in bacteria as small circular, double-stranded DNA molecules; however, plasmids are sometimes present in archaea and eukaryotic organisms. In nature, plasmids often carry genes that may benefit the survival of the organism, for example antibiotic resistance. While the chromosomes are big and contain all the essential genetic information for living under normal conditions, plasmids usually are very small and contain only additional genes that may be useful to the organism under certain situations or particular conditions. Artificial plasmids are widely used as vectors in molecular cloning, serving to drive the replication of recombinant DNA sequences within host organisms.
The Role of Plasmids
Malaise is a feeling of general discomfort, uneasiness or pain, often the first indication of an infection or other disease.
Vaccine Dangers - Antibiotics - Travel Health Advice
Repeated infections associated with increased risk of some neurodegenerative diseases. People with hospital-treated infections in early- and mid-life had the greatest risk of Alzheimer's and Parkinson's diseases later in life.
World Health Organization - Center For Disease Control (CDC) - Infectious Diseases Emergency Preparedness Plan.
Biosecurity is a set of preventive measures designed to reduce the risk of transmission of infectious diseases in crops and livestock, quarantined pests, invasive alien species, and living modified organisms.
Disease Outbreaks - Virus Outbreaks Map - Antibody-Based Protection HIV - Aids - Colds
ZMapp is an experimental biopharmaceutical drug comprising three chimeric monoclonal antibodies under development as a treatment for Ebola virus disease.
Monoclonal Antibody - Hospital Infections
Engineered Bacteria Target Antibiotic-Resistant Pathogens
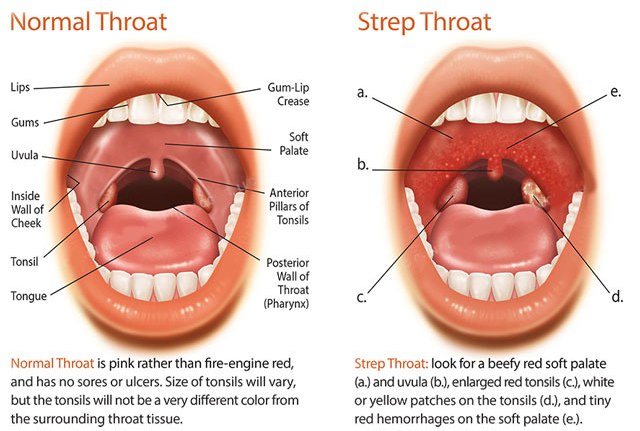 Otorhinolaryngology is a surgical subspecialty within medicine that
deals with conditions of the ear, nose, and throat
or ENT and related structures of the head and neck. Doctors who specialize
in this area are called otorhinolaryngologists, otolaryngologists, ENT
doctors, ENT surgeons, or head and neck surgeons. Patients seek treatment
from an otorhinolaryngologist for diseases of the ear, nose, throat, base
of the skull, and for the surgical management of cancers and benign tumors of the head and neck.
Otorhinolaryngology is a surgical subspecialty within medicine that
deals with conditions of the ear, nose, and throat
or ENT and related structures of the head and neck. Doctors who specialize
in this area are called otorhinolaryngologists, otolaryngologists, ENT
doctors, ENT surgeons, or head and neck surgeons. Patients seek treatment
from an otorhinolaryngologist for diseases of the ear, nose, throat, base
of the skull, and for the surgical management of cancers and benign tumors of the head and neck.
Serology is the scientific study of serum and other bodily fluids. In practice, the term usually refers to the diagnostic identification of antibodies in the serum. Such antibodies are typically formed in response to an infection (against a given microorganism), against other foreign proteins (in response, for example, to a mismatched blood transfusion), or to one's own proteins (in instances of autoimmune disease).
Researchers develop a novel antibiotic cement to treat bone infections. Specialized drug-device delivery system demonstrates high efficacy, potency against resistant strains, and promises decreased bacterial resistance development. Each year, 700,000 people die due to antibiotic resistance. A growing global population unfortunately generates a growing resistance to established antibiotic treatments -- a threat that has been met with insufficient funding and dwindling inspiration, as commercial incentives for developing new antibiotics have fallen. A new study addresses this growing problem in antibiotic development using a novel, interdisciplinary approach to construct a robust, computer-program-generated library of antibiotics and to identify an effective antibiotic for targeted use in a bone cement matrix.
Immune System can effect Social Behavior - Interferon Gamma is a cytokine that is critical for innate and adaptive immunity against viral, some bacterial and protozoal infections.
Cytokine is important in cell signaling. Their release has an effect on the behavior of cells around them. It can be said that cytokines are involved in autocrine signalling, paracrine signalling and endocrine signalling as immunomodulating agents. Their definite distinction from hormones is still part of ongoing research. Cytokines include chemokines, interferons, interleukins, lymphokines, and tumour necrosis factors but generally not hormones or growth factors (despite some overlap in the terminology). Cytokines are produced by a broad range of cells, including immune cells like macrophages, B lymphocytes, T lymphocytes and mast cells, as well as endothelial cells, fibroblasts, and various stromal cells; a given cytokine may be produced by more than one type of cell. They act through receptors, and are especially important in the immune system; cytokines modulate the balance between humoral and cell-based immune responses, and they regulate the maturation, growth, and responsiveness of particular cell populations. Some cytokines enhance or inhibit the action of other cytokines in complex ways. They are different from hormones, which are also important cell signaling molecules, in that hormones circulate in less variable concentrations and hormones tend to be made by specific kinds of cells. They are important in health and disease, specifically in host responses to infection, immune responses, inflammation, trauma, sepsis, cancer, and reproduction. Cytokine are a broad and loose category of small proteins (~5–20 kDa) that are important in cell signaling. Their release has an effect on the behavior of cells around them. It can be said that cytokines are involved in autocrine signalling, paracrine signalling and endocrine signalling as immunomodulating agents. Their definite distinction from hormones is still part of ongoing research. Cytokines include chemokines, interferons, interleukins, lymphokines, and tumour necrosis factors but generally not hormones or growth factors (despite some overlap in the terminology). Cytokines are produced by a broad range of cells, including immune cells like macrophages, B lymphocytes, T lymphocytes and mast cells, as well as endothelial cells, fibroblasts, and various stromal cells; a given cytokine may be produced by more than one type of cell. They act through receptors, and are especially important in the immune system; cytokines modulate the balance between humoral and cell-based immune responses, and they regulate the maturation, growth, and responsiveness of particular cell populations. Some cytokines enhance or inhibit the action of other cytokines in complex ways. They are different from hormones, which are also important cell signaling molecules, in that hormones circulate in less variable concentrations and hormones tend to be made by specific kinds of cells. They are important in health and disease, specifically in host responses to infection, immune responses, inflammation, trauma, sepsis, cancer, and reproduction.
 Interferon are a
group of signaling proteins
made and released by host cells in response to the presence of several
pathogens, such as viruses, bacteria, parasites, and also tumor cells. In
a typical scenario, a virus-infected cell will release interferons causing
nearby cells to heighten their anti-viral defenses.
IFNs belong to the large class of proteins known as cytokines, molecules
used for communication between cells to trigger the protective defenses of
the immune system that help eradicate pathogens. Interferons are named for
their ability to "interfere" with viral replication by protecting cells
from virus infections. IFNs also have various other functions: they
activate immune cells, such as natural killer cells and macrophages; they
increase host defenses by up-regulating antigen presentation by virtue of
increasing the expression of major histocompatibility complex (MHC)
antigens. Certain symptoms of infections, such as fever, muscle pain and
"flu-like symptoms", are also caused by the production of IFNs and other
cytokines. More than twenty distinct IFN genes and proteins have been
identified in animals, including humans. They are typically divided among
three classes: Type I IFN, Type II IFN, and Type III IFN. IFNs belonging
to all three classes are important for fighting viral infections and for
the regulation of the immune system.
Interferon are a
group of signaling proteins
made and released by host cells in response to the presence of several
pathogens, such as viruses, bacteria, parasites, and also tumor cells. In
a typical scenario, a virus-infected cell will release interferons causing
nearby cells to heighten their anti-viral defenses.
IFNs belong to the large class of proteins known as cytokines, molecules
used for communication between cells to trigger the protective defenses of
the immune system that help eradicate pathogens. Interferons are named for
their ability to "interfere" with viral replication by protecting cells
from virus infections. IFNs also have various other functions: they
activate immune cells, such as natural killer cells and macrophages; they
increase host defenses by up-regulating antigen presentation by virtue of
increasing the expression of major histocompatibility complex (MHC)
antigens. Certain symptoms of infections, such as fever, muscle pain and
"flu-like symptoms", are also caused by the production of IFNs and other
cytokines. More than twenty distinct IFN genes and proteins have been
identified in animals, including humans. They are typically divided among
three classes: Type I IFN, Type II IFN, and Type III IFN. IFNs belonging
to all three classes are important for fighting viral infections and for
the regulation of the immune system. Interferon-Stimulated Gene is a gene that can be expressed in response to stimulation by interferon. Interferons bind to receptors on the surface of a cell, initiating protein signaling pathways within the cell. This interaction leads to the expression of a subset of genes involved in the innate immune system response. ISGs are commonly expressed in response to viral infection, but also during bacterial infection and in the presence of parasites.
Scientists have identified a set of human genes that fight SARS-CoV-2 infection, the virus that causes COVID-19. We found that 65 interferon-stimulated genes controlled SARS-CoV-2 infection, including some that inhibited the virus' ability to enter cells, some that suppressed manufacture of the RNA that is the virus's lifeblood, and a cluster of genes that inhibited assembly of the virus.
Super Immunity - Exemptions - Corona Virus
The common cold might protect you from coronavirus. Interferons are produced in response to infections by all types of viruses, but they’re produced much faster and in greater quantities in response to rhinovirus compared to other respiratory viruses.
Besides SARS-CoV-2, there are four other coronaviruses in widespread circulation: NL63, 229E, OC43 and HKU1. The first two have likely been infecting people for centuries, and the latter two for decades, perhaps longer. They're related to SARS-CoV-2 but are not the same. Each year, one or more of these other coronaviruses sweeps through the U.S. — in schools, day care centers, churches and offices — and makes people sick. Many, many people. These coronaviruses are so common that by the time a child starts kindergarten, the youngster has likely been infected with all four of them. these coronaviruses cause about 10% to 30% of all colds in adults, studies have found. Here's the sneaky thing about these coronaviruses: Just because you caught one of them last year doesn't mean you're protected from that same coronavirus infection the next year. Having higher antibody levels prevented people from developing symptoms altogether and shortened the time they spread the virus.
Human Rhinovirus Infection Blocks Severe Acute Respiratory Syndrome Coronavirus 2 Replication Within the Respiratory Epithelium: Implications for COVID-19 Epidemiology. We show that human rhinovirus triggers an interferon response that blocks SARS-CoV-2 replication. Mathematical simulations show that this virus-virus interaction is likely to have a population-wide effect as an increasing prevalence of rhinovirus will reduce the number of new coronavirus disease 2019 cases.
Why do some people never show symptoms when infected with covid-19? Why are some people more vulnerable to covd-19?
Gene mutation may explain why some don't get sick from COVID-19. People who contract COVID-19 but never develop symptoms -- the so-called super dodgers -- may have a genetic ace up their sleeve. They're more than twice as likely as those who become symptomatic to carry a specific gene variation that helps them obliterate the virus, according to a new study. The secret lies with the human leukocyte antigen, or protein markers that signal the immune system. A mutation in one of the genes coding for HLA appears to help virus-killing T cells identify SARS-CoV-2 and launch a lighting attack. The T cells of some people who carry this variant can identify the novel coronavirus, even if they have never encountered it before, thanks to its resemblance to the seasonal cold viruses they already know. The mutation -- HLA-B*15:01 -- is quite common, carried by about 10% of the study's population. It doesn't prevent the virus from infecting cells but, rather, prevents people from developing any symptoms. That includes a runny nose or even a barely noticeable sore throat. UCSF researchers found that 20% of people in the study who remained asymptomatic after infection carried at least one copy of the HLA-B*15:01 variant, compared to 9% of those who reported symptoms. Those who carried two copies of the variant were far more likely -- more than eight times -- to avoid feeling sick.
Why are some people immune to covid-19? Some people, even before being vaccinated, are really good at clearing the coronavirus from their respiratory tract and do it so quickly that the virus never reaches detectable levels. Exposure to another coronavirus could be protecting people against SARS-CoV-2. A study presented striking evidence that prior exposure to another coronavirus can prepare the immune system to fight off SARS-CoV-2. Immune cells originally made to fight another coronavirus can help with immunity. An analysis from the Centers for Disease Control and Prevention found that at least 58% of children under age 18 — that's about 42 million children — had been infected with SARS-CoV-2 as of Jan. 22, according to antibody testing. Yet the U.S. has recorded only about 13 million pediatric cases. So many coronavirus cases among kids have gone unnoticed, unreported or undetected. During the first wave of the pandemic, when vaccines weren't available, healthcare workers repeatedly tested negative for SARS-CoV-2 despite being heavily exposed. Inside the blood of 20 health care workers, a team found a special group of T cells that could do just that, recognize and stop SARS-CoV-2. These special cells are called cross-reactive T cells. The cells are called cross-reactive because they recognize several types of coronaviruses. So just like cross-training involves several sports, cross-reactive cells work on several different viruses. Estimates about these cross-reactive T cells occur in only 10% to 15% of people. First, antibodies come in and protect you against infection, and then T cells help clean up the infected cells. T cells aren't the only immune component that can do this cross-reacting. Antibodies made to fight off seasonal coronavirus can also recognize SARS-CoV-2. Evidence that the immune system brings these seasonal coronavirus antibodies back into action when you're exposed to SARS-CoV-2. Even if a persons immune system doesn't have cross-reactive antibodies or cross-reactive T cells to protect her from SARS-CoV-2, there's a 100% guarantee that a person has another protective device. It's called the RIG-I pathway. Inside your respiratory cells, tiny molecules, called RIG-I receptors, recognize and bind to a virus's genome (specifically its RNA). Once a RIG-I receptor sticks to a piece of viral RNA, it launches a massive immune response. It tries to limit the viral infection as well as warn its neighbors so other cells can also go into an antiviral response, and not get infected too. This response kills the infected cell, protects surrounding cells from infection and possibly brings in immune cells (like T cells) to help control the infection. There's evidence the RIG-I pathway can clear out a SARS-CoV-2 infection before viral loads reach detectable levels or the immune system even has a chance to make antibodies. Children have more RIG-I receptors inside their nasal cells. And this higher concentration helps them respond more quickly to an infection. But in a study, the T cells appear at a very early stage of the infection, before the body can make antibodies. In contrast, in blood samples taken from health care workers who did test positive for SARS-CoV-2, these cross-reactive T cells were missing or present at much lower levels. People who had higher levels of these cross-reactive T cells at the baseline didn't get infected, versus the group who didn't. These special T cells likely arose in the health care workers before the pandemic began. Their immune systems likely generated them when the workers were infected with another of the several coronaviruses that can strike humans. Most likely candidate would be the common cold coronaviruses that we're all exposed to. About 30% of colds are caused by four other coronaviruses known as seasonal coronaviruses (because they typically come around in winter and cause winter colds). These viruses circulate around the world and have been making people sick for decades, perhaps even centuries. Basically, every kid catches all four of them before age 5 or 6. Even though these seasonal coronaviruses typically don't cause more than a runny nose and cough, your body still has to clear out the virus to prevent it from turning into a more serious problem. To do that, the immune system makes antibodies and T cells that recognize these coronaviruses. Some of these T cells stick around and watch out for the virus, or a similar one to return again. Long Covid.
Miracle Mineral Solution or MMS has long been promoted as a miracle cure, but new research shows it’s essentially a toxic disinfectant. While it can kill bacteria, it only works at levels that also damage human cells and beneficial gut microbes. Scientists warn that homemade MMS mixtures are especially dangerous due to wildly inconsistent dosing. The study calls MMS a clear case where the risks are high—and the benefits are effectively zero.
